Metabolism
Abstract
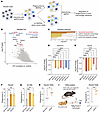
Macrophage-mediated phagocytosis plays a critical role in the elimination of cancer cells and shaping antitumor immunity. However, the tumor-intrinsic pathways that regulate cancer cell sensitivity to macrophage-mediated phagocytosis remain poorly defined. In this study, we performed a genome-wide CRISPR screen in murine pancreatic cancer cells cocultured with primary macrophages and identified that disruption of the tumor-intrinsic pyrimidine synthesis pathway enhances phagocytosis. Mechanistically, we discovered that macrophages inhibit the pyrimidine salvage pathway in tumor cells by upregulating Upp1-mediated uridine degradation through cytokines TNF-α and IL-1. This shift increased tumor cells’ reliance on de novo pyrimidine synthesis. As a result, tumor cells with impaired de novo pyrimidine synthesis showed depleted UMP and displayed enhanced exposure of phosphatidylserine (PtdSer), a major “eat-me” signal, thereby promoting macrophage-mediated phagocytosis. In multiple pancreatic cancer models, Cad-deficient tumors exhibited markedly reduced tumor burden with increased levels of phagocytosis by macrophages. Importantly, the Cad-mediated suppression of pancreatic cancer was dependent on TAMs and cytokines IL-1 and TNF-α. Pharmacological inhibition of DHODH, which blocks de novo pyrimidine synthesis, similarly decreased tumor burden with enhanced phagocytosis in pancreatic cancer models. These findings highlight the critical role of the tumor-intrinsic pyrimidine synthesis pathway in modulating macrophage-mediated antitumor immunity, with potential therapeutic implications.
Authors
Jie Zhao, Xinghao Li, Xinyu Li, Pengfei Ren, Yilan Wu, Hao Gong, Lijian Wu, Junran Huang, Saisai Wang, Ziwei Guo, Mo Chen, Zexian Zeng, Deng Pan
Abstract
Familial partial lipodystrophy 2 (FPLD2) is a rare disease characterized by adipose tissue loss and redistribution, and metabolic dysfunction. FPLD2 is caused by pathogenic variants in the LMNA gene, encoding nuclear lamins A/C, structural proteins that control nuclear function and gene expression. However, the mechanisms driving adipocyte loss in FPLD2 remain poorly defined. In this study, we recruited eight families with developing or established FPLD2 and performed clinical, histological, and transcriptomic analyses of subcutaneous adipose tissue biopsies. Bulk and single-nuclei RNA-sequencing revealed suppression of lipid metabolism and mitochondrial pathways, alongside increased inflammation. These signatures were mirrored in tamoxifen-inducible adipocyte-specific Lmna knockout mice, in which lamin A/C-deficient adipocytes shrank and disappeared. Lmna-deficient fibroblasts shared similar gene expression changes, linked to altered chromatin accessibility, underscoring lamin A/C’s potential regulatory role in lipid metabolism and inflammatory programs. By directly comparing atrophic and hypertrophic adipose depots in FPLD2, and integrating human, mouse, and in vitro models, this study provides new insights into disease progression and potential therapeutic targets.
Authors
Jessica N. Maung, Rebecca L. Schill, Akira Nishii, Maria Foss de Freitas, Bonje N. Obua, Marcus Nygård, Maria D. Mendez-Casillas, Isabel D.K. Hermsmeyer, Donatella Gilio, Ozge Besci, Yang Chen, Brian Desrosiers, Rose E. Adler, Anabela D. Gomes, Merve Celik Guler, Hiroyuki Mori, Romina M. Uranga, Ziru Li, Hadla Hariri, Liping Zhang, Anderson de Paula Souza, Keegan S. Hoose, Kenneth T. Lewis, Taryn A. Hetrick, Paul Cederna, Carey N. Lumeng, Susanne Mandrup, Elif A. Oral, Ormond A. MacDougald
Abstract
Sulfite oxidase (SOX) deficiency is a rare inborn error of cysteine metabolism resulting in severe neurological damage. In patients, sulfite accumulates to toxic levels, causing a rise in the downstream products S-sulfocysteine, which mediates excitotoxicity, and thiosulfate, a catabolic intermediate/product of hydrogen sulfide (H2S) metabolism. Here, we report a full-body knockout mouse model for SOX deficiency (SOXD) with a severely impaired phenotype. Among the urinary biomarkers, thiosulfate showed a 45-fold accumulation in SOXD mice, representing the major excreted S-metabolite. Consistently, we found increased plasma H2S, which was derived from sulfite-induced release from persulfides, as demonstrated in vitro and in vivo. Mass spectrometry analysis of total protein persulfidome identified a major loss of S-persulfidation in 20% of the proteome, affecting enzymes in amino acids, fatty acid metabolism, and cytosolic iron-sulfur cluster biogenesis. Urinary amino acid profiles indicated metabolic rewiring and mitochondrial dysfunction, thus identifying an altered H2S metabolism and persulfidation in SOXD. Finally, oxidized glutathione and glutathione trisulfide were able to scavenge sulfite in vitro and in vivo, extending the lifespan of SOXD mice and providing a mechanistic concept of sulfite scavenging for the treatment of this severe metabolic disorder of cysteine catabolism.
Authors
Chun-Yu Fu, Joshua B. Kohl, Filip Liebsch, Davide D’Andrea, Tamás Ditrói, Seiryo Ogata, Franziska Neuser, Max Mai, Anna T. Mellis, Emilia Kouroussis, Masanobu Morita, Titus Gehling, José Angel Santamaria-Araujo, Sin Yuin Yeo, Heike Endepols, Michaela Křížková, Viktor Kozich, Marcus Krueger, Julia B. Hennermann, Uladzimir Barayeu, Takaaki Akaike, Peter Nagy, Milos Filipovic, Guenter Schwarz
Abstract
Obesity is a major driver of type 2 diabetes (T2D) and related metabolic disorders, characterized by chronic inflammation and adipocyte dysfunction. However, the molecular triggers initiating these processes remain poorly understood. We identify FAM20C, a serine/threonine kinase, as an early obesity-induced mediator of adipocyte dysfunction. Fam20c expression is substantially upregulated in adipocytes in response to obesity, correlating with a proinflammatory transcriptional signature. Forced expression of Fam20c in adipocytes promotes robust upregulation of proinflammatory cytokines and induces insulin resistance that is dependent on its kinase activity. Conversely, deletion of adipocyte Fam20c after established obesity and hyperglycemia improves glucose tolerance, augments insulin sensitivity, and reduces visceral adiposity, without altering body weight. Phosphoproteomic studies reveal that FAM20C regulates phosphorylation of intracellular and secreted proteins, modulating pathways critical to inflammation, metabolism, and extracellular matrix remodeling. We identify FAM20C-dependent substrates, such as CNPY4, whose phosphorylation contributes to proinflammatory adipocyte signaling. Of translational relevance, we show that in humans visceral adipose FAM20C expression positively correlates with insulin resistance. Our findings establish FAM20C as an early regulator of obesity-induced adipocyte dysfunction and systemic metabolic impairment. Our studies provide proof of concept that inhibition of FAM20C may serve as a potential therapy for T2D by restoring adipocyte health.
Authors
Ankit Gilani, Benjamin D. Stein, Anne Hoffmann, Renan Pereira de Lima, Elizabeth E. Ha, Edwin A. Homan, Lunkun Ma, Alfonso Rubio-Navarro, Tint Tha Ra Wun, Gabriel Jose Ayala Carrascal, Bhavneet Bhinder, Adhideb Ghosh, Falko J. Noé, Olivier Elemento, Christian Wolfrum, Matthias Blüher, James C. Lo
Abstract
Deposits of hydroxyapatite called Randall's plaques are found in the renal papilla of calcium oxalate kidney stone formers and likely serve as the nidus for stone formation, but their pathogenesis is unknown. Claudin-2 is a paracellular ion channel that mediates calcium reabsorption in the renal proximal tubule. To investigate the role of renal claudin-2, we generated kidney tubule-specific claudin-2 conditional knockout mice (KS-Cldn2 KO). KS-Cldn2 KO mice exhibited transient hypercalciuria in early life. Normalization of urine calcium was accompanied by a compensatory increase in expression and function of renal tubule calcium transporters, including in the thick ascending limb. Despite normocalciuria, KS-Cldn2 KO mice developed papillary hydroxyapatite deposits, beginning at 6 months of age, that resembled Randall's plaques and tubule plugs. Bulk chemical tissue analysis and laser ablation-inductively coupled plasma mass spectrometry revealed a gradient of intrarenal calcium concentration along the corticomedullary axis in normal mice, that was accentuated in KS-Cldn2 KO mice. Our findings provide evidence for the “vas washdown” hypothesis for Randall's plaque formation, and identify the corticomedullary calcium gradient as a target for therapies to prevent kidney stone disease.
Authors
Christine V. Behm, Duuamene Nyimanu, Ony Araujo Galdino, Sadhana Kanoo, Young Chul Kim, Natalia Lopez, Helen Goodluck, Peter S. Rowe, Andrew P. Evan, André J. Sommer, Matthew N. Barr, Tracy Punshon, Volker Vallon, Brian P. Jackson, James C. Williams Jr., Alan S.L. Yu
Abstract
In peripheral tissues, an endothelial cell (EC) protein, GPIHBP1, captures lipoprotein lipase (LPL) from the interstitial spaces and transports it to the capillary lumen. LPL mediates the margination of triglyceride-rich (TG-rich) lipoproteins (TRLs) along capillaries, allowing the lipolytic processing of TRLs to proceed. TRL-derived fatty acids are used for fuel in oxidative tissues or stored in adipose tissue. In mice, GPIHBP1 is absent from capillary ECs of the brain (which uses glucose for fuel); consequently, LPL and TRL margination are absent in mouse brain capillaries. However, because fatty acids were reported to play signaling roles in the brain, we hypothesized that LPL-mediated TRL processing might occur within specialized vascular beds within the central nervous system. Here, we show that GPIHBP1 is expressed in capillary ECs of human and mouse choroid plexus (ChP) and that GPIHBP1 transports LPL (produced by adjacent ChP cells) to the capillary lumen. The LPL in ChP capillaries mediates both TRL margination and processing. Intracapillary LPL and TRL margination are absent in the ChP of Gpihbp1–/– mice. GPIHBP1 expression, intracapillary LPL, and TRL margination were also observed in the median eminence and subfornical organ, circumventricular organs implicated in the regulation of food intake.
Authors
Wenxin Song, Madison Hung, Ellen Kozlov, Megan Hung, Anh P. Tran, James Carroll, Le Phoung Nguyen, Troy L. Lowe, Paul Kim, Hyesoo Jung, Yiping Tu, Joonyoung Kim, Ashley M. Presnell, Julia Scheithauer, Jenna P. Koerner, Ye Yang, Shino D. Magaki, Christopher K. Williams, Michael Ploug, Haibo Jiang, Christer Betsholtz, Maarja Andaloussi Mäe, Liqun He, Anne P. Beigneux, Loren G. Fong, Stephen G. Young
Abstract
Clinically, blockade of renal glucose resorption by sodium–glucose cotransporter 2 (SGLT2) inhibitors slows progression of kidney disease, yet the underlying mechanisms are not fully understood. We hypothesized that altered renal metabolites underlie observed kidney protection when SGLT2 function is lost. S-adenosylmethionine (SAM) levels were increased in kidneys from mice lacking SGLT2 function on a diabetogenic high-fat diet (SPHFD) compared with WT mice fed HFD. Elevated SAM in SPHFD was associated with improved kidney function and decreased expression of NF-κB pathway–related genes. Injured proximal tubular cells that emerged under HFD conditions in WT mice and humans consistently showed reduction in expression of the SAM synthetase Mat2a/MAT2A, while MAT2A inhibition, which reduces SAM production, abrogated kidney protection in SPHFD mice. Histone H3 lysine 27 (H3K27) repressive trimethylation of NF-κB–related genes was increased in SPHFD, consistent with SAM’s role as a methyl donor. Our data support a model whereby SGLT2 loss enhances SAM levels within the kidney, leading to epigenetic repression of inflammatory genes and kidney protection under metabolic stress.
Authors
Hiroshi Maekawa, Yalu Zhou, Yuki Aoi, Margaret E. Fain, Dorian S. Kaminski, Hyewon Kong, Zachary L. Sebo, Ram P. Chakrabarty, Benjamin C. Howard, Grant Andersen, Biliana Marcheva, Peng Gao, Pinelopi Kapitsinou, Joseph Bass, Ali Shilatifard, Navdeep S. Chandel, Susan E. Quaggin
Abstract
Metabolic dysfunction-associated steatohepatitis (MASH) is a progressive liver disease characterized by complex interactions between lipotoxicity, ER stress responses, and immune-mediated inflammation. We identified enrichment of the proinflammatory alarmin S100 calcium-binding protein A11 (S100A11) on extracellular vesicles stimulated by palmitate-induced lipotoxic ER stress with concomitant upregulation of hepatocellular S100A11 abundance in an IRE1A-XBP1s dependent manner. We next investigated the epigenetic mechanisms that regulate this stress response. Publicly available human liver ChIP-Seq GEO datasets demonstrated a region of histone H3 lysine 27 (H3K27) acetylation upstream to the S100A11 promoter. H3K27acetylation ChIP-qPCR demonstrated a positive correlation between lipotoxic ER stress and H3K27acetylation of the region, which we termed Lipotoxicity Influenced Enhancer (LIE) domain. CRISPR-mediated repression of the LIE domain reduced palmitate-induced H3K27acetylation and corresponding S100A11 upregulation in Huh7 cells and immortalized mouse hepatocytes. Silencing of the murine LIE in two independent steatohepatitis models demonstrated reduced S100a11 upregulation and attenuated liver injury. We confirmed H3K27acetylation and XBP1s occupancy at the LIE domain in human MASH liver samples and an increase in hepatocyte-derived S100A11-enriched extracellular vesicles in MASH patient plasma. Our studies demonstrate a LIE domain which mediates hepatic S100A11 upregulation. This pathway may be a potential therapeutic target in MASH.
Authors
P. Vineeth Daniel, Hanna L. Erickson, Daheui Choi, Feda H. Hamdan, Yasuhiko Nakao, Gyanendra Puri, Takahito Nishihara, Yeriel Yoon, Amy S. Mauer, Debanjali Dasgupta, Jill Thompson, Alexander Revzin, Harmeet Malhi
Abstract
Authors
Bowen Yan, Qingchen Yuan, Marco M. Buttigieg, Prabhjot Kaur, Annalisse R. McKee, Daniil E. Shabashvili, Caitlyn Vlasschaert, Alexander G. Bick, Michael J. Rauh, Olga A. Guryanova
Abstract
Regulatory T-cells (Treg) are critical for maintaining immune homeostasis, and their adoptive transfer can treat murine inflammatory disorders. In patients, Treg therapies have been variably efficacious. Therefore, new strategies to enhance Treg therapeutic efficacy are needed. Treg predominantly depend upon oxidative phosphorylation (OXPHOS) for energy and suppressive function. Fatty acid oxidation (FAO) contributes to Treg OXPHOS and can be important for Treg “effector” differentiation, but FAO activity is inhibited by coordinated activity of isoenzymes acetyl-CoA Carboxylase-1 and -2 (ACC1/2). Here, we show that small molecule inhibition or Treg-specific genetic deletion of ACC1 significantly increases Treg suppressive function in vitro and in mice with established chronic GVHD. ACC1 inhibition skewed Treg towards an “effector” phenotype and enhanced FAO-mediated OXPHOS, mitochondrial function, and mitochondrial fusion. Inhibiting mitochondrial fusion diminished the effect of ACC1 inhibition. Reciprocally, promoting mitochondrial fusion, even in the absence of ACC1 modulation, resulted in a Treg functional and metabolic phenotype similar to ACC1 inhibition, indicating a key role for mitochondrial fusion in Treg suppressive potency. Ex vivo expanded, ACC1 inhibitor treated human Treg similarly augmented suppressor function as observed with murine Treg. Together, these data suggest that ACC1 manipulation may be exploited to modulate Treg function in patients.
Authors
Cameron McDonald-Hyman, Ethan G. Aguilar, Ewoud B. Compeer, Michael C. Zaiken, Stephanie Y. Rhee, Fathima A. Mohamed, Jemma H. Larson, Michael L. Loschi, Christopher Lees, Govindarajan Thangavelu, Margaret L. Sleeth, Kyle D. Smith, Jennifer S. Whangbo, Jerome Ritz, Tim D. Sparwasser, Roddy S. O'Connor, Peter A. Crawford, Jeffrey C. Rathmell, Leslie S. Kean, Robert Zeiser, Keli L. Hippen, Michael L. Dustin, Bruce R. Blazar



Copyright © 2025 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)