Issue published April 1, 2020 Previous issue | Next issue

On the cover: IFN-driven neuroinflammation in Alzheimer disease
Pathologic inflammation leading to neurodegeneration in Alzheimer disease (AD) may be driven by immunogenic responses to β-amyloid (Aβ) fibrils, aggregates of soluble proteins that form insoluble secondary structures. In this issue of the JCI, Roy et al. highlight the IFN pathway’s contribution to neuropathology in models of AD. They reveal that Aβ-driven activation of IFN signaling in microglia drives microgliosis as well as complement-mediated synapse loss in mice. Blocking IFN reduced inflammation and synapse loss in these models. Together, the observations support further examination of the IFN pathway as a target in treating AD. The accompanying image shows the accumulation of activated microglia (Iba1, green; Clec7a, yellow) associated with Aβ plaques (blue) in a mouse model of AD. Image credit: Ethan Roy.
-
Viewpoints
×
Abstract
Authors
Arturo Casadevall, Liise-anne Pirofski
-
Review Series
×
Abstract
In spite of the recent approval of new promising targeted therapies, the clinical outcome of patients with acute myeloid leukemia (AML) remains suboptimal, prompting the search for additional and synergistic therapeutic rationales. It is increasingly evident that the bone marrow immune environment of AML patients is profoundly altered, contributing to the severity of the disease but also providing several windows of opportunity to prompt or rewire a proficient antitumor immune surveillance. In this Review, we present current evidence on immune defects in AML, discuss the challenges with selective targeting of AML cells, and summarize the clinical results and immunologic insights from studies that are testing the latest immunotherapy approaches to specifically target AML cells (antibodies, cellular therapies) or more broadly reactivate antileukemia immunity (vaccines, checkpoint blockade). Given the complex interactions between AML cells and the many components of their environment, it is reasonable to surmise that the future of immunotherapy in AML lies in the rational combination of complementary immunotherapeutic strategies with chemotherapeutics or other oncogenic pathway inhibitors. Identifying reliable biomarkers of response to improve patient selection and avoid toxicities will be critical in this process.
Authors
Luca Vago, Ivana Gojo
×Abstract
Multiple myeloma (MM), a bone marrow–resident hematological malignancy of plasma cells, has remained largely incurable despite dramatic improvements in patient outcomes in the era of myeloma-targeted and immunomodulatory agents. It has recently become clear that T cells from MM patients are able to recognize and eliminate myeloma, although this is subverted in the majority of patients who eventually succumb to progressive disease. T cell exhaustion and a suppressive bone marrow microenvironment have been implicated in disease progression, and once these are established, immunotherapy appears largely ineffective. Autologous stem cell transplantation (ASCT) is a standard of care in eligible patients and results in immune effects beyond cytoreduction, including lymphodepletion, T cell priming via immunogenic cell death, and inflammation; all occur within the context of a disrupted bone marrow microenvironment. Recent studies suggest that ASCT reestablishes immune equilibrium and thus represents a logical platform in which to intervene to prevent immune escape. New immunotherapies based on checkpoint inhibition targeting the immune receptor TIGIT and the deletion of suppressive myeloid populations appear attractive, particularly after ASCT. Finally, the immunologically favorable environment created after ASCT may also represent an opportunity for approaches utilizing bispecific antibodies or chimeric antigen receptor T cells.
Authors
Simone A. Minnie, Geoffrey R. Hill
×Abstract
Lymphoid malignancies typically promote an infiltrate of immune cells at sites involved by the disease. While some of the immune cells present in lymphoma have effector function, the immune system is unable to eradicate the malignant clone. Therapies that optimize immune function therefore have the potential to improve the outcome of lymphoma patients. In this Review, we discuss immunologic approaches that directly target the malignant cell as well as approaches to optimize both the innate and adaptive immune response to the tumor. While many of these therapies have shown single-agent activity, the future will clearly require thoughtful combinations of these approaches.
Authors
Stephen M. Ansell, Yi Lin
×Abstract
Cellular therapy for hematologic malignancies is a rapidly evolving field, with new iterations of novel constructs being developed at a rapid pace. Since the initial reports of chimeric antigen receptor T cell (CAR T cell)success in CD19+ B cell malignancies, multiple clinical trials of CAR T cell therapy directed to CD19 have led to the approval of this therapy by the FDA and the European Medicines Agency for specific indications. Despite strikingly similar efficacy, investigators at multiple centers participating in these studies have observed the nuances of each CAR T cell product, including variability in manufacturing, availability, and toxicity profiles. Here we review state-of-the-art clinical data on CD19-directed CAR T cell therapies in B cell hematologic malignancies, advances made in understanding and modeling associated toxicities, and several exciting advances and creative solutions for overcoming challenges with this therapeutic modality.
Authors
Matthew J. Frigault, Marcela V. Maus
×Abstract
Hematological malignancies have long been at the forefront of the development of novel immune-based treatment strategies. The earliest successful efforts originated from the extensive body of work in the field of allogeneic hematopoietic stem cell transplantation. These efforts laid the foundation for the recent exciting era of cancer immunotherapy, which includes immune checkpoint blockade, personal neoantigen vaccines, and adoptive T cell transfer. At the heart of the specificity of these novel strategies is the recognition of target antigens presented by malignant cells to T cells. Here, we review the advances in systematic identification of minor histocompatibility antigens and neoantigens arising from personal somatic alterations or recurrent driver mutations. These exciting efforts pave the path for the implementation of personalized combinatorial cancer therapy.
Authors
Livius Penter, Catherine J. Wu
-
Commentaries
×
Abstract
The cardiomyopathy of Duchenne muscular dystrophy (DMD) is an important cause of morbidity and mortality in affected males with this dreaded muscle disease. Previous studies have implicated changes in expression and subcellular localization of connexin-43 (Cx43), the major ventricular gap junction protein, in DMD cardiomyopathy. In this issue of the JCI, Himelman et al. explore how hypophosphorylation of Cx43 at a triplet of serine residues (S325/S328/S330) in the regulatory C-terminus contributes to multiple features of the cardiomyopathy phenotype. Using a mouse model of DMD cardiomyopathy in which phosphomimetic glutamic acids are substituted for serines at these residues in Cx43, Himelman et al. observed reduced gap junction remodeling and lateralization of Cx43 immunosignals, protection against isoproterenol-induced arrhythmias, and improved Ca2+ homeostasis. This study contributes to the understanding of pathologic Cx43 remodeling and encourages further research into developing strategic interventions to mitigate cardiac dysfunction and arrhythmias in DMD patients.
Authors
Robin M. Shaw, Jeffrey E. Saffitz
×Abstract
Currently, the incidence of HIV infection exceeds the death rate from HIV, and as a result, the prevalence of individuals living with the infection continues to increase. A critical limitation preventing the development of curative strategies is the lack of knowledge regarding mechanisms that allow HIV-infected cells to persist in individuals during combination antiviral therapy (ART). In this issue of the JCI, Chaillon and coworkers assessed HIV-infected cells from various anatomic compartments obtained through a rapid autopsy program of individuals undergoing long-term ART. This study, made possible with strong community collaboration, provides new insights on the potential locations of reservoirs of HIV-infected cells that persist during therapy.
Authors
Frank Maldarelli
×Abstract
Parathyroid hormone (PTH) has complex effects on bone, including stimulating bone formation and regulating the hematopoietic stem cell (HSC) niche. In the current issue of the JCI, Li et al. demonstrated that the microbiome, through the production of short-chain fatty acids and in particular, butyrate, is necessary for the ability of PTH to increase osteoblast numbers and stimulate bone formation. In addition to implications for the treatment of osteoporosis with PTH analogs, this pathway may be part of a broader mechanism through which the microbiome serves its key function of modulating the immune system.
Authors
Sundeep Khosla
×Abstract
Tregs require specific epigenetic signatures to induce and maintain their suppressive function in the context of inflammation and cancer surveillance. In this issue of the JCI, Xiong and colleagues identify a critical role for the epigenetic repressor REST corepressor 1 (CoREST) in promoting Treg suppressive transcriptional and functional programs. Pharmacologic inhibition and genetic loss of CoREST in Tregs impaired organ allograft tolerance and unleashed antitumor immunity via epigenetic activation of effector T cell programs. We propose that exploiting epigenetic control mechanisms will further the translation of Treg-based therapeutics to target inflammatory and malignant disorders.
Authors
Luisa Morales-Nebreda, Kathryn A. Helmin, Benjamin D. Singer
×Abstract
β-Amyloid aggregates found in brain plaques are viewed as triggers of cytotoxicity and neuroinflammation in Alzheimer disease (AD). However, the main β-amyloid (Aβ) species and what imbues the aggregates with such toxic potential are still not yet understood. In this issue of the JCI, Roy et al. show that Aβ complexed with nucleic acids triggers an antiviral type I interferon response in neuroglia, resulting in complement-mediated synapse elimination in AD models. These findings identify a putative endogenous immune signaling axis that drives neurodegeneration in AD and has strong implications for the development of precise therapeutic strategies.
Authors
Stefano Pluchino, Cory Willis
×Abstract
Chronic graft-versus-host disease (GVHD) is a major complication of allogeneic hematopoietic cell transplantation that resembles autoimmunity, with unclear pathogenesis and few effective therapeutic options. In this issue of the JCI, Dertschnig et al. used mouse models to investigate the basis of T cell autoreactivity following GVHD. Notably, GVHD caused irreversible damage to a population of tolerogenic stromal cells that display peripheral tissue–restricted antigens in lymph nodes, which impaired their capacity to purge and suppress autoreactive T cells. Together with damage to central tolerance mechanisms in the thymus, these findings outline a critical one-two punch injury that profoundly disrupts immune tolerance in this devastating disease.
Authors
Léolène J. Carrington, Ivan Maillard
×Abstract
Tumor-associated macrophages (TAMs) represent the most abundant hematopoietic cell type in the solid tumor microenvironment. TAMs drive T cell inhibition, promote angiogenesis, and produce tumor growth factors. Although they can paradoxically exert antitumor activity and prime protective immunity, the pathways driving this phenotype remain unclear. In this issue of the JCI, Liu and colleagues identified the c-Maf transcription factor as a master regulator of protumoral TAM polarization. The authors found that c-Maf promoted TAMs’ immunosuppressive activity, governed their metabolic programming, and drove expression of the macrophage differentiation protein, CSF1R. Further, inhibiting c-Maf in myeloid progenitors, and consequent myeloid-lineage cells, including TAMs, delayed tumor growth. Importantly, β-glucan treatment reduced c-MAF expression in macrophages and monocytes from patients with non–small cell lung cancer (NSCLC) where c-MAF is overexpressed. These results reveal mechanisms whereby myeloid cells drive human cancer progression by thwarting protective immunity and could lead to immunotherapy for most solid malignancies.
Authors
Jose R. Conejo-Garcia, Paulo C. Rodriguez
×Abstract
Cystic fibrosis (CF) is a multisystem disorder, but progressive inflammatory lung disease causes the greatest burden of morbidity and death. Recent translational and mechanistic studies of samples from patients, and observations in animal models, indicate that platelets may drive lung injury and contribute to dysregulated host defense in CF lung disease. In this issue of the JCI, Ortiz-Muñoz and Yu et al. explored the role that the cystic fibrosis transmembrane conductance regulator (CFTR) plays in platelet-related inflammation. The authors used mouse and human model systems to show that CFTR dysfunction in platelets increased calcium entry though the transient receptor potential cation channel 6 (TRPC6), causing hyperactivation and consequent experimental lung inflammation. The study persuasively suggests that platelets are critical thromboinflammatory effector cells in CF lung disease. In the context of platelet-related organ injury seen in a variety of other diseases and syndromes, platelets may also contribute to nonpulmonary manifestations and comorbidities of CF.
Authors
Guy A. Zimmerman
-
Research Articles
Xiaobo Luo, Christopher R. Donnelly, Wang Gong, Blake R. Heath, Yuning Hao, Lorenza A. Donnelly, Toktam Moghbeli, Yee Sun Tan, Xin Lin, Emily Bellile, Benjamin A. Kansy, Thomas E. Carey, J. Chad Brenner, Lei Cheng, Peter J. Polverini, Meredith A. Morgan, Haitao Wen, Mark E. Prince, Robert L. Ferris, Yuying Xie, Simon Young, Gregory T. Wolf, Qianming Chen, Yu L. LeiXiaobo Luo, Christopher R. Donnelly, Wang Gong, Blake R. Heath, Yuning Hao, Lorenza A. Donnelly, Toktam Moghbeli, Yee Sun Tan, Xin Lin, Emily Bellile, Benjamin A. Kansy, Thomas E. Carey, J. Chad Brenner, Lei Cheng, Peter J. Polverini, Meredith A. Morgan, Haitao Wen, Mark E. Prince, Robert L. Ferris, Yuying Xie, Simon Young, Gregory T. Wolf, Qianming Chen, Yu L. Lei×
Abstract
The incidence of human papillomavirus–positive (HPV+) head and neck squamous cell carcinoma (HNSCC) has surpassed that of cervical cancer and is projected to increase rapidly until 2060. The coevolution of HPV with transforming epithelial cells leads to the shutdown of host immune detection. Targeting proximal viral nucleic acid–sensing machinery is an evolutionarily conserved strategy among viruses to enable immune evasion. However, E7 from the dominant HPV subtype 16 in HNSCC shares low homology with HPV18 E7, which was shown to inhibit the STING DNA-sensing pathway. The mechanisms by which HPV16 suppresses STING remain unknown. Recently, we characterized the role of the STING/type I interferon (IFN-I) pathway in maintaining immunogenicity of HNSCC in mouse models. Here we extended those findings into the clinical domain using tissue microarrays and machine learning–enhanced profiling of STING signatures with immune subsets. We additionally showed that HPV16 E7 uses mechanisms distinct from those used by HPV18 E7 to antagonize the STING pathway. We identified NLRX1 as a critical intermediary partner to facilitate HPV16 E7–potentiated STING turnover. The depletion of NLRX1 resulted in significantly improved IFN-I–dependent T cell infiltration profiles and tumor control. Overall, we discovered a unique HPV16 viral strategy to thwart host innate immune detection that can be further exploited to restore cancer immunogenicity.
Authors
Xiaobo Luo, Christopher R. Donnelly, Wang Gong, Blake R. Heath, Yuning Hao, Lorenza A. Donnelly, Toktam Moghbeli, Yee Sun Tan, Xin Lin, Emily Bellile, Benjamin A. Kansy, Thomas E. Carey, J. Chad Brenner, Lei Cheng, Peter J. Polverini, Meredith A. Morgan, Haitao Wen, Mark E. Prince, Robert L. Ferris, Yuying Xie, Simon Young, Gregory T. Wolf, Qianming Chen, Yu L. Lei
Himisha Beltran, Alessandro Romanel, Vincenza Conteduca, Nicola Casiraghi, Michael Sigouros, Gian Marco Franceschini, Francesco Orlando, Tarcisio Fedrizzi, Sheng-Yu Ku, Emma Dann, Alicia Alonso, Juan Miguel Mosquera, Andrea Sboner, Jenny Xiang, Olivier Elemento, David M. Nanus, Scott T. Tagawa, Matteo Benelli, Francesca DemichelisHimisha Beltran, Alessandro Romanel, Vincenza Conteduca, Nicola Casiraghi, Michael Sigouros, Gian Marco Franceschini, Francesco Orlando, Tarcisio Fedrizzi, Sheng-Yu Ku, Emma Dann, Alicia Alonso, Juan Miguel Mosquera, Andrea Sboner, Jenny Xiang, Olivier Elemento, David M. Nanus, Scott T. Tagawa, Matteo Benelli, Francesca Demichelis×Abstract
Loss of androgen receptor (AR) signaling dependence occurs in approximately 15%–20% of advanced treatment-resistant prostate cancers, and this may manifest clinically as transformation from a prostate adenocarcinoma histology to a castration-resistant neuroendocrine prostate cancer (CRPC-NE). The diagnosis of CRPC-NE currently relies on a metastatic tumor biopsy, which is invasive for patients and sometimes challenging to diagnose due to morphologic heterogeneity. By studying whole-exome sequencing and whole-genome bisulfite sequencing of cell free DNA (cfDNA) and of matched metastatic tumor biopsies from patients with metastatic prostate adenocarcinoma and CRPC-NE, we identified CRPC-NE features detectable in the circulation. Overall, there was markedly higher concordance between cfDNA and biopsy tissue genomic alterations in patients with CRPC-NE compared with castration-resistant adenocarcinoma, supporting greater intraindividual genomic consistency across metastases. Allele-specific copy number and serial sampling analyses allowed for the detection and tracking of clonal and subclonal tumor cell populations. cfDNA methylation was indicative of circulating tumor content fraction, reflective of methylation patterns observed in biopsy tissues, and was capable of detecting CRPC-NE–associated epigenetic changes (e.g., hypermethylation of ASXL3 and SPDEF; hypomethylation of INSM1 and CDH2). A targeted set combining genomic (TP53, RB1, CYLD, AR) and epigenomic (hypo- and hypermethylation of 20 differential sites) alterations applied to ctDNA was capable of identifying patients with CRPC-NE.
Authors
Himisha Beltran, Alessandro Romanel, Vincenza Conteduca, Nicola Casiraghi, Michael Sigouros, Gian Marco Franceschini, Francesco Orlando, Tarcisio Fedrizzi, Sheng-Yu Ku, Emma Dann, Alicia Alonso, Juan Miguel Mosquera, Andrea Sboner, Jenny Xiang, Olivier Elemento, David M. Nanus, Scott T. Tagawa, Matteo Benelli, Francesca Demichelis
×Abstract
BACKGROUND Undifferentiated systemic autoinflammatory diseases (USAIDs) present diagnostic and therapeutic challenges. Chronic interferon (IFN) signaling and cytokine dysregulation may identify diseases with available targeted treatments.METHODS Sixty-six consecutively referred USAID patients underwent underwent screening for the presence of an interferon signature using a standardized type-I IFN-response-gene score (IRG-S), cytokine profiling, and genetic evaluation by next-generation sequencing.RESULTS Thirty-six USAID patients (55%) had elevated IRG-S. Neutrophilic panniculitis (40% vs. 0%), basal ganglia calcifications (46% vs. 0%), interstitial lung disease (47% vs. 5%), and myositis (60% vs. 10%) were more prevalent in patients with elevated IRG-S. Moderate IRG-S elevation and highly elevated serum IL-18 distinguished 8 patients with pulmonary alveolar proteinosis (PAP) and recurrent macrophage activation syndrome (MAS). Among patients with panniculitis and progressive cytopenias, 2 patients were compound heterozygous for potentially novel LRBA mutations, 4 patients harbored potentially novel splice variants in IKBKG (which encodes NF-κB essential modulator [NEMO]), and 6 patients had de novo frameshift mutations in SAMD9L. Of additional 12 patients with elevated IRG-S and CANDLE-, SAVI- or Aicardi-Goutières syndrome–like (AGS-like) phenotypes, 5 patients carried mutations in either SAMHD1, TREX1, PSMB8, or PSMG2. Two patients had anti-MDA5 autoantibody–positive juvenile dermatomyositis, and 7 could not be classified. Patients with LRBA, IKBKG, and SAMD9L mutations showed a pattern of IRG elevation that suggests prominent NF-κB activation different from the canonical interferonopathies CANDLE, SAVI, and AGS.CONCLUSIONS In patients with elevated IRG-S, we identified characteristic clinical features and 3 additional autoinflammatory diseases: IL-18–mediated PAP and recurrent MAS (IL-18PAP-MAS), NEMO deleted exon 5–autoinflammatory syndrome (NEMO-NDAS), and SAMD9L-associated autoinflammatory disease (SAMD9L-SAAD). The IRG-S expands the diagnostic armamentarium in evaluating USAIDs and points to different pathways regulating IRG expression.TRIAL REGISTRATION ClinicalTrials.gov NCT02974595.FUNDING The Intramural Research Program of the NIH, NIAID, NIAMS, and the Clinical Center.
Authors
Adriana A. de Jesus, Yangfeng Hou, Stephen Brooks, Louise Malle, Angelique Biancotto, Yan Huang, Katherine R. Calvo, Bernadette Marrero, Susan Moir, Andrew J. Oler, Zuoming Deng, Gina A. Montealegre Sanchez, Amina Ahmed, Eric Allenspach, Bita Arabshahi, Edward Behrens, Susanne Benseler, Liliana Bezrodnik, Sharon Bout-Tabaku, AnneMarie C. Brescia, Diane Brown, Jon M. Burnham, Maria Soledad Caldirola, Ruy Carrasco, Alice Y. Chan, Rolando Cimaz, Paul Dancey, Jason Dare, Marietta DeGuzman, Victoria Dimitriades, Ian Ferguson, Polly Ferguson, Laura Finn, Marco Gattorno, Alexei A. Grom, Eric P. Hanson, Philip J. Hashkes, Christian M. Hedrich, Ronit Herzog, Gerd Horneff, Rita Jerath, Elizabeth Kessler, Hanna Kim, Daniel J. Kingsbury, Ronald M. Laxer, Pui Y. Lee, Min Ae Lee-Kirsch, Laura Lewandowski, Suzanne Li, Vibke Lilleby, Vafa Mammadova, Lakshmi N. Moorthy, Gulnara Nasrullayeva, Kathleen M. O’Neil, Karen Onel, Seza Ozen, Nancy Pan, Pascal Pillet, Daniela G.P. Piotto, Marilynn G. Punaro, Andreas Reiff, Adam Reinhardt, Lisa G. Rider, Rafael Rivas-Chacon, Tova Ronis, Angela Rösen-Wolff, Johannes Roth, Natasha Mckerran Ruth, Marite Rygg, Heinrike Schmeling, Grant Schulert, Christiaan Scott, Gisella Seminario, Andrew Shulman, Vidya Sivaraman, Mary Beth Son, Yuriy Stepanovskiy, Elizabeth Stringer, Sara Taber, Maria Teresa Terreri, Cynthia Tifft, Troy Torgerson, Laura Tosi, Annet Van Royen-Kerkhof, Theresa Wampler Muskardin, Scott W. Canna, Raphaela Goldbach-Mansky
Lindsay M. Webb, Shouvonik Sengupta, Claudia Edell, Zayda L. Piedra-Quintero, Stephanie A. Amici, Janiret Narvaez Miranda, Makenzie Bevins, Austin Kennemer, Georgios Laliotis, Philip N. Tsichlis, Mireia Guerau-de-ArellanoLindsay M. Webb, Shouvonik Sengupta, Claudia Edell, Zayda L. Piedra-Quintero, Stephanie A. Amici, Janiret Narvaez Miranda, Makenzie Bevins, Austin Kennemer, Georgios Laliotis, Philip N. Tsichlis, Mireia Guerau-de-Arellano×Abstract
Protein arginine methyltransferase 5 (PRMT5) catalyzes symmetric dimethylation (SDM) of arginine, a posttranslational modification involved in oncogenesis and embryonic development. However, the role and mechanisms by which PRMT5 modulates Th cell polarization and autoimmune disease have not yet been elucidated. Here, we found that PRMT5 promoted SREBP1 SDM and the induction of cholesterol biosynthetic pathway enzymes that produce retinoid-related orphan receptor (ROR) agonists that activate RORγt. Specific loss of PRMT5 in the CD4+ Th cell compartment suppressed Th17 differentiation and protected mice from developing experimental autoimmune encephalomyelitis (EAE). We also found that PRMT5 controlled thymic and peripheral homeostasis in the CD4+ Th cell life cycle and invariant NK (iNK) T cell development and CD8+ T cell maintenance. This work demonstrates that PRMT5 expression in recently activated T cells is necessary for the cholesterol biosynthesis metabolic gene expression program that generates RORγt agonistic activity and promotes Th17 differentiation and EAE. These results point to Th PRMT5 and its downstream cholesterol biosynthesis pathway as promising therapeutic targets in Th17-mediated diseases.
Authors
Lindsay M. Webb, Shouvonik Sengupta, Claudia Edell, Zayda L. Piedra-Quintero, Stephanie A. Amici, Janiret Narvaez Miranda, Makenzie Bevins, Austin Kennemer, Georgios Laliotis, Philip N. Tsichlis, Mireia Guerau-de-Arellano
Antoine Chaillon, Sara Gianella, Simon Dellicour, Stephen A. Rawlings, Timothy E. Schlub, Michelli Faria De Oliveira, Caroline Ignacio, Magali Porrachia, Bram Vrancken, Davey M. SmithAntoine Chaillon, Sara Gianella, Simon Dellicour, Stephen A. Rawlings, Timothy E. Schlub, Michelli Faria De Oliveira, Caroline Ignacio, Magali Porrachia, Bram Vrancken, Davey M. Smith×Abstract
BACKGROUND Understanding HIV dynamics across the human body is important for cure efforts. This goal has been hampered by technical difficulties and the challenge of obtaining fresh tissues.METHODS This observational study evaluated 6 individuals with HIV (n = 4 with viral suppression using antiretroviral [ART] therapy; n = 2 with rebound viremia after stopping ART), who provided serial blood samples before death and their bodies for rapid autopsy. HIV reservoirs were characterized by digital droplet PCR, single-genome amplification, and sequencing of full-length (FL) envelope HIV. Phylogeographic methods were used to reconstruct HIV spread, and generalized linear models were tested for viral factors associated with dispersal.RESULTS Across participants, HIV DNA levels varied from approximately 0 to 659 copies/106 cells (IQR: 22.9–126.5). A total of 605 intact FL env sequences were recovered in antemortem blood cells and across 28 tissues (IQR: 5–9). Sequence analysis showed (a) the emergence of large, identical, intact HIV RNA populations in blood after cessation of therapy, which repopulated tissues throughout the body; (b) that multiple sites acted as hubs for HIV dissemination but that blood and lymphoid tissues were the main source; (c) that viral exchanges occurred within brain areas and across the blood-brain barrier; and (d) that migration was associated with low HIV divergence between sites and greater diversity at the recipient site.CONCLUSION HIV reservoirs persisted in all deep tissues, and blood was the main source of dispersal. This may explain why eliminating HIV susceptibility in circulating T cells via bone marrow transplants allowed some individuals with HIV to experience therapy-free remission, even though deeper tissue reservoirs were not targeted.TRIAL REGISTRATION Not applicable.FUNDING NIH grants P01 AI31385, P30 AI036214, AI131971-01, AI120009AI036214, HD094646, AI027763, AI134295, and AI68636.
Authors
Antoine Chaillon, Sara Gianella, Simon Dellicour, Stephen A. Rawlings, Timothy E. Schlub, Michelli Faria De Oliveira, Caroline Ignacio, Magali Porrachia, Bram Vrancken, Davey M. Smith
Eric Himelman, Mauricio A. Lillo, Julie Nouet, J. Patrick Gonzalez, Qingshi Zhao, Lai-Hua Xie, Hong Li, Tong Liu, Xander H.T. Wehrens, Paul D. Lampe, Glenn I. Fishman, Natalia Shirokova, Jorge E. Contreras, Diego FraidenraichEric Himelman, Mauricio A. Lillo, Julie Nouet, J. Patrick Gonzalez, Qingshi Zhao, Lai-Hua Xie, Hong Li, Tong Liu, Xander H.T. Wehrens, Paul D. Lampe, Glenn I. Fishman, Natalia Shirokova, Jorge E. Contreras, Diego Fraidenraich×Abstract
Aberrant expression of the cardiac gap junction protein connexin-43 (Cx43) has been suggested as playing a role in the development of cardiac disease in the mdx mouse model of Duchenne muscular dystrophy (DMD); however, a mechanistic understanding of this association is lacking. Here, we identified a reduction of phosphorylation of Cx43 serines S325/S328/S330 in human and mouse DMD hearts. We hypothesized that hypophosphorylation of Cx43 serine-triplet triggers pathological Cx43 redistribution to the lateral sides of cardiomyocytes (remodeling). Therefore, we generated knockin mdx mice in which the Cx43 serine-triplet was replaced with either phospho-mimicking glutamic acids (mdxS3E) or nonphosphorylatable alanines (mdxS3A). The mdxS3E, but not mdxS3A, mice were resistant to Cx43 remodeling, with a corresponding reduction of Cx43 hemichannel activity. MdxS3E cardiomyocytes displayed improved intracellular Ca2+ signaling and a reduction of NADPH oxidase 2 (NOX2)/ROS production. Furthermore, mdxS3E mice were protected against inducible arrhythmias, related lethality, and the development of cardiomyopathy. Inhibition of microtubule polymerization by colchicine reduced both NOX2/ROS and oxidized CaMKII, increased S325/S328/S330 phosphorylation, and prevented Cx43 remodeling in mdx hearts. Together, these results demonstrate a mechanism of dystrophic Cx43 remodeling and suggest that targeting Cx43 may be a therapeutic strategy for preventing heart dysfunction and arrhythmias in DMD patients.
Authors
Eric Himelman, Mauricio A. Lillo, Julie Nouet, J. Patrick Gonzalez, Qingshi Zhao, Lai-Hua Xie, Hong Li, Tong Liu, Xander H.T. Wehrens, Paul D. Lampe, Glenn I. Fishman, Natalia Shirokova, Jorge E. Contreras, Diego Fraidenraich
Oakleigh M. Folkes, Rita Báldi, Veronika Kondev, David J. Marcus, Nolan D. Hartley, Brandon D. Turner, Jade K. Ayers, Jordan J. Baechle, Maya P. Misra, Megan Altemus, Carrie A. Grueter, Brad A. Grueter, Sachin PatelOakleigh M. Folkes, Rita Báldi, Veronika Kondev, David J. Marcus, Nolan D. Hartley, Brandon D. Turner, Jade K. Ayers, Jordan J. Baechle, Maya P. Misra, Megan Altemus, Carrie A. Grueter, Brad A. Grueter, Sachin Patel×Abstract
Deficits in social interaction (SI) are a core symptom of autism spectrum disorders (ASDs); however, treatments for social deficits are notably lacking. Elucidating brain circuits and neuromodulatory signaling systems that regulate sociability could facilitate a deeper understanding of ASD pathophysiology and reveal novel treatments for ASDs. Here we found that in vivo optogenetic activation of the basolateral amygdala–nucleus accumbens (BLA-NAc) glutamatergic circuit reduced SI and increased social avoidance in mice. Furthermore, we found that 2-arachidonoylglycerol (2-AG) endocannabinoid signaling reduced BLA-NAc glutamatergic activity and that pharmacological 2-AG augmentation via administration of JZL184, a monoacylglycerol lipase inhibitor, blocked SI deficits associated with in vivo BLA-NAc stimulation. Additionally, optogenetic inhibition of the BLA-NAc circuit markedly increased SI in the Shank3B–/– mouse, an ASD model with substantial SI impairment, without affecting SI in WT mice. Finally, we demonstrated that JZL184 delivered systemically or directly to the NAc also normalized SI deficits in Shank3B–/– mice, while ex vivo JZL184 application corrected aberrant NAc excitatory and inhibitory neurotransmission and reduced BLA-NAc–elicited feed-forward inhibition of NAc neurons in Shank3B–/– mice. These data reveal circuit-level and neuromodulatory mechanisms regulating social function relevant to ASDs and suggest 2-AG augmentation could reduce social deficits via modulation of excitatory and inhibitory neurotransmission in the NAc.
Authors
Oakleigh M. Folkes, Rita Báldi, Veronika Kondev, David J. Marcus, Nolan D. Hartley, Brandon D. Turner, Jade K. Ayers, Jordan J. Baechle, Maya P. Misra, Megan Altemus, Carrie A. Grueter, Brad A. Grueter, Sachin Patel
Joaquin Mateo, George Seed, Claudia Bertan, Pasquale Rescigno, David Dolling, Ines Figueiredo, Susana Miranda, Daniel Nava Rodrigues, Bora Gurel, Matthew Clarke, Mark Atkin, Rob Chandler, Carlo Messina, Semini Sumanasuriya, Diletta Bianchini, Maialen Barrero, Antonella Petermolo, Zafeiris Zafeiriou, Mariane Fontes, Raquel Perez-Lopez, Nina Tunariu, Ben Fulton, Robert Jones, Ursula McGovern, Christy Ralph, Mohini Varughese, Omi Parikh, Suneil Jain, Tony Elliott, Shahneen Sandhu, Nuria Porta, Emma Hall, Wei Yuan, Suzanne Carreira, Johann S. de BonoJoaquin Mateo, George Seed, Claudia Bertan, Pasquale Rescigno, David Dolling, Ines Figueiredo, Susana Miranda, Daniel Nava Rodrigues, Bora Gurel, Matthew Clarke, Mark Atkin, Rob Chandler, Carlo Messina, Semini Sumanasuriya, Diletta Bianchini, Maialen Barrero, Antonella Petermolo, Zafeiris Zafeiriou, Mariane Fontes, Raquel Perez-Lopez, Nina Tunariu, Ben Fulton, Robert Jones, Ursula McGovern, Christy Ralph, Mohini Varughese, Omi Parikh, Suneil Jain, Tony Elliott, Shahneen Sandhu, Nuria Porta, Emma Hall, Wei Yuan, Suzanne Carreira, Johann S. de Bono×Abstract
The genomics of primary prostate cancer differ from those of metastatic castration-resistant prostate cancer (mCRPC). We studied genomic aberrations in primary prostate cancer biopsies from patients who developed mCRPC, also studying matching, same-patient, diagnostic, and mCRPC biopsies following treatment. We profiled 470 treatment-naive prostate cancer diagnostic biopsies and, for 61 cases, mCRPC biopsies, using targeted and low-pass whole-genome sequencing (n = 52). Descriptive statistics were used to summarize mutation and copy number profile. Prevalence was compared using Fisher’s exact test. Survival correlations were studied using log-rank test. TP53 (27%) and PTEN (12%) and DDR gene defects (BRCA2 7%; CDK12 5%; ATM 4%) were commonly detected. TP53, BRCA2, and CDK12 mutations were markedly more common than described in the TCGA cohort. Patients with RB1 loss in the primary tumor had a worse prognosis. Among 61 men with matched hormone-naive and mCRPC biopsies, differences were identified in AR, TP53, RB1, and PI3K/AKT mutational status between same-patient samples. In conclusion, the genomics of diagnostic prostatic biopsies acquired from men who develop mCRPC differ from those of the nonlethal primary prostatic cancers. RB1/TP53/AR aberrations are enriched in later stages, but the prevalence of DDR defects in diagnostic samples is similar to mCRPC.
Authors
Joaquin Mateo, George Seed, Claudia Bertan, Pasquale Rescigno, David Dolling, Ines Figueiredo, Susana Miranda, Daniel Nava Rodrigues, Bora Gurel, Matthew Clarke, Mark Atkin, Rob Chandler, Carlo Messina, Semini Sumanasuriya, Diletta Bianchini, Maialen Barrero, Antonella Petermolo, Zafeiris Zafeiriou, Mariane Fontes, Raquel Perez-Lopez, Nina Tunariu, Ben Fulton, Robert Jones, Ursula McGovern, Christy Ralph, Mohini Varughese, Omi Parikh, Suneil Jain, Tony Elliott, Shahneen Sandhu, Nuria Porta, Emma Hall, Wei Yuan, Suzanne Carreira, Johann S. de Bono
Kewen Hu, Kun Li, Jing Lv, Jie Feng, Jing Chen, Haigang Wu, Feixiong Cheng, Wenhao Jiang, Jieqiong Wang, Haixiang Pei, Paul J. Chiao, Zhenyu Cai, Yihua Chen, Mingyao Liu, Xiufeng PangKewen Hu, Kun Li, Jing Lv, Jie Feng, Jing Chen, Haigang Wu, Feixiong Cheng, Wenhao Jiang, Jieqiong Wang, Haixiang Pei, Paul J. Chiao, Zhenyu Cai, Yihua Chen, Mingyao Liu, Xiufeng Pang×Abstract
Oncogenic KRAS is a major driver in lung adenocarcinoma (LUAD) that has yet to be therapeutically conquered. Here we report that the SLC7A11/glutathione axis displays metabolic synthetic lethality with oncogenic KRAS. Through metabolomics approaches, we found that mutationally activated KRAS strikingly increased intracellular cystine levels and glutathione biosynthesis. SLC7A11, a cystine/glutamate antiporter conferring specificity for cystine uptake, was overexpressed in patients with KRAS-mutant LUAD and showed positive association with tumor progression. Furthermore, SLC7A11 inhibition by either genetic depletion or pharmacological inhibition with sulfasalazine resulted in selective killing across a panel of KRAS-mutant cancer cells in vitro and tumor growth inhibition in vivo, suggesting the functionality and specificity of SLC7A11 as a therapeutic target. Importantly, we further identified a potent SLC7A11 inhibitor, HG106, that markedly decreased cystine uptake and intracellular glutathione biosynthesis. Furthermore, HG106 exhibited selective cytotoxicity toward KRAS-mutant cells by increasing oxidative stress– and ER stress–mediated cell apoptosis. Of note, treatment of KRAS-mutant LUAD with HG106 in several preclinical lung cancer mouse models led to marked tumor suppression and prolonged survival. Overall, our findings reveal that KRAS-mutant LUAD cells are vulnerable to SLC7A11 inhibition, offering potential therapeutic approaches for this currently incurable disease.
Authors
Kewen Hu, Kun Li, Jing Lv, Jie Feng, Jing Chen, Haigang Wu, Feixiong Cheng, Wenhao Jiang, Jieqiong Wang, Haixiang Pei, Paul J. Chiao, Zhenyu Cai, Yihua Chen, Mingyao Liu, Xiufeng Pang
×Abstract
Parathyroid hormone (PTH) is a critical regulator of skeletal development that promotes both bone formation and bone resorption. Using microbiota depletion by wide-spectrum antibiotics and germ-free (GF) female mice, we showed that the microbiota was required for PTH to stimulate bone formation and increase bone mass. Microbiota depletion lowered butyrate levels, a metabolite responsible for gut-bone communication, while reestablishment of physiologic levels of butyrate restored PTH-induced anabolism. The permissive activity of butyrate was mediated by GPR43 signaling in dendritic cells and by GPR43-independent signaling in T cells. Butyrate was required for PTH to increase the number of bone marrow (BM) regulatory T cells (Tregs). Tregs stimulated production of the osteogenic Wnt ligand Wnt10b by BM CD8+ T cells, which activated Wnt-dependent bone formation. Together, these data highlight the role that butyrate produced by gut luminal microbiota plays in triggering regulatory pathways, which are critical for the anabolic action of PTH in bone.
Authors
Jau-Yi Li, Mingcan Yu, Subhashis Pal, Abdul Malik Tyagi, Hamid Dar, Jonathan Adams, M. Neale Weitzmann, Rheinallt M. Jones, Roberto Pacifici
×Abstract
Recent findings have shown that inhibitors targeting bromodomain and extraterminal domain (BET) proteins, such as the small molecule JQ1, are potent growth inhibitors of many cancers and hold promise for cancer therapy. However, some reports have also revealed that JQ1 can activate additional oncogenic pathways and may affect epithelial-to-mesenchymal transition (EMT). Therefore, it is important to address the potential unexpected effect of JQ1 treatment, such as cell invasion and metastasis. Here, we showed that in prostate cancer, JQ1 inhibited cancer cell growth but promoted invasion and metastasis in a BET protein–independent manner. Multiple invasion pathways including EMT, bone morphogenetic protein (BMP) signaling, chemokine signaling, and focal adhesion were activated by JQ1 to promote invasion. Notably, JQ1 induced upregulation of invasion genes through inhibition of Forkhead box protein A1 (FOXA1), an invasion suppressor in prostate cancer. JQ1 directly interacted with FOXA1 and inactivated FOXA1 binding to its interacting repressors TLE3, HDAC7, and NFIC, thereby blocking FOXA1-repressive function and activating the invasion genes. Our findings indicate that JQ1 has an unexpected effect of promoting invasion in prostate cancer. Thus, the ill effect of JQ1 or its derived therapeutic agents cannot be ignored during cancer treatment, especially in FOXA1-related cancers.
Authors
Leiming Wang, Mafei Xu, Chung-Yang Kao, Sophia Y. Tsai, Ming-Jer Tsai
×Abstract
Bruton tyrosine kinase (BTK) is present in a wide variety of cells and may thus have important non–B cell functions. Here, we explored the function of this kinase in macrophages with studies of its regulation of the NLR family, pyrin domain–containing 3 (NLRP3) inflammasome. We found that bone marrow–derived macrophages (BMDMs) from BTK-deficient mice or monocytes from patients with X-linked agammaglobulinemia (XLA) exhibited increased NLRP3 inflammasome activity; this was also the case for BMDMs exposed to low doses of BTK inhibitors such as ibrutinib and for monocytes from patients with chronic lymphocytic leukemia being treated with ibrutinib. In mechanistic studies, we found that BTK bound to NLRP3 during the priming phase of inflammasome activation and, in doing so, inhibited LPS- and nigericin-induced assembly of the NLRP3 inflammasome during the activation phase of inflammasome activation. This inhibitory effect was caused by BTK inhibition of protein phosphatase 2A–mediated (PP2A-mediated) dephosphorylation of Ser5 in the pyrin domain of NLRP3. Finally, we show that BTK-deficient mice were subject to severe experimental colitis and that such colitis was normalized by administration of anti–IL-β or anakinra, an inhibitor of IL-1β signaling. Together, these studies strongly suggest that BTK functions as a physiologic inhibitor of NLRP3 inflammasome activation and explain why patients with XLA are prone to develop Crohn’s disease.
Authors
Liming Mao, Atsushi Kitani, Eitaro Hiejima, Kim Montgomery-Recht, Wenchang Zhou, Ivan Fuss, Adrian Wiestner, Warren Strober
Tingting Chen, Caroline Blanc, Yanyan Liu, Elise Ishida, Sarah Singer, Jiayong Xu, Maju Joe, Elizabeth R. Jenny-Avital, John Chan, Todd L. Lowary, Jacqueline M. AchkarTingting Chen, Caroline Blanc, Yanyan Liu, Elise Ishida, Sarah Singer, Jiayong Xu, Maju Joe, Elizabeth R. Jenny-Avital, John Chan, Todd L. Lowary, Jacqueline M. Achkar×Abstract
A better understanding of all immune components involved in protecting against Mycobacterium tuberculosis infection is urgently needed to inform strategies for novel immunotherapy and tuberculosis (TB) vaccine development. Although cell-mediated immunity is critical, increasing evidence supports that antibodies also have a protective role against TB. Yet knowledge of protective antigens is limited. Analyzing sera from 97 US immigrants at various stages of M. tuberculosis infection, we showed protective in vitro and in vivo efficacy of polyclonal IgG against the M. tuberculosis capsular polysaccharide arabinomannan (AM). Using recently developed glycan arrays, we established that anti-AM IgG induced in natural infection is highly heterogeneous in its binding specificity and differs in both its reactivity to oligosaccharide motifs within AM and its functions in bacillus Calmette-Guérin vaccination and/or in controlled (latent) versus uncontrolled (TB) M. tuberculosis infection. We showed that anti-AM IgG from asymptomatic but not from diseased individuals was protective and provided data suggesting a potential role of IgG2 and specific AM oligosaccharides. Filling a gap in the current knowledge of protective antigens in humans, our data support the key role of the M. tuberculosis surface glycan AM and suggest the importance of targeting specific glycan epitopes within AM in antibody-mediated immunity against TB.
Authors
Tingting Chen, Caroline Blanc, Yanyan Liu, Elise Ishida, Sarah Singer, Jiayong Xu, Maju Joe, Elizabeth R. Jenny-Avital, John Chan, Todd L. Lowary, Jacqueline M. Achkar
Channakeshava Sokke Umeshappa, Jacques Mbongue, Santiswarup Singha, Saswat Mohapatra, Jun Yamanouchi, Justin A. Lee, Roopa Hebbandi Nanjundappa, Kun Shao, Urs Christen, Yang Yang, Kristofor K. Ellestad, Pere SantamariaChannakeshava Sokke Umeshappa, Jacques Mbongue, Santiswarup Singha, Saswat Mohapatra, Jun Yamanouchi, Justin A. Lee, Roopa Hebbandi Nanjundappa, Kun Shao, Urs Christen, Yang Yang, Kristofor K. Ellestad, Pere Santamaria×Abstract
Peptide MHC class II–based (pMHCII-based) nanomedicines trigger the formation of multicellular regulatory networks by reprogramming autoantigen-experienced CD4+ T cells into autoimmune disease–suppressing T regulatory type 1 (TR1) cells. We have shown that pMHCII-based nanomedicines displaying liver autoimmune disease–relevant yet ubiquitously expressed antigens can blunt various liver autoimmune disorders in a non–disease-specific manner without suppressing local or systemic immunity against infectious agents or cancer. Here, we show that such ubiquitous autoantigen-specific T cells are also awakened by extrahepatic tissue damage and that the corresponding TR1 progeny can suppress experimental autoimmune encephalomyelitis (EAE) and pancreatic β cell autoreactivity. In mice having EAE, nanomedicines displaying either ubiquitous or CNS-specific epitopes triggered the formation and expansion of cognate TR1 cells and their recruitment to the CNS-draining lymph nodes, sparing their liver-draining counterparts. Surprisingly, in mice having both liver autoimmunity and EAE, liver inflammation sequestered these ubiquitous or even CNS-specific TR1 cells away from the CNS, abrogating their antiencephalitogenic activity. In these mice, only the ubiquitous antigen-specific TR1 cells suppressed liver autoimmunity. Thus, the scope of antigen spreading in autoimmune disorders is larger than previously anticipated, involving specificities expected to be silenced by mechanisms of tolerance; the regulatory activity, but not the retention of autoreactive TR1 cells, requires local autoantigen expression.
Authors
Channakeshava Sokke Umeshappa, Jacques Mbongue, Santiswarup Singha, Saswat Mohapatra, Jun Yamanouchi, Justin A. Lee, Roopa Hebbandi Nanjundappa, Kun Shao, Urs Christen, Yang Yang, Kristofor K. Ellestad, Pere Santamaria
Yan Xiong, Liqing Wang, Eros Di Giorgio, Tatiana Akimova, Ulf H. Beier, Rongxiang Han, Matteo Trevisanut, Jay H. Kalin, Philip A. Cole, Wayne W. HancockYan Xiong, Liqing Wang, Eros Di Giorgio, Tatiana Akimova, Ulf H. Beier, Rongxiang Han, Matteo Trevisanut, Jay H. Kalin, Philip A. Cole, Wayne W. Hancock×Abstract
Foxp3+ Tregs are key to immune homeostasis, but the contributions of various large, multiprotein complexes that regulate gene expression remain unexplored. We analyzed the role in Tregs of the evolutionarily conserved CoREST complex, consisting of a scaffolding protein, Rcor1 or Rcor2, plus Hdac1 or Hdac2 and Lsd1 enzymes. Rcor1, Rcor2, and Lsd1 were physically associated with Foxp3, and mice with conditional deletion of Rcor1 in Foxp3+ Tregs had decreased proportions of Tregs in peripheral lymphoid tissues and increased Treg expression of IL-2 and IFN-γ compared with what was found in WT cells. Mice with conditional deletion of the gene encoding Rcor1 in their Tregs had reduced suppression of homeostatic proliferation, inability to maintain long-term allograft survival despite costimulation blockade, and enhanced antitumor immunity in syngeneic models. Comparable findings were seen in WT mice treated with CoREST complex bivalent inhibitors, which also altered the phenotype of human Tregs and impaired their suppressive function. Our data point to the potential for therapeutic modulation of Treg functions by pharmacologic targeting of enzymatic components of the CoREST complex and contribute to an understanding of the biochemical and molecular mechanisms by which Foxp3 represses large gene sets and maintains the unique properties of this key immune cell.
Authors
Yan Xiong, Liqing Wang, Eros Di Giorgio, Tatiana Akimova, Ulf H. Beier, Rongxiang Han, Matteo Trevisanut, Jay H. Kalin, Philip A. Cole, Wayne W. Hancock
Ritika Dutta, Tian Yi Zhang, Thomas Köhnke, Daniel Thomas, Miles Linde, Eric Gars, Melissa Stafford, Satinder Kaur, Yusuke Nakauchi, Raymond Yin, Armon Azizi, Anupama Narla, Ravindra MajetiRitika Dutta, Tian Yi Zhang, Thomas Köhnke, Daniel Thomas, Miles Linde, Eric Gars, Melissa Stafford, Satinder Kaur, Yusuke Nakauchi, Raymond Yin, Armon Azizi, Anupama Narla, Ravindra Majeti×Abstract
Cancer-related anemia is present in more than 60% of newly diagnosed cancer patients and is associated with substantial morbidity and high medical costs. Drugs that enhance erythropoiesis are urgently required to decrease transfusion rates and improve quality of life. Clinical studies have observed an unexpected improvement in hemoglobin and RBC transfusion-independence in patients with acute myeloid leukemia (AML) treated with the isocitrate dehydrogenase 2 (IDH2) mutant-specific inhibitor enasidenib, leading to improved quality of life without a reduction in AML disease burden. Here, we demonstrate that enasidenib enhanced human erythroid differentiation of hematopoietic progenitors. The phenomenon was not observed with other IDH1/2 inhibitors and occurred in IDH2-deficient CRISPR-engineered progenitors independently of D-2-hydroxyglutarate. The effect of enasidenib on hematopoietic progenitors was mediated by protoporphyrin accumulation, driving heme production and erythroid differentiation in committed CD71+ progenitors rather than hematopoietic stem cells. Our results position enasidenib as a promising therapeutic agent for improvement of anemia and provide the basis for a clinical trial using enasidenib to decrease transfusion dependence in a wide array of clinical contexts.
Authors
Ritika Dutta, Tian Yi Zhang, Thomas Köhnke, Daniel Thomas, Miles Linde, Eric Gars, Melissa Stafford, Satinder Kaur, Yusuke Nakauchi, Raymond Yin, Armon Azizi, Anupama Narla, Ravindra Majeti
Michael R. Rickels, Carmella Evans-Molina, Henry T. Bahnson, Alyssa Ylescupidez, Kristen J. Nadeau, Wei Hao, Mark A. Clements, Jennifer L. Sherr, Richard E. Pratley, Tamara S. Hannon, Viral N. Shah, Kellee M. Miller, Carla J. Greenbaum, the T1D Exchange β-Cell Function Study GroupMichael R. Rickels, Carmella Evans-Molina, Henry T. Bahnson, Alyssa Ylescupidez, Kristen J. Nadeau, Wei Hao, Mark A. Clements, Jennifer L. Sherr, Richard E. Pratley, Tamara S. Hannon, Viral N. Shah, Kellee M. Miller, Carla J. Greenbaum, the T1D Exchange β-Cell Function Study Group×Abstract
BACKGROUND Residual C-peptide is detected in many people for years following the diagnosis of type 1 diabetes; however, the physiologic significance of low levels of detectable C-peptide is not known.METHODS We studied 63 adults with type 1 diabetes classified by peak mixed-meal tolerance test (MMTT) C-peptide as negative (<0.007 pmol/mL; n = 15), low (0.017–0.200; n = 16), intermediate (>0.200–0.400; n = 15), or high (>0.400; n = 17). We compared the groups’ glycemia from continuous glucose monitoring (CGM), β cell secretory responses from a glucose-potentiated arginine (GPA) test, insulin sensitivity from a hyperinsulinemic-euglycemic (EU) clamp, and glucose counterregulatory responses from a subsequent hypoglycemic (HYPO) clamp.RESULTS Low and intermediate MMTT C-peptide groups did not exhibit β cell secretory responses to hyperglycemia, whereas the high C-peptide group showed increases in both C-peptide and proinsulin (P ≤ 0.01). All groups with detectable MMTT C-peptide demonstrated acute C-peptide and proinsulin responses to arginine that were positively correlated with peak MMTT C-peptide (P < 0.0001 for both analytes). During the EU-HYPO clamp, C-peptide levels were proportionately suppressed in the low, intermediate, and high C-peptide compared with the negative group (P ≤ 0.0001), whereas glucagon increased from EU to HYPO only in the high C-peptide group compared with negative (P = 0.01). CGM demonstrated lower mean glucose and more time in range for the high C-peptide group.CONCLUSION These results indicate that in adults with type 1 diabetes, β cell responsiveness to hyperglycemia and α cell responsiveness to hypoglycemia are observed only at high levels of residual C-peptide that likely contribute to glycemic control.FUNDING Funding for this work was provided by the Leona M. and Harry B. Helmsley Charitable Trust, the National Center for Advancing Translational Sciences, and the National Institute of Diabetes and Digestive and Kidney Diseases.
Authors
Michael R. Rickels, Carmella Evans-Molina, Henry T. Bahnson, Alyssa Ylescupidez, Kristen J. Nadeau, Wei Hao, Mark A. Clements, Jennifer L. Sherr, Richard E. Pratley, Tamara S. Hannon, Viral N. Shah, Kellee M. Miller, Carla J. Greenbaum, the T1D Exchange β-Cell Function Study Group
Eric Gracey, Dominika Hromadová, Melissa Lim, Zoya Qaiyum, Michael Zeng, Yuchen Yao, Archita Srinath, Yuriy Baglaenko, Natalia Yeremenko, William Westlin, Craig Masse, Mathias Müller, Birgit Strobl, Wenyan Miao, Robert D. InmanEric Gracey, Dominika Hromadová, Melissa Lim, Zoya Qaiyum, Michael Zeng, Yuchen Yao, Archita Srinath, Yuriy Baglaenko, Natalia Yeremenko, William Westlin, Craig Masse, Mathias Müller, Birgit Strobl, Wenyan Miao, Robert D. Inman×TYK2 inhibition reduces type 3 immunity and modifies disease progression in murine spondyloarthritis
Abstract
Spondyloarthritis (SpA) represents a family of inflammatory diseases of the spine and peripheral joints. Ankylosing spondylitis (AS) is the prototypic form of SpA in which progressive disease can lead to fusion of the spine. Therapeutically, knowledge of type 3 immunity has translated into the development of IL-23– and IL-17A–blocking antibodies for the treatment of SpA. Despite being able to provide symptomatic control, the current biologics do not prevent the fusion of joints in AS patients. Thus, there is an unmet need for disease-modifying drugs. Genetic studies have linked the Janus kinase TYK2 to AS. TYK2 is a mediator of type 3 immunity through intracellular signaling of IL-23. Here, we describe and characterize a potentially novel small-molecule inhibitor of TYK2 that blocked IL-23 signaling in vitro and inhibited disease progression in animal models of SpA. The effect of the inhibitor appears to be TYK2 specific, using TYK2-inactive mice, which further revealed a duality in the induction of IL-17A and IL-22 by IL-23. Specifically, IL-22 production was TYK2/JAK2/STAT3 dependent, while IL-17A was mostly JAK2 dependent. Finally, we examined the effects of AS-associated TYK2 SNPs on TYK2 expression and function and correlated them with AS disease progression. This work provides evidence that TYK2 inhibitors have great potential as an orally delivered therapeutic for SpA.
Authors
Eric Gracey, Dominika Hromadová, Melissa Lim, Zoya Qaiyum, Michael Zeng, Yuchen Yao, Archita Srinath, Yuriy Baglaenko, Natalia Yeremenko, William Westlin, Craig Masse, Mathias Müller, Birgit Strobl, Wenyan Miao, Robert D. Inman
Karmele Valencia, Oihane Erice, Kaja Kostyrko, Simone Hausmann, Elizabeth Guruceaga, Anuradha Tathireddy, Natasha M. Flores, Leanne C. Sayles, Alex G. Lee, Rita Fragoso, Tian-Qiang Sun, Adrian Vallejo, Marta Roman, Rodrigo Entrialgo-Cadierno, Itziar Migueliz, Nerea Razquin, Puri Fortes, Fernando Lecanda, Jun Lu, Mariano Ponz-Sarvise, Chang-Zheng Chen, Pawel K. Mazur, E. Alejandro Sweet-Cordero, Silvestre VicentKarmele Valencia, Oihane Erice, Kaja Kostyrko, Simone Hausmann, Elizabeth Guruceaga, Anuradha Tathireddy, Natasha M. Flores, Leanne C. Sayles, Alex G. Lee, Rita Fragoso, Tian-Qiang Sun, Adrian Vallejo, Marta Roman, Rodrigo Entrialgo-Cadierno, Itziar Migueliz, Nerea Razquin, Puri Fortes, Fernando Lecanda, Jun Lu, Mariano Ponz-Sarvise, Chang-Zheng Chen, Pawel K. Mazur, E. Alejandro Sweet-Cordero, Silvestre Vicent×Abstract
Few therapies are currently available for patients with KRAS-driven cancers, highlighting the need to identify new molecular targets that modulate central downstream effector pathways. Here we found that the microRNA (miRNA) cluster including miR181ab1 is a key modulator of KRAS-driven oncogenesis. Ablation of Mir181ab1 in genetically engineered mouse models of Kras-driven lung and pancreatic cancer was deleterious to tumor initiation and progression. Expression of both resident miRNAs in the Mir181ab1 cluster, miR181a1 and miR181b1, was necessary to rescue the Mir181ab1-loss phenotype, underscoring their nonredundant role. In human cancer cells, depletion of miR181ab1 impaired proliferation and 3D growth, whereas overexpression provided a proliferative advantage. Lastly, we unveiled miR181ab1-regulated genes responsible for this phenotype. These studies identified what we believe to be a previously unknown role for miR181ab1 as a potential therapeutic target in 2 highly aggressive and difficult to treat KRAS-mutated cancers.
Authors
Karmele Valencia, Oihane Erice, Kaja Kostyrko, Simone Hausmann, Elizabeth Guruceaga, Anuradha Tathireddy, Natasha M. Flores, Leanne C. Sayles, Alex G. Lee, Rita Fragoso, Tian-Qiang Sun, Adrian Vallejo, Marta Roman, Rodrigo Entrialgo-Cadierno, Itziar Migueliz, Nerea Razquin, Puri Fortes, Fernando Lecanda, Jun Lu, Mariano Ponz-Sarvise, Chang-Zheng Chen, Pawel K. Mazur, E. Alejandro Sweet-Cordero, Silvestre Vicent
×Abstract
Acute graft-versus-host disease (GVHD) is initially triggered by alloreactive T cells, which damage peripheral tissues and lymphoid organs. Subsequent transition to chronic GVHD involves the emergence of autoimmunity, although the underlying mechanisms driving this process are unclear. Here, we tested the hypothesis that acute GVHD blocks peripheral tolerance of autoreactive T cells by impairing lymph node (LN) display of peripheral tissue–restricted antigens (PTAs). At the initiation of GVHD, LN fibroblastic reticular cells (FRCs) rapidly reduced expression of genes regulated by DEAF1, an autoimmune regulator-like transcription factor required for intranodal expression of PTAs. Subsequently, GVHD led to the selective elimination of the FRC population, and blocked the repair pathways required for its regeneration. We used a transgenic mouse model to show that the loss of presentation of an intestinal PTA by FRCs during GVHD resulted in the activation of autoaggressive T cells and gut injury. Finally, we show that FRCs normally expressed a unique PTA gene signature that was highly enriched for genes expressed in the target organs affected by chronic GVHD. In conclusion, acute GVHD damages and prevents repair of the FRC network, thus disabling an essential platform for purging autoreactive T cells from the repertoire.
Authors
Simone Dertschnig, Pamela Evans, Pedro Santos e Sousa, Teresa Manzo, Ivana R. Ferrer, Hans J. Stauss, Clare L. Bennett, Ronjon Chakraverty
Ethan R. Roy, Baiping Wang, Ying-wooi Wan, Gabriel Chiu, Allysa Cole, Zhuoran Yin, Nicholas E. Propson, Yin Xu, Joanna L. Jankowsky, Zhandong Liu, Virginia M.-Y. Lee, John Q. Trojanowski, Stephen D. Ginsberg, Oleg Butovsky, Hui Zheng, Wei CaoEthan R. Roy, Baiping Wang, Ying-wooi Wan, Gabriel Chiu, Allysa Cole, Zhuoran Yin, Nicholas E. Propson, Yin Xu, Joanna L. Jankowsky, Zhandong Liu, Virginia M.-Y. Lee, John Q. Trojanowski, Stephen D. Ginsberg, Oleg Butovsky, Hui Zheng, Wei Cao×Abstract
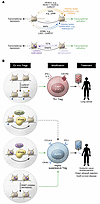
Type I interferon (IFN) is a key cytokine that curbs viral infection and cell malignancy. Previously, we demonstrated a potent IFN immunogenicity of nucleic acid–containing (NA-containing) amyloid fibrils in the periphery. Here, we investigated whether IFN is associated with β-amyloidosis inside the brain and contributes to neuropathology. An IFN-stimulated gene (ISG) signature was detected in the brains of multiple murine Alzheimer disease (AD) models, a phenomenon also observed in WT mouse brain challenged with generic NA-containing amyloid fibrils. In vitro, microglia innately responded to NA-containing amyloid fibrils. In AD models, activated ISG-expressing microglia exclusively surrounded NA+ amyloid β plaques, which accumulated in an age-dependent manner. Brain administration of rIFN-β resulted in microglial activation and complement C3-dependent synapse elimination in vivo. Conversely, selective IFN receptor blockade effectively diminished the ongoing microgliosis and synapse loss in AD models. Moreover, we detected activated ISG-expressing microglia enveloping NA-containing neuritic plaques in postmortem brains of patients with AD. Gene expression interrogation revealed that IFN pathway was grossly upregulated in clinical AD and significantly correlated with disease severity and complement activation. Therefore, IFN constitutes a pivotal element within the neuroinflammatory network of AD and critically contributes to neuropathogenic processes.
Authors
Ethan R. Roy, Baiping Wang, Ying-wooi Wan, Gabriel Chiu, Allysa Cole, Zhuoran Yin, Nicholas E. Propson, Yin Xu, Joanna L. Jankowsky, Zhandong Liu, Virginia M.-Y. Lee, John Q. Trojanowski, Stephen D. Ginsberg, Oleg Butovsky, Hui Zheng, Wei Cao
Cristiane de Oliveira, Biswajit Khatua, Pawan Noel, Sergiy Kostenko, Arup Bag, Bijinu Balakrishnan, Krutika S. Patel, Andre A. Guerra, Melissa N. Martinez, Shubham Trivedi, Ann McCullough, Dora M. Lam-Himlin, Sarah Navina, Douglas O. Faigel, Norio Fukami, Rahul Pannala, Anna Evans Phillips, Georgios I. Papachristou, Erin E. Kershaw, Mark E. Lowe, Vijay P. SinghCristiane de Oliveira, Biswajit Khatua, Pawan Noel, Sergiy Kostenko, Arup Bag, Bijinu Balakrishnan, Krutika S. Patel, Andre A. Guerra, Melissa N. Martinez, Shubham Trivedi, Ann McCullough, Dora M. Lam-Himlin, Sarah Navina, Douglas O. Faigel, Norio Fukami, Rahul Pannala, Anna Evans Phillips, Georgios I. Papachristou, Erin E. Kershaw, Mark E. Lowe, Vijay P. Singh×Abstract
Visceral adipose tissue plays a critical role in numerous diseases. Although imaging studies often show adipose involvement in abdominal diseases, their outcomes may vary from being a mild self-limited illness to one with systemic inflammation and organ failure. We therefore compared the pattern of visceral adipose injury during acute pancreatitis and acute diverticulitis to determine its role in organ failure. Acute pancreatitis–associated adipose tissue had ongoing lipolysis in the absence of adipocyte triglyceride lipase (ATGL). Pancreatic lipase injected into mouse visceral adipose tissue hydrolyzed adipose triglyceride and generated excess nonesterified fatty acids (NEFAs), which caused organ failure in the absence of acute pancreatitis. Pancreatic triglyceride lipase (PNLIP) increased in adipose tissue during pancreatitis and entered adipocytes by multiple mechanisms, hydrolyzing adipose triglyceride and generating excess NEFAs. During pancreatitis, obese PNLIP-knockout mice, unlike obese adipocyte-specific ATGL knockouts, had lower visceral adipose tissue lipolysis, milder inflammation, less severe organ failure, and improved survival. PNLIP-knockout mice, unlike ATGL knockouts, were protected from adipocyte-induced pancreatic acinar injury without affecting NEFA signaling or acute pancreatitis induction. Therefore, during pancreatitis, unlike diverticulitis, PNLIP leaking into visceral adipose tissue can cause excessive visceral adipose tissue lipolysis independently of adipocyte-autonomous ATGL, and thereby worsen organ failure.
Authors
Cristiane de Oliveira, Biswajit Khatua, Pawan Noel, Sergiy Kostenko, Arup Bag, Bijinu Balakrishnan, Krutika S. Patel, Andre A. Guerra, Melissa N. Martinez, Shubham Trivedi, Ann McCullough, Dora M. Lam-Himlin, Sarah Navina, Douglas O. Faigel, Norio Fukami, Rahul Pannala, Anna Evans Phillips, Georgios I. Papachristou, Erin E. Kershaw, Mark E. Lowe, Vijay P. Singh
Joshua N. Curry, Matthew Saurette, Masomeh Askari, Lei Pei, Michael B. Filla, Megan R. Beggs, Peter S.N. Rowe, Timothy Fields, Andre J. Sommer, Chizu Tanikawa, Yoichiro Kamatani, Andrew P. Evan, Mehdi Totonchi, R. Todd Alexander, Koichi Matsuda, Alan S.L. YuJoshua N. Curry, Matthew Saurette, Masomeh Askari, Lei Pei, Michael B. Filla, Megan R. Beggs, Peter S.N. Rowe, Timothy Fields, Andre J. Sommer, Chizu Tanikawa, Yoichiro Kamatani, Andrew P. Evan, Mehdi Totonchi, R. Todd Alexander, Koichi Matsuda, Alan S.L. Yu×Abstract
The major risk factor for kidney stone disease is idiopathic hypercalciuria. Recent evidence implicates a role for defective calcium reabsorption in the renal proximal tubule. We hypothesized that claudin-2, a paracellular cation channel protein, mediates proximal tubule calcium reabsorption. We found that claudin-2–null mice have hypercalciuria due to a primary defect in renal tubule calcium transport and papillary nephrocalcinosis that resembles the intratubular plugs in kidney stone formers. Our findings suggest that a proximal tubule defect in calcium reabsorption predisposes to papillary calcification, providing support for the vas washdown hypothesis. Claudin-2–null mice were also found to have increased net intestinal calcium absorption, but reduced paracellular calcium permeability in the colon, suggesting that this was due to reduced intestinal calcium secretion. Common genetic variants in the claudin-2 gene were associated with decreased tissue expression of claudin-2 and increased risk of kidney stones in 2 large population-based studies. Finally, we describe a family in which males with a rare missense variant in claudin-2 have marked hypercalciuria and kidney stone disease. Our findings indicate that claudin-2 is a key regulator of calcium excretion and a potential target for therapies to prevent kidney stones.
Authors
Joshua N. Curry, Matthew Saurette, Masomeh Askari, Lei Pei, Michael B. Filla, Megan R. Beggs, Peter S.N. Rowe, Timothy Fields, Andre J. Sommer, Chizu Tanikawa, Yoichiro Kamatani, Andrew P. Evan, Mehdi Totonchi, R. Todd Alexander, Koichi Matsuda, Alan S.L. Yu
×Abstract
Induction of the inflammasome protein cryopyrin (NLRP3) in visceral adipose tissue (VAT) promotes release of the proinflammatory cytokine IL-1β in obesity. Although this mechanism contributes to peripheral metabolic dysfunction, effects on the brain remain unexplored. We investigated whether visceral adipose NLRP3 impairs cognition by activating microglial IL-1 receptor 1 (IL-1R1). After observing protection against obesity-induced neuroinflammation and cognitive impairment in NLRP3-KO mice, we transplanted VAT from obese WT or NLRP3-KO donors into lean recipient mice. Transplantation of VAT from a WT donor (TRANSWT) increased hippocampal IL-1β and impaired cognition, but VAT transplants from comparably obese NLRP3-KO donors (TRANSKO) had no effect. Visceral adipose NLRP3 was required for deficits in long-term potentiation (LTP) in transplant recipients, and LTP impairment in TRANSWT mice was IL-1 dependent. Flow cytometric and gene expression analyses revealed that VAT transplantation recapitulated the effects of obesity on microglial activation and IL-1β gene expression, and visualization of hippocampal microglia revealed similar effects in vivo. Inducible ablation of IL-1R1 in CX3CR1-expressing cells eliminated cognitive impairment in mice with dietary obesity and in transplant recipients and restored immunoquiescence in hippocampal microglia. These results indicate that visceral adipose NLRP3 impairs memory via IL-1–mediated microglial activation and suggest that NLRP3/IL-1β signaling may underlie correlations between visceral adiposity and cognitive impairment in humans.
Authors
De-Huang Guo, Masaki Yamamoto, Caterina M. Hernandez, Hesam Khodadadi, Babak Baban, Alexis M. Stranahan
Zhilin Li, Emilia A. Korhonen, Arianna Merlini, Judith Strauss, Eleonoora Wihuri, Harri Nurmi, Salli Antila, Jennifer Paech, Urban Deutsch, Britta Engelhardt, Sudhakar Chintharlapalli, Gou Young Koh, Alexander Flügel, Kari AlitaloZhilin Li, Emilia A. Korhonen, Arianna Merlini, Judith Strauss, Eleonoora Wihuri, Harri Nurmi, Salli Antila, Jennifer Paech, Urban Deutsch, Britta Engelhardt, Sudhakar Chintharlapalli, Gou Young Koh, Alexander Flügel, Kari Alitalo×Abstract
Angiopoietin-2 (Ang2), a ligand of the endothelial Tie2 tyrosine kinase, is involved in vascular inflammation and leakage in critically ill patients. However, the role of Ang2 in demyelinating central nervous system (CNS) autoimmune diseases is unknown. Here, we report that Ang2 is critically involved in the pathogenesis of experimental autoimmune encephalomyelitis (EAE), a rodent model of multiple sclerosis. Ang2 expression was induced in CNS autoimmunity, and transgenic mice overexpressing Ang2 specifically in endothelial cells (ECs) developed a significantly more severe EAE. In contrast, treatment with Ang2-blocking Abs ameliorated neuroinflammation and decreased spinal cord demyelination and leukocyte infiltration into the CNS. Similarly, Ang2-binding and Tie2-activating Ab attenuated the development of CNS autoimmune disease. Ang2 blockade inhibited expression of EC adhesion molecules, improved blood-brain barrier integrity, and decreased expression of genes involved in antigen presentation and proinflammatory responses of microglia and macrophages, which was accompanied by inhibition of α5β1 integrin activation in microglia. Taken together, our data suggest that Ang2 provides a target for increasing Tie2 activation in ECs and inhibiting proinflammatory polarization of CNS myeloid cells via α5β1 integrin in neuroinflammation. Thus, Ang2 targeting may serve as a therapeutic option for the treatment of CNS autoimmune disease.
Authors
Zhilin Li, Emilia A. Korhonen, Arianna Merlini, Judith Strauss, Eleonoora Wihuri, Harri Nurmi, Salli Antila, Jennifer Paech, Urban Deutsch, Britta Engelhardt, Sudhakar Chintharlapalli, Gou Young Koh, Alexander Flügel, Kari Alitalo
Anjui Wu, Paolo Cremaschi, Daniel Wetterskog, Vincenza Conteduca, Gian Marco Franceschini, Dimitrios Kleftogiannis, Anuradha Jayaram, Shahneen Sandhu, Stephen Q. Wong, Matteo Benelli, Samanta Salvi, Giorgia Gurioli, Andrew Feber, Mariana Buongermino Pereira, Anna Maria Wingate, Enrique Gonzalez-Billalebeitia, Ugo De Giorgi, Francesca Demichelis, Stefano Lise, Gerhardt AttardAnjui Wu, Paolo Cremaschi, Daniel Wetterskog, Vincenza Conteduca, Gian Marco Franceschini, Dimitrios Kleftogiannis, Anuradha Jayaram, Shahneen Sandhu, Stephen Q. Wong, Matteo Benelli, Samanta Salvi, Giorgia Gurioli, Andrew Feber, Mariana Buongermino Pereira, Anna Maria Wingate, Enrique Gonzalez-Billalebeitia, Ugo De Giorgi, Francesca Demichelis, Stefano Lise, Gerhardt Attard×Abstract
Tumor DNA circulates in the plasma of cancer patients admixed with DNA from noncancerous cells. The genomic landscape of plasma DNA has been characterized in metastatic castration-resistant prostate cancer (mCRPC) but the plasma methylome has not been extensively explored. Here, we performed next-generation sequencing (NGS) on plasma DNA with and without bisulfite treatment from mCRPC patients receiving either abiraterone or enzalutamide in the pre- or post-chemotherapy setting. Principal component analysis on the mCRPC plasma methylome indicated that the main contributor to methylation variance (principal component one, or PC1) was strongly correlated with genomically determined tumor fraction (r = –0.96; P < 10–8) and characterized by hypermethylation of targets of the polycomb repressor complex 2 components. Further deconvolution of the PC1 top-correlated segments revealed that these segments are comprised of methylation patterns specific to either prostate cancer or prostate normal epithelium. To extract information specific to an individual’s cancer, we then focused on an orthogonal methylation signature, which revealed enrichment for androgen receptor binding sequences and hypomethylation of these segments associated with AR copy number gain. Individuals harboring this methylation pattern had a more aggressive clinical course. Plasma methylome analysis can accurately quantitate tumor fraction and identify distinct biologically relevant mCRPC phenotypes.
Authors
Anjui Wu, Paolo Cremaschi, Daniel Wetterskog, Vincenza Conteduca, Gian Marco Franceschini, Dimitrios Kleftogiannis, Anuradha Jayaram, Shahneen Sandhu, Stephen Q. Wong, Matteo Benelli, Samanta Salvi, Giorgia Gurioli, Andrew Feber, Mariana Buongermino Pereira, Anna Maria Wingate, Enrique Gonzalez-Billalebeitia, Ugo De Giorgi, Francesca Demichelis, Stefano Lise, Gerhardt Attard
×Abstract
Meal ingestion increases body temperature in multiple species, an effect that is blunted by obesity. However, the mechanisms responsible for these phenomena remain incompletely understood. Here we show that refeeding increases plasma leptin concentrations approximately 8-fold in 48-hour-fasted lean rats, and this normalization of plasma leptin concentrations stimulates adrenomedullary catecholamine secretion. Increased adrenal medulla–derived plasma catecholamines were necessary and sufficient to increase body temperature postprandially, a process that required both fatty acids generated from adipose tissue lipolysis and β-adrenergic activation of brown adipose tissue (BAT). Diet-induced obese rats, which remained relatively hyperleptinemic while fasting, did not exhibit fasting-induced reductions in temperature. To examine the impact of feeding-induced increases in body temperature on energy balance, we compared rats fed chronically by either 2 carbohydrate-rich boluses daily or a continuous isocaloric intragastric infusion. Bolus feeding increased body temperature and reduced weight gain compared with continuous feeding, an effect abrogated by treatment with atenolol. In summary, these data demonstrate that leptin stimulates a hypothalamus–adrenal medulla–BAT axis, which is necessary and sufficient to induce lipolysis and, as a result, increase body temperature after refeeding.
Authors
Rachel J. Perry, Kun Lyu, Aviva Rabin-Court, Jianying Dong, Xiruo Li, Yunfan Yang, Hua Qing, Andrew Wang, Xiaoyong Yang, Gerald I. Shulman
LaQuita M. Jones, Katelyn Melgar, Lyndsey Bolanos, Kathleen Hueneman, Morgan M. Walker, Jian-Kang Jiang, Kelli M. Wilson, Xiaohu Zhang, Jian Shen, Fan Jiang, Patrick Sutter, Amy Wang, Xin Xu, Gregory J. Tawa, Scott B. Hoyt, Mark Wunderlich, Eric O’Brien, John P. Perentesis, Daniel T. Starczynowski, Craig J. ThomasLaQuita M. Jones, Katelyn Melgar, Lyndsey Bolanos, Kathleen Hueneman, Morgan M. Walker, Jian-Kang Jiang, Kelli M. Wilson, Xiaohu Zhang, Jian Shen, Fan Jiang, Patrick Sutter, Amy Wang, Xin Xu, Gregory J. Tawa, Scott B. Hoyt, Mark Wunderlich, Eric O’Brien, John P. Perentesis, Daniel T. Starczynowski, Craig J. Thomas×Abstract
Tyrosine kinase domain (TKD) mutations contribute to acquired resistance to FMS-like tyrosine kinase 3 (FLT3) inhibitors used to treat FLT3-mutant acute myeloid leukemia (AML). We report a cocrystal structure of FLT3 with a type I inhibitor, NCGC1481, that retained potent binding and activity against FLT3 TKD and gatekeeper mutations. Relative to the current generation of advanced FLT3 inhibitors, NCGC1481 exhibited superior antileukemic activity against the common, clinically relevant FLT3-mutant AML cells in vitro and in vivo.
Authors
LaQuita M. Jones, Katelyn Melgar, Lyndsey Bolanos, Kathleen Hueneman, Morgan M. Walker, Jian-Kang Jiang, Kelli M. Wilson, Xiaohu Zhang, Jian Shen, Fan Jiang, Patrick Sutter, Amy Wang, Xin Xu, Gregory J. Tawa, Scott B. Hoyt, Mark Wunderlich, Eric O’Brien, John P. Perentesis, Daniel T. Starczynowski, Craig J. Thomas
Rita Pinto-Costa, Sara C. Sousa, Sérgio C. Leite, Joana Nogueira-Rodrigues, Tiago Ferreira da Silva, Diana Machado, Joana Marques, Ana Catarina Costa, Márcia A. Liz, Francesca Bartolini, Pedro Brites, Mercedes Costell, Reinhard Fässler, Mónica M. SousaRita Pinto-Costa, Sara C. Sousa, Sérgio C. Leite, Joana Nogueira-Rodrigues, Tiago Ferreira da Silva, Diana Machado, Joana Marques, Ana Catarina Costa, Márcia A. Liz, Francesca Bartolini, Pedro Brites, Mercedes Costell, Reinhard Fässler, Mónica M. Sousa×Abstract
After trauma, regeneration of adult CNS axons is abortive, causing devastating neurologic deficits. Despite progress in rehabilitative care, there is no effective treatment that stimulates axonal growth following injury. Using models with different regenerative capacities, followed by gain- and loss-of-function analysis, we identified profilin 1 (Pfn1) as a coordinator of actin and microtubules (MTs), powering axonal growth and regeneration. In growth cones, Pfn1 increased actin retrograde flow, MT growth speed, and invasion of filopodia by MTs, orchestrating cytoskeletal dynamics toward axonal growth. In vitro, active Pfn1 promoted MT growth in a formin-dependent manner, whereas localization of MTs to growth cone filopodia was facilitated by direct MT binding and interaction with formins. In vivo, Pfn1 ablation limited regeneration of growth-competent axons after sciatic nerve and spinal cord injury. Adeno-associated viral (AAV) delivery of constitutively active Pfn1 to rodents promoted axonal regeneration, neuromuscular junction maturation, and functional recovery of injured sciatic nerves, and increased the ability of regenerating axons to penetrate the inhibitory spinal cord glial scar. Thus, we identify Pfn1 as an important regulator of axonal regeneration and suggest that AAV-mediated delivery of constitutively active Pfn1, together with the identification of modulators of Pfn1 activity, should be considered to treat the injured nervous system.
Authors
Rita Pinto-Costa, Sara C. Sousa, Sérgio C. Leite, Joana Nogueira-Rodrigues, Tiago Ferreira da Silva, Diana Machado, Joana Marques, Ana Catarina Costa, Márcia A. Liz, Francesca Bartolini, Pedro Brites, Mercedes Costell, Reinhard Fässler, Mónica M. Sousa
Guadalupe Ortiz-Muñoz, Michelle A. Yu, Emma Lefrançais, Beñat Mallavia, Colin Valet, Jennifer J. Tian, Serena Ranucci, Kristin M. Wang, Zhe Liu, Nicholas Kwaan, Diana Dawson, Mary Ellen Kleinhenz, Fadi T. Khasawneh, Peter M. Haggie, Alan S. Verkman, Mark R. LooneyGuadalupe Ortiz-Muñoz, Michelle A. Yu, Emma Lefrançais, Beñat Mallavia, Colin Valet, Jennifer J. Tian, Serena Ranucci, Kristin M. Wang, Zhe Liu, Nicholas Kwaan, Diana Dawson, Mary Ellen Kleinhenz, Fadi T. Khasawneh, Peter M. Haggie, Alan S. Verkman, Mark R. Looney×Abstract
Cystic fibrosis (CF) lung disease is characterized by an inflammatory response that can lead to terminal respiratory failure. The cystic fibrosis transmembrane conductance regulator (CFTR) is mutated in CF, and we hypothesized that dysfunctional CFTR in platelets, which are key participants in immune responses, is a central determinant of CF inflammation. We found that deletion of CFTR in platelets produced exaggerated acute lung inflammation and platelet activation after intratracheal LPS or Pseudomonas aeruginosa challenge. CFTR loss of function in mouse or human platelets resulted in agonist-induced hyperactivation and increased calcium entry into platelets. Inhibition of the transient receptor potential cation channel 6 (TRPC6) reduced platelet activation and calcium flux, and reduced lung injury in CF mice after intratracheal LPS or Pseudomonas aeruginosa challenge. CF subjects receiving CFTR modulator therapy showed partial restoration of CFTR function in platelets, which may be a convenient approach to monitoring biological responses to CFTR modulators. We conclude that CFTR dysfunction in platelets produces aberrant TRPC6-dependent platelet activation, which is a major driver of CF lung inflammation and impaired bacterial clearance. Platelets and TRPC6 are what we believe to be novel therapeutic targets in the treatment of CF lung disease.
Authors
Guadalupe Ortiz-Muñoz, Michelle A. Yu, Emma Lefrançais, Beñat Mallavia, Colin Valet, Jennifer J. Tian, Serena Ranucci, Kristin M. Wang, Zhe Liu, Nicholas Kwaan, Diana Dawson, Mary Ellen Kleinhenz, Fadi T. Khasawneh, Peter M. Haggie, Alan S. Verkman, Mark R. Looney
Jason Charish, Alireza P. Shabanzadeh, Danian Chen, Patrick Mehlen, Santhosh Sethuramanujam, Hidekiyo Harada, Vera L. Bonilha, Gautam Awatramani, Rod Bremner, Philippe P. MonnierJason Charish, Alireza P. Shabanzadeh, Danian Chen, Patrick Mehlen, Santhosh Sethuramanujam, Hidekiyo Harada, Vera L. Bonilha, Gautam Awatramani, Rod Bremner, Philippe P. Monnier×Abstract
Inherited retinal degenerations (IRDs) are characterized by the progressive loss of photoreceptors and represent one of the most prevalent causes of blindness among working-age populations. Cyclic nucleotide dysregulation is a common pathological feature linked to numerous forms of IRD, yet the precise mechanisms through which this contributes to photoreceptor death remain elusive. Here we demonstrate that cAMP induced upregulation of the dependence receptor neogenin in the retina. Neogenin levels were also elevated in both human and murine degenerating photoreceptors. We found that overexpressing neogenin in mouse photoreceptors was sufficient to induce cell death, whereas silencing neogenin in degenerating murine photoreceptors promoted survival, thus identifying a pro-death signal in IRDs. A possible treatment strategy is modeled whereby peptide neutralization of neogenin in Rd1, Rd10, and Rho P23H–knockin mice promotes rod and cone survival and rescues visual function as measured by light-evoked retinal ganglion cell recordings, scotopic/photopic electroretinogram recordings, and visual acuity tests. These results expose neogenin as a critical link between cAMP and photoreceptor death, and identify a druggable target for the treatment of retinal degeneration.
Authors
Jason Charish, Alireza P. Shabanzadeh, Danian Chen, Patrick Mehlen, Santhosh Sethuramanujam, Hidekiyo Harada, Vera L. Bonilha, Gautam Awatramani, Rod Bremner, Philippe P. Monnier
Daxian Wu, Sainan Zhang, Zhongyang Xie, Ermei Chen, Qunfang Rao, Xiaoli Liu, Kaizhou Huang, Jing Yang, Lanlan Xiao, Feiyang Ji, Zhengyi Jiang, Yalei Zhao, Xiaoxi Ouyang, Danhua Zhu, Xiahong Dai, Zhouhua Hou, Bingjie Liu, Binbin Deng, Ning Zhou, Hainv Gao, Zeyu Sun, Lanjuan LiDaxian Wu, Sainan Zhang, Zhongyang Xie, Ermei Chen, Qunfang Rao, Xiaoli Liu, Kaizhou Huang, Jing Yang, Lanlan Xiao, Feiyang Ji, Zhengyi Jiang, Yalei Zhao, Xiaoxi Ouyang, Danhua Zhu, Xiahong Dai, Zhouhua Hou, Bingjie Liu, Binbin Deng, Ning Zhou, Hainv Gao, Zeyu Sun, Lanjuan Li×Abstract
BACKGROUND HBV-related acute-on-chronic liver failure (HBV-ACLF) is hallmarked by high short-term mortality rates, calling for accurate prognostic biomarkers for initial risk stratification.METHODS Three tandem mass tag–labeled (TMT-labeled) quantitative proteomic studies were performed on 10 patients with HBV-related acute hepatic decompensation and on 20 patients with HBV-ACLF. Candidate biomarkers were preliminarily verified in a cross-sectional cohort (n = 144) and further confirmed in 2 prospective cohorts (n = 207 and n = 148).RESULTS Plasminogen, a potential prognostic biomarker for HBV-ACLF, was identified by TMT quantitative proteomics and preliminarily verified in the cross-sectional cohort. Further validation with a prospective cohort (n = 207) showed that plasminogen levels at admission were significantly lower (P < 0.001) in HBV-ACLF nonsurvivors than in survivors. The cumulative survival duration of patients with high plasminogen levels was significantly longer (P < 0.001) than that of patients with low plasminogen levels. During hospitalization, plasminogen levels significantly decreased (P = 0.008) in the deterioration group but significantly increased (P < 0.001) in the improvement group. Additionally, plasminogen levels gradually increased in survivors but gradually decreased in nonsurvivors. The P5 score, a prognostic panel incorporating plasminogen levels, hepatic encephalopathy occurrence, age, international normalized ratio (INR), and total bilirubin, was significantly superior to the Child-Pugh, Model for End-stage Liver Disease (MELD), Chronic Liver Failure Consortium ACLF (CLIF-C ACLF), Chinese Group on the Study of Severe Hepatitis B (COSSH), and HINT (a prognostic score based on hepatic encephalopathy occurrence, INR, neutrophil count, and thyroid-stimulating hormone) scores (all P < 0.05). The performances of the plasminogen level and P5 score were validated in a second multicenter, prospective cohort (n = 148).CONCLUSIONS Plasminogen is a promising prognostic biomarker for HBV-ACLF, and sequential plasminogen measurements could profile the clinical course of HBV-ACLF. P5 is a high-performance prognostic score for HBV-ACLF.FUNDING The National Key Research and Development Program (2017YFC1200204); the National Natural Science Foundation of China (81400589, 81600497); the Foundation for Innovative Research Groups of the National Natural Science Foundation of China (81121002); the Chinese High-Tech Research and Development Programs (2012AA020204); the National S&T Major Project (2012ZX10002004); and the Zhejiang Provincial Medicine and Health Science and Technology Project (2016147735).
Authors
Daxian Wu, Sainan Zhang, Zhongyang Xie, Ermei Chen, Qunfang Rao, Xiaoli Liu, Kaizhou Huang, Jing Yang, Lanlan Xiao, Feiyang Ji, Zhengyi Jiang, Yalei Zhao, Xiaoxi Ouyang, Danhua Zhu, Xiahong Dai, Zhouhua Hou, Bingjie Liu, Binbin Deng, Ning Zhou, Hainv Gao, Zeyu Sun, Lanjuan Li
Min Liu, Zan Tong, Chuanlin Ding, Fengling Luo, Shouzhen Wu, Caijun Wu, Sabrin Albeituni, Liqing He, Xiaoling Hu, David Tieri, Eric C. Rouchka, Michito Hamada, Satoru Takahashi, Andrew A. Gibb, Goetz Kloecker, Huang-ge Zhang, Michael Bousamra II, Bradford G. Hill, Xiang Zhang, Jun YanMin Liu, Zan Tong, Chuanlin Ding, Fengling Luo, Shouzhen Wu, Caijun Wu, Sabrin Albeituni, Liqing He, Xiaoling Hu, David Tieri, Eric C. Rouchka, Michito Hamada, Satoru Takahashi, Andrew A. Gibb, Goetz Kloecker, Huang-ge Zhang, Michael Bousamra II, Bradford G. Hill, Xiang Zhang, Jun Yan×Abstract
Macrophages have been linked to tumor initiation, progression, metastasis, and treatment resistance. However, the transcriptional regulation of macrophages driving the protumor function remains elusive. Here, we demonstrate that the transcription factor c-Maf is a critical controller for immunosuppressive macrophage polarization and function in cancer. c-Maf controls many M2-related genes and has direct binding sites within a conserved noncoding sequence of the Csf-1r gene and promotes M2-like macrophage–mediated T cell suppression and tumor progression. c-Maf also serves as a metabolic checkpoint regulating the TCA cycle and UDP-GlcNAc biosynthesis, thus promoting M2-like macrophage polarization and activation. Additionally, c-Maf is highly expressed in tumor-associated macrophages (TAMs) and regulates TAM immunosuppressive function. Deletion of c-Maf specifically in myeloid cells results in reduced tumor burden with enhanced antitumor T cell immunity. Inhibition of c-Maf partly overcomes resistance to anti–PD-1 therapy in a subcutaneous LLC tumor model. Similarly, c-Maf is expressed in human M2 and tumor-infiltrating macrophages/monocytes as well as circulating monocytes of human non–small cell lung carcinoma (NSCLC) patients and critically regulates their immunosuppressive activity. The natural compound β-glucan downregulates c-Maf expression on macrophages, leading to enhanced antitumor immunity in mice. These findings establish a paradigm for immunosuppressive macrophage polarization and transcriptional regulation by c-Maf and suggest that c-Maf is a potential target for effective tumor immunotherapy.
Authors
Min Liu, Zan Tong, Chuanlin Ding, Fengling Luo, Shouzhen Wu, Caijun Wu, Sabrin Albeituni, Liqing He, Xiaoling Hu, David Tieri, Eric C. Rouchka, Michito Hamada, Satoru Takahashi, Andrew A. Gibb, Goetz Kloecker, Huang-ge Zhang, Michael Bousamra II, Bradford G. Hill, Xiang Zhang, Jun Yan
Ryan J. Ashley, Hongxia Yan, Nan Wang, John Hale, Brian M. Dulmovits, Julien Papoin, Meagan E. Olive, Namrata D. Udeshi, Steven A. Carr, Adrianna Vlachos, Jeffrey M. Lipton, Lydie Da Costa, Christopher Hillyer, Sandrina Kinet, Naomi Taylor, Narla Mohandas, Anupama Narla, Lionel BlancRyan J. Ashley, Hongxia Yan, Nan Wang, John Hale, Brian M. Dulmovits, Julien Papoin, Meagan E. Olive, Namrata D. Udeshi, Steven A. Carr, Adrianna Vlachos, Jeffrey M. Lipton, Lydie Da Costa, Christopher Hillyer, Sandrina Kinet, Naomi Taylor, Narla Mohandas, Anupama Narla, Lionel Blanc×Abstract
Despite the effective clinical use of steroids for the treatment of Diamond Blackfan anemia (DBA), the mechanisms through which glucocorticoids regulate human erythropoiesis remain poorly understood. We report that the sensitivity of erythroid differentiation to dexamethasone is dependent on the developmental origin of human CD34+ progenitor cells, specifically increasing the expansion of CD34+ progenitors from peripheral blood (PB) but not cord blood (CB). Dexamethasone treatment of erythroid-differentiated PB, but not CB, CD34+ progenitors resulted in the expansion of a newly defined CD34+CD36+CD71hiCD105med immature colony-forming unit–erythroid (CFU-E) population. Furthermore, proteomics analyses revealed the induction of distinct proteins in dexamethasone-treated PB and CB erythroid progenitors. Dexamethasone treatment of PB progenitors resulted in the specific upregulation of p57Kip2, a Cip/Kip cyclin–dependent kinase inhibitor, and we identified this induction as critical; shRNA-mediated downregulation of p57Kip2, but not the related p27Kip1, significantly attenuated the impact of dexamethasone on erythroid differentiation and inhibited the expansion of the immature CFU-E subset. Notably, in the context of DBA, we found that steroid resistance was associated with dysregulated p57Kip2 expression. Altogether, these data identify a unique glucocorticoid-responsive human erythroid progenitor and provide new insights into glucocorticoid-based therapeutic strategies for the treatment of patients with DBA.
Authors
Ryan J. Ashley, Hongxia Yan, Nan Wang, John Hale, Brian M. Dulmovits, Julien Papoin, Meagan E. Olive, Namrata D. Udeshi, Steven A. Carr, Adrianna Vlachos, Jeffrey M. Lipton, Lydie Da Costa, Christopher Hillyer, Sandrina Kinet, Naomi Taylor, Narla Mohandas, Anupama Narla, Lionel Blanc
Yadong Xie, Yifan Zhao, Lei Shi, Wei Li, Kun Chen, Min Li, Xia Chen, Haiwei Zhang, Tiantian Li, Yu Matsuzawa-Ishimoto, Xiaomin Yao, Dianhui Shao, Zunfu Ke, Jian Li, Yan Chen, Xiaoming Zhang, Jun Cui, Shuzhong Cui, Qibin Leng, Ken Cadwell, Xiaoxia Li, Hong Wei, Haibing Zhang, Huabin Li, Hui XiaoYadong Xie, Yifan Zhao, Lei Shi, Wei Li, Kun Chen, Min Li, Xia Chen, Haiwei Zhang, Tiantian Li, Yu Matsuzawa-Ishimoto, Xiaomin Yao, Dianhui Shao, Zunfu Ke, Jian Li, Yan Chen, Xiaoming Zhang, Jun Cui, Shuzhong Cui, Qibin Leng, Ken Cadwell, Xiaoxia Li, Hong Wei, Haibing Zhang, Huabin Li, Hui Xiao×Abstract
Although Western diet and dysbiosis are the most prominent environmental factors associated with inflammatory bowel diseases (IBDs), the corresponding host factors and cellular mechanisms remain poorly defined. Here we report that the TSC1/mTOR pathway in the gut epithelium represents a metabolic and innate immune checkpoint for intestinal dysfunction and inflammation. mTOR hyperactivation triggered by Western diet or Tsc1 ablation led to epithelium necroptosis, barrier disruption, and predisposition to dextran sulfate sodium–induced colitis and inflammation-associated colon cancer. Mechanistically, our results uncovered a critical role for TSC1/mTOR in restraining the expression and activation of RIPK3 in the gut epithelium through TRIM11-mediated ubiquitination and autophagy-dependent degradation. Notably, microbiota depletion by antibiotics or gnotobiotics attenuated RIPK3 expression and activation, thereby alleviating epithelial necroptosis and colitis driven by mTOR hyperactivation. mTOR primarily impinged on RIPK3 to potentiate necroptosis induced by TNF and by microbial pathogen-associated molecular patterns (PAMPs), and hyperactive mTOR and aberrant necroptosis were intertwined in human IBDs. Together, our data reveal a previously unsuspected link between the Western diet, microbiota, and necroptosis and identify the mTOR/RIPK3/necroptosis axis as a driving force for intestinal inflammation and cancer.
Authors
Yadong Xie, Yifan Zhao, Lei Shi, Wei Li, Kun Chen, Min Li, Xia Chen, Haiwei Zhang, Tiantian Li, Yu Matsuzawa-Ishimoto, Xiaomin Yao, Dianhui Shao, Zunfu Ke, Jian Li, Yan Chen, Xiaoming Zhang, Jun Cui, Shuzhong Cui, Qibin Leng, Ken Cadwell, Xiaoxia Li, Hong Wei, Haibing Zhang, Huabin Li, Hui Xiao
Jeongeun Hyun, Zhaoli Sun, Ali Reza Ahmadi, Sushant Bangru, Ullas V. Chembazhi, Kuo Du, Tianyi Chen, Hidekazu Tsukamoto, Ivan Rusyn, Auinash Kalsotra, Anna Mae DiehlJeongeun Hyun, Zhaoli Sun, Ali Reza Ahmadi, Sushant Bangru, Ullas V. Chembazhi, Kuo Du, Tianyi Chen, Hidekazu Tsukamoto, Ivan Rusyn, Auinash Kalsotra, Anna Mae Diehl×Abstract
Severe alcoholic hepatitis (SAH) is a deadly liver disease without an effective medical therapy. Although SAH mortality is known to correlate with hepatic accumulation of immature liver cells, why this occurs and how it causes death are unclear. Here, we demonstrate that expression of epithelial splicing regulatory protein 2 (ESRP2), an RNA-splicing factor that maintains the nonproliferative, mature phenotype of adult hepatocytes, was suppressed in both human SAH and various mouse models of SAH in parallel with the severity of alcohol consumption and liver damage. Inflammatory cytokines released by excessive alcohol ingestion reprogrammed adult hepatocytes into proliferative, fetal-like cells by suppressing ESRP2. Sustained loss of ESRP2 permitted reemergence of a fetal RNA-splicing program that attenuates the Hippo signaling pathway and thus allows fetal transcriptional regulators to accumulate in adult liver. We further showed that depleting ESRP2 in mice exacerbated alcohol-induced steatohepatitis, enabling surviving hepatocytes to shed adult hepatocyte functions and become more regenerative, but threatening overall survival by populating the liver with functionally immature hepatocytes. Our findings revealed a mechanism that explains why liver failure develops in patients with the clinical syndrome of SAH, suggesting that recovery from SAH might be improved by limiting adult-to-fetal reprogramming in hepatocytes.
Authors
Jeongeun Hyun, Zhaoli Sun, Ali Reza Ahmadi, Sushant Bangru, Ullas V. Chembazhi, Kuo Du, Tianyi Chen, Hidekazu Tsukamoto, Ivan Rusyn, Auinash Kalsotra, Anna Mae Diehl



Copyright © 2026 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)