Issue published May 15, 2026 Previous issue

On the cover: Metastatic tropism of clear-cell renal cell carcinoma
Haddad et al. report a comprehensive analysis of kidney cancer tumor burden, demonstrating that the anatomic distribution of metastases relates to molecular clusters associated with response to specific therapies. Image illustrated by Elsa Pedrosa.
-
Reviews
×
Abstract
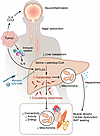
Anemia affects one-third of the population globally and is marked by impaired erythropoiesis that results in substantial mortality and morbidity. Over the past few decades, our understanding of the molecular mechanisms underlying anemia has progressed but translating that knowledge into effective targeted therapeutics remains challenging. Preclinical and clinical studies substantiate the efficacy of modulating erythropoietin-driven signaling pathways to stimulate erythropoiesis. Additional approaches include strategies to maintain iron homeostasis and control iron metabolism, using small molecules and oral supplements. New frontiers in molecular regulation of anemia include perturbation of regulatory genes and spliceosome proteins in erythroid cells, as well as mutation-specific therapeutic approaches. Finally, new evidence supporting the importance of neuronal signaling and mitochondrial dynamics in shaping erythropoiesis is pointing toward novel interventions. Here, we discuss the molecular and genetic factors underlying defective erythropoiesis and highlight current and emerging therapies, including molecular targets to overcome drug resistance.
Authors
Nilesh Rai, Omar Abdel-Wahab, Lingbo Zhang
Andrew T. Hale, Adam J. Kundishora, Pazhanichamy Kalailingam, Tanyeri Barak, Phan Q. Duy, Christopher M. Ramundo, Baojian Fan, Qiang Li, Priscilla K. Brastianos, Ganesh M. Shankar, Seth L. Alper, Benjamin P. Kleinstiver, Patricia L. Musolino, Kristopher T. KahleAndrew T. Hale, Adam J. Kundishora, Pazhanichamy Kalailingam, Tanyeri Barak, Phan Q. Duy, Christopher M. Ramundo, Baojian Fan, Qiang Li, Priscilla K. Brastianos, Ganesh M. Shankar, Seth L. Alper, Benjamin P. Kleinstiver, Patricia L. Musolino, Kristopher T. Kahle×Abstract
Recent advances in cerebrovascular genomics, single-cell biology, pharmacology, and gene editing technology are transforming our understanding of brain arteriovenous malformations (bAVMs) — a leading cause of pediatric hemorrhagic stroke. Once considered static anatomical defects, bAVMs are now recognized as dynamic, genetically driven lesions resulting from somatic mutations in KRAS, BRAF, and pathways involved in arteriovenous specification, angiogenesis, and vascular remodeling. By integrating human genetics, animal models, and endovascular innovations, researchers have uncovered convergent mechanisms that link endothelial Ras/MAPK hyperactivation to abnormal vessel growth and higher rupture risk. These insights provide a foundation for precision medicine approaches that combine molecular diagnostics — such as liquid or endoluminal biopsies — with mutation-specific pharmacotherapies and emerging CRISPR-based gene editing strategies. We suggest that genotype-guided interventions, tailored by spatial and developmental cerebrovascular context, could ultimately reclassify bAVMs from surgically incurable malformations to treatable molecular conditions.
Authors
Andrew T. Hale, Adam J. Kundishora, Pazhanichamy Kalailingam, Tanyeri Barak, Phan Q. Duy, Christopher M. Ramundo, Baojian Fan, Qiang Li, Priscilla K. Brastianos, Ganesh M. Shankar, Seth L. Alper, Benjamin P. Kleinstiver, Patricia L. Musolino, Kristopher T. Kahle
×Abstract
Type 1 diabetes mellitus (T1D) has been recognized as a chronic autoimmune disease for five decades, but therapy has relied on the exogenous replacement of insulin, which is an imperfect substitute for normal β cell function. In recent years, there has been progress in the development of new therapeutics that target the primary causes of the disease: failed immunologic tolerance and β cell killing. One agent, teplizumab, was shown to attenuate loss of β cell function that occurs over time and delay progression to clinical disease in individuals at risk, leading to its regulatory approval in 2022. Other immunologic agents show promise in modulating the immunologic imbalance. Moreover, a role for β cells in T1D pathogenesis has been identified and may be targeted. Now that the first disease-modifying therapeutic agent is available, future studies may involve combinations of agents to extend immunologic tolerance and protect and restore β cells so that lasting metabolic remission can be achieved.
Authors
Kevan C. Herold, Carmella Evans-Molina
-
Commentaries
×
Abstract
Glioma stem cells (GSCs) are a small subset of self-renewing, plastic, and multipotent neoplastic cells in glioblastoma (GBM) that sit at the apex of a cellular differentiation hierarchy. Elucidating pathways that enhance GSC properties and determine their cell-specific interactions within the immunosuppressive GBM microenvironment are critical for developing effective therapeutic approaches. The CLOCK-BMAL1 complex, which is well known for its activity as a circadian rhythm–regulating transcription factor, plays a critical role in maintaining GSC stemness, and the gene encoding CLOCK was found to be amplified in about 5% of GBM cases. Here, Zhou et al. have uncovered a “symbiotic exclusivity” relationship between CLOCK-BMAL1 and TFPI2, which is also amplified in a small proportion of GBM cases. This relationship forms a HIF-1α/NF-κB P65–mediated positive feedback loop that boosts the proliferative and tumor-enhancing capacities of GSC and immunosuppressive microglia. This self-amplifying regulatory circuit represents an opportunity for intervention to inhibit GBM growth.
Authors
Petros Basakis, Ling-kai Shih, Jiabo Li, Daniel J. Brat
×Abstract
Clinical management of pancreatic cancer (PC) remains severely limited, primarily due to the complex tumor microenvironment. Emerging DNA damage–targeted strategies have demonstrated considerable therapeutic potential in PC. In this issue of the JCI, Teh et al. employed cancer-specific multitarget sgRNAs to induce DNA double-strand breaks (DSBs), resulting in lethal effects in PC cells. Integrative bioinformatic and cytogenetic analyses revealed that CRISPR/Cas9-mediated DSBs provoked persistent chromosomal instability, ultimately leading to chromosome catastrophe and cell death. Compared with equivalent radiation-induced DSBs, these sgRNAs exhibited superior cytotoxicity and were able to eliminate cells resistant to a specific sgRNA via subsequent targeting at distinct genomic sites, highlighting a promising and innovative precision therapeutic approach for clinical treatment of PC.
Authors
Li-Chan Chang, Christine E. Eyler, Chang-Lung Lee
×Abstract
Cancer cachexia, characterized by weight loss, muscle wasting, and anorexia, complicates cancer treatment and adversely affects patient outcomes. Both tumor-derived and host inflammatory factors are implicated in aspects of cachexia. The search for circulating mediators of cancer cachexia has focused largely on secreted proteins, but metabolites may also drive systemic wasting. In this issue, Morigny, Rohm, and colleagues identified the liver as a major source of circulating ceramides in cachectic mice and patients with cancer and demonstrated that inhibiting ceramide synthesis attenuated muscle wasting and preserved function in cachectic mice. These findings position the liver as an endocrine organ in cachexia and introduce a druggable metabolic pathway with translational potential.
Authors
Kerui Huang, Norbert Perrimon, Marcus D. Goncalves
×Abstract
Immune checkpoint inhibitors (ICIs) have improved patient outcomes substantially in non–small cell lung cancer (NSCLC). Despite considerable effort, our understanding of the features that predict for immunotherapy response and resistance in patients remains incomplete. In this issue of the JCI, Isomoto and colleagues utilized a multiplex IHC platform to profile the spatial organization of the lung cancer tumor immune microenvironment, enabling the identification of spatial immune features that correlate with immunotherapy efficacy. This study enhances our knowledge of the spatial organization of features impacting ICI efficacy by identifying a three-variable spatial composite — including CD73 upregulation in EGFR-mutant NSCLC — that substantially outperforms PD-L1 expression in predicting immunotherapy efficacy. Moreover, it establishes spatial proteomic profiling as a platform for generating therapeutic hypotheses that are actionable and mechanistic in NSCLC.
Authors
Tao Zou, John D. Minna
-
Research Letters
Fumihiko Urano, Bess A. Marshall, Stacy Hurst, Amy Robichaux-Viehoever, Saumel Ahmadi, Tamara Hershey, Gregory Van Stavern, Paulina Cruz Bravo, Jennifer Powers Carson, John Pesko, Kelly Fox, Nathalie Erpelding, Camille L. BedrosianFumihiko Urano, Bess A. Marshall, Stacy Hurst, Amy Robichaux-Viehoever, Saumel Ahmadi, Tamara Hershey, Gregory Van Stavern, Paulina Cruz Bravo, Jennifer Powers Carson, John Pesko, Kelly Fox, Nathalie Erpelding, Camille L. Bedrosian×
Abstract
Authors
Fumihiko Urano, Bess A. Marshall, Stacy Hurst, Amy Robichaux-Viehoever, Saumel Ahmadi, Tamara Hershey, Gregory Van Stavern, Paulina Cruz Bravo, Jennifer Powers Carson, John Pesko, Kelly Fox, Nathalie Erpelding, Camille L. Bedrosian
Larissa Mendes, Peter F. Dutey-Magni, Emily Grist, Ashwin Sachdeva, Sara Santos Vidal, Sharanpreet Lall, Marina A. Parry, Claire L. Amos, Nafisah Atako, Anna Wingate, Daniel Wetterskog, Matthew R. Sydes, Chris C. Parker, Noel Clarke, Christopher J. Sweeney, Mahesh K. Parmar, Louise C. Brown, Nicholas D. James, Daniel M. Berney, Gerhardt AttardLarissa Mendes, Peter F. Dutey-Magni, Emily Grist, Ashwin Sachdeva, Sara Santos Vidal, Sharanpreet Lall, Marina A. Parry, Claire L. Amos, Nafisah Atako, Anna Wingate, Daniel Wetterskog, Matthew R. Sydes, Chris C. Parker, Noel Clarke, Christopher J. Sweeney, Mahesh K. Parmar, Louise C. Brown, Nicholas D. James, Daniel M. Berney, Gerhardt Attard×Abstract
Authors
Larissa Mendes, Peter F. Dutey-Magni, Emily Grist, Ashwin Sachdeva, Sara Santos Vidal, Sharanpreet Lall, Marina A. Parry, Claire L. Amos, Nafisah Atako, Anna Wingate, Daniel Wetterskog, Matthew R. Sydes, Chris C. Parker, Noel Clarke, Christopher J. Sweeney, Mahesh K. Parmar, Louise C. Brown, Nicholas D. James, Daniel M. Berney, Gerhardt Attard
-
Research Articles
Brooke A. Christensen, Jennifer Tat, Michael Z. Leonard, Soren D. Emerson, Shemuel Roberts, Eleanor B. Holmgren, Ainoa Konomi-Pilkati, Hannah B. Reiley, Devan M. Gomez, Lin Zheng, Hye Jean Yoon, Sofia H. Lago, Abigail L. Carr, Lillian J. Brady, Maxime Chevée, Erin S. CalipariBrooke A. Christensen, Jennifer Tat, Michael Z. Leonard, Soren D. Emerson, Shemuel Roberts, Eleanor B. Holmgren, Ainoa Konomi-Pilkati, Hannah B. Reiley, Devan M. Gomez, Lin Zheng, Hye Jean Yoon, Sofia H. Lago, Abigail L. Carr, Lillian J. Brady, Maxime Chevée, Erin S. Calipari×
Abstract
Stimulant medications are widely prescribed for attention deficit hyperactivity disorder (ADHD) and have significant abuse liability. Here, we show that, consistent with clinical data, female mice exhibited enhanced behavioral sensitivity to stimulants, and we define sex- and hormone-dependent adaptations in the dopamine system that contributed to these effects. Single-nucleus RNA-seq of ventral tegmental area dopamine neurons revealed that projections to the nucleus accumbens (NAc) core, compared with other projection populations, were a hub of sexually dimorphic gene expression, including transcripts regulating dopamine synthesis, and transport. These molecular differences coincided with enhanced dopamine release and clearance in female mice, particularly during phases of the estrous cycle when estradiol levels were high. The stimulants amphetamine (a releaser) and methylphenidate (a reuptake inhibitor) more effectively increased dopamine levels in female mice under certain conditions. However, amphetamine showed more robust hormone-sensitive regulation, with potency reduced by ovariectomy and restored by direct estradiol replacement in the NAc core. Together, the findings indicate that even within a drug class, drugs with different mechanisms of action can leverage different aspects of sexually dimorphic dopamine function. This distinction highlights the notion that sex differences are not uniform but can be differentially sensitive to drug pharmacology.
Authors
Brooke A. Christensen, Jennifer Tat, Michael Z. Leonard, Soren D. Emerson, Shemuel Roberts, Eleanor B. Holmgren, Ainoa Konomi-Pilkati, Hannah B. Reiley, Devan M. Gomez, Lin Zheng, Hye Jean Yoon, Sofia H. Lago, Abigail L. Carr, Lillian J. Brady, Maxime Chevée, Erin S. Calipari
Siddharth K. Shenoy, Mark Gutay, Ian Brown, Troy D. Rogers, Kane Banner, Nico Olegario, Nicholas Griffin, Henry P. Goodell, Bryan Yoder, David S. Lalush, David A. Edwards, Richard C. Boucher, Barbara R. Grubb, Brian ButtonSiddharth K. Shenoy, Mark Gutay, Ian Brown, Troy D. Rogers, Kane Banner, Nico Olegario, Nicholas Griffin, Henry P. Goodell, Bryan Yoder, David S. Lalush, David A. Edwards, Richard C. Boucher, Barbara R. Grubb, Brian Button×Abstract
Airway mucus clearance from the lungs occurs by 2 widely recognized mechanisms: cilia-mediated clearance and high-velocity airflow-mediated cough clearance. However, a potentially important third mechanism of mucus clearance, referred to as cilia-independent gas–liquid transport (GLT), was proposed based on in vitro model systems to occur during normal tidal breathing but has largely been overlooked. We conducted in vitro and in vivo studies to investigate the role of tidal breathing airflow rates in mucus clearance. An in vitro airway culture bead-tracking model demonstrated airflow-dependent mucus transport at tidal breathing flow rates. As with other modes of mucus clearance, GLT was critically dependent on mucus concentration. In vivo studies in cilial beat-deficient mice demonstrated that GLT-mediated mucus clearance occurs during tidal breathing in the absence of cough, and the rate of GLT mucus clearance was dependent on breathing frequency and body orientation. These studies demonstrated that GLT is a third mechanism of mucus clearance and likely represents a significant mode of clearance in persons with cilial dysfunction. These findings indicate that increasing breathing rates through exercise, using mucus rehydrating agents or mucolytics, or combining these approaches may restore clinically and physiologically meaningful airway clearance in these patients.
Authors
Siddharth K. Shenoy, Mark Gutay, Ian Brown, Troy D. Rogers, Kane Banner, Nico Olegario, Nicholas Griffin, Henry P. Goodell, Bryan Yoder, David S. Lalush, David A. Edwards, Richard C. Boucher, Barbara R. Grubb, Brian Button
Selina Shiqing K. Teh, Akhil Kotwal, Alexis Bennett, Eitan Halper-Stromberg, Laura Morsberger, Saum Zamani, Yanan Shi, Alyza Skaist, Qingfeng Zhu, Kirsten Bowland, Hong Liang, Ralph H. Hruban, Chien-Fu Hung, Robert A. Anders, Nicholas J. Roberts, Robert B. Scharpf, Michael Goldstein, Ying S. Zou, James R. EshlemanSelina Shiqing K. Teh, Akhil Kotwal, Alexis Bennett, Eitan Halper-Stromberg, Laura Morsberger, Saum Zamani, Yanan Shi, Alyza Skaist, Qingfeng Zhu, Kirsten Bowland, Hong Liang, Ralph H. Hruban, Chien-Fu Hung, Robert A. Anders, Nicholas J. Roberts, Robert B. Scharpf, Michael Goldstein, Ying S. Zou, James R. Eshleman×Abstract
While radiation is an effective oncologic therapy, killing cancer by inducing DNA double-strand breaks (DSBs), it lacks specificity for neoplastic cells. We have previously adapted the CRISPR/Cas9 gene-editing technology as a cancer-specific treatment modality targeting somatic mutations in pancreatic cancer (PC). However, its tumoricidal potential remains unclear, especially in comparison with therapeutic doses of radiation. Here, we demonstrate that CRISPR/Cas9-induced DSBs are more cytotoxic in PCs than a comparable number of radiation-induced DSBs. We observed more than 90% tumor growth inhibition by targeting 9 sites with cancer-specific sgRNAs. Through both bioinformatics and cytogenetics analyses, we found that CRISPR/Cas9-induced DSBs triggered ongoing chromosomal rearrangements, with 87% of structural variants not directly produced from the initial CRISPR/Cas9-induced DSBs, and chromosomal instability peaking before cell death. By comparing the cytotoxicity of CRISPR/Cas9- and radiation-induced DSBs, we demonstrated that the number of DSBs required to achieve equitoxic effects was approximately 3 times higher for radiation than CRISPR/Cas9. Finally, we showed that PC cells that had survived CRISPR/Cas9 targeting retained susceptibility to subsequent CRISPR/Cas9-induced DSBs at different genomic sites with more than 87% growth inhibition. Together, our data support the therapeutic potential of CRISPR/Cas9 as an anticancer strategy.
Authors
Selina Shiqing K. Teh, Akhil Kotwal, Alexis Bennett, Eitan Halper-Stromberg, Laura Morsberger, Saum Zamani, Yanan Shi, Alyza Skaist, Qingfeng Zhu, Kirsten Bowland, Hong Liang, Ralph H. Hruban, Chien-Fu Hung, Robert A. Anders, Nicholas J. Roberts, Robert B. Scharpf, Michael Goldstein, Ying S. Zou, James R. Eshleman
Tae Wan Kim, Jinghua Piao, Vittoria D. Bocchi, So Yeon Koo, Se Joon Choi, Fayzan Chaudhry, Donghe Yang, Hyein S. Cho, Emiliano Hergenreder, Lucia Ruiz Perera, Subhashini Joshi, Zaki Abou Mrad, Nidia Claros, Shkurte Ademi Donohue, Yeong Eun Im, Hyo Jae Jeong, Anika K. Frank, Ryan M. Walsh, Eugene V. Mosharov, Doron Betel, Viviane Tabar, Lorenz StuderTae Wan Kim, Jinghua Piao, Vittoria D. Bocchi, So Yeon Koo, Se Joon Choi, Fayzan Chaudhry, Donghe Yang, Hyein S. Cho, Emiliano Hergenreder, Lucia Ruiz Perera, Subhashini Joshi, Zaki Abou Mrad, Nidia Claros, Shkurte Ademi Donohue, Yeong Eun Im, Hyo Jae Jeong, Anika K. Frank, Ryan M. Walsh, Eugene V. Mosharov, Doron Betel, Viviane Tabar, Lorenz Studer×Abstract
While clinical trials of human pluripotent stem cell–derived midbrain dopamine (mDA) neuron precursor grafts for Parkinson’s disease (PD) are ongoing, current protocols remain suboptimal. In particular, the yield of TH+ mDA neurons after in vivo grafting and the expression of certain mDA neuron and subtype-specific markers require improvement. Single-cell transcriptomic analyses of grafts have revealed low proportions of mDA neurons and substantial off-target contamination. Here, we present an optimized mDA neuron differentiation strategy that builds on our clinical-grade (“Boost”) protocol by adding FGF18 and IWP2 treatment (“Boost+”) at the neurogenesis stage. Boost+ mDA neurons show higher expression of EN1, PITX3, and ALDH1A1. Improvements in mDA neuron yield and transcriptional similarity to primary mDA neurons are observed in vitro and following transplantation. Single-nucleus RNA sequencing demonstrates enrichment of A9 mDA neurons within Boost+ grafts. Functional studies in vitro demonstrate increased dopamine production and release and improved electrophysiological properties. In vivo analyses show higher percentages of TH+ mDA neurons, resulting in efficient rescue of amphetamine-induced rotation behavior in the 6-OHDA rat model and rescue of deficits in some nondrug-induced assays, including the ladder rung assay, which are not improved by Boost mDA neurons. The Boost+ conditions present an optimized differentiation protocol with advantages for disease modeling and mDA neuron grafting paradigms.
Authors
Tae Wan Kim, Jinghua Piao, Vittoria D. Bocchi, So Yeon Koo, Se Joon Choi, Fayzan Chaudhry, Donghe Yang, Hyein S. Cho, Emiliano Hergenreder, Lucia Ruiz Perera, Subhashini Joshi, Zaki Abou Mrad, Nidia Claros, Shkurte Ademi Donohue, Yeong Eun Im, Hyo Jae Jeong, Anika K. Frank, Ryan M. Walsh, Eugene V. Mosharov, Doron Betel, Viviane Tabar, Lorenz Studer
Nathaniel S. Chapman, Viktoriya Borisevich, Nurgun Kose, Luke Myers, Stephen Priest, Éric Bergeron, Elena Trigo Esteban, María Paz Sánchez-Seco, José Melero, Thomas W. Geisbert, Robert W. Cross, James E. Crowe Jr.Nathaniel S. Chapman, Viktoriya Borisevich, Nurgun Kose, Luke Myers, Stephen Priest, Éric Bergeron, Elena Trigo Esteban, María Paz Sánchez-Seco, José Melero, Thomas W. Geisbert, Robert W. Cross, James E. Crowe Jr.×Abstract
Crimean-Congo hemorrhagic fever virus (CCHFV) is an emerging arboviral and zoonotic bunyavirus. CCHFV can infect livestock, wild animals, and humans. Here, we report the isolation of a panel of mAbs from the B cells of an immune individual following a natural nosocomial infection. We determined that the panel comprised antibodies that bound to 2 glycoproteins: (a) the carboxy-terminal glycoprotein (Gc) that serves as the fusion protein and (b) the glycoprotein 38 (GP38). By antibody variable gene analysis, we identified genetic diversity in the B cell response to CCHFV within a single donor for both Gc- and GP38-specific responses. Protection against most bunyavirus-associated diseases is mediated principally by neutralizing antibodies, but here, we found that neutralization activity was not associated with protection. Gc-specific antibodies to diverse antigenic sites neutralized only weakly and did not protect against heterologous virus challenge. GP38-specific antibodies bound to 2 dominant antigenic sites on the glycoprotein. Although GP38-specific antibodies did not neutralize the virus, one mediated protection against heterologous virus challenge in an experimental model of infection in mice primarily by complement-mediated activity. These studies support the development of protective CCHFV countermeasures against GP38.
Authors
Nathaniel S. Chapman, Viktoriya Borisevich, Nurgun Kose, Luke Myers, Stephen Priest, Éric Bergeron, Elena Trigo Esteban, María Paz Sánchez-Seco, José Melero, Thomas W. Geisbert, Robert W. Cross, James E. Crowe Jr.
Zhebin Hua, Weimin Xu, Wenjun Ding, Zhuoyue Fu, Yaosheng Wang, Yiqing Yang, Fangyuan Liu, Zhujiang Dai, Wenbo Tang, Weijun Ou, Wensong Ge, YingWei Chen, Zhongchuan Wang, Chen-Ying Liu, Peng DuZhebin Hua, Weimin Xu, Wenjun Ding, Zhuoyue Fu, Yaosheng Wang, Yiqing Yang, Fangyuan Liu, Zhujiang Dai, Wenbo Tang, Weijun Ou, Wensong Ge, YingWei Chen, Zhongchuan Wang, Chen-Ying Liu, Peng Du×Abstract
The dynamic assembly and regulation of the IκB kinase (IKK) complex in the NF-κB pathway are central to the pathogenesis and progression of inflammatory bowel disease (IBD). We recently reported that the transcription factor hematopoietically expressed homeobox (HHEX) promotes colitis-associated colorectal cancer, but the potential role of HHEX in intestinal inflammation remains uncharacterized. Here, we found that HHEX is upregulated in inflamed colons in a colitis mouse model and in clinical IBD samples. HHEX overexpression increased inflammatory cytokine expression, and HHEX loss largely abrogated the inflammatory response in vitro and intestinal inflammation in vivo. Mechanistically, IKKα phosphorylates HHEX at S213 to stabilize HHEX in response to TNF-α by inhibiting the interaction of HHEX with the E3 ubiquitin ligase MID2 and subsequent K48-linked ubiquitination and protein degradation. Importantly, HHEX interacted with and stabilized the IKKα/IKKβ complex via its N-terminal domain, thereby activating the NF-κB pathway and establishing a positive feedback loop that exacerbates intestinal inflammation. Our study reveals a transcription-independent function of HHEX in promoting IKK complex assembly and colitis, identifying HHEX as an IBD susceptibility gene and a potential target for IBD treatment.
Authors
Zhebin Hua, Weimin Xu, Wenjun Ding, Zhuoyue Fu, Yaosheng Wang, Yiqing Yang, Fangyuan Liu, Zhujiang Dai, Wenbo Tang, Weijun Ou, Wensong Ge, YingWei Chen, Zhongchuan Wang, Chen-Ying Liu, Peng Du
Yang Wu, Erika Tavares, Binrun Liang, Wallace B. Wee, Vito Mennella, Han-Chao Feng, Jiaying Cao, Pui Yee Wong, Jiayi Zheng, Mu He, Kirk AJ Stephenson, Liran Hanan Hochma, Janice Min Li, Nan-Peng Chen, Sharon D. Dell, Elise Heon, Zhen LiuYang Wu, Erika Tavares, Binrun Liang, Wallace B. Wee, Vito Mennella, Han-Chao Feng, Jiaying Cao, Pui Yee Wong, Jiayi Zheng, Mu He, Kirk AJ Stephenson, Liran Hanan Hochma, Janice Min Li, Nan-Peng Chen, Sharon D. Dell, Elise Heon, Zhen Liu×Abstract
Cilia are cellular organelles that extrude from the surface of various cell types, serving either sensory or motile functions. Retinitis pigmentosa GTPase regulator (RPGR) variants affect both photoreceptor sensory cilia and airway motile cilia, leading to retinitis pigmentosa (RP) and primary ciliary dyskinesia (PCD), respectively. Not all patients develop PCD, and it remains unclear which RPGR variants predispose patients to PCD. Here, we leverage 2D organoids, super-resolution microscopy, and live-cell imaging to characterize the multiciliated cells (MCCs) from patients with different RPGR variants and CRISPR-modified RPGR KO MCCs. We demonstrate that MCCs with RPGR variants have reduced ciliation, shorter cilia, impaired cilia beat, or cilia beat incoordination, potentially resulting in compromised mucociliary clearance and lung diseases. Moreover, we show that RPGR regulates motile cilia through interfering with F-actin dynamics, evidenced by the undissolved F-actin meshwork in RPGR-deficient MCCs, and the defects can be ameliorated with either latrunculin A or Y27632 treatment. Though PCD was observed only in patients with variants that affect both isoforms, patients with RPGRORF15 variants also had cilia and airway anomalies. All RPGR variants affected motile cilia in some way, and the mechanisms involved the accumulation of apical F-actin.
Authors
Yang Wu, Erika Tavares, Binrun Liang, Wallace B. Wee, Vito Mennella, Han-Chao Feng, Jiaying Cao, Pui Yee Wong, Jiayi Zheng, Mu He, Kirk AJ Stephenson, Liran Hanan Hochma, Janice Min Li, Nan-Peng Chen, Sharon D. Dell, Elise Heon, Zhen Liu
Madeleine E. Harvey, Mingxin Shi, Yeongseok Oh, Taylor M. Page, Debra A. Mitchell, Addie Luo, Ov D. Slayden, James A. MacLean, Anjali Sharma, Kanako HayashiMadeleine E. Harvey, Mingxin Shi, Yeongseok Oh, Taylor M. Page, Debra A. Mitchell, Addie Luo, Ov D. Slayden, James A. MacLean, Anjali Sharma, Kanako Hayashi×Abstract
This study investigated how chronic pelvic pain (CPP) develops using rhesus macaques with naturally occurring endometriosis and a multiple lesion induction mouse model (MIM), as repeated retrograde menstruation is considered an underlying mechanism of endometriosis pathogenesis. MIM increased lesion numbers and elevated hypersensitivity. Elevated persistent glial cell activation was observed across multiple brain regions or spinal cords in MIM and rhesus macaques. Elevated TRPV1, SP, and CGRP expressions in the dorsal root ganglia (DRG) were persistent in MIM. MIM induced the severe disappearance of TIM4hiMHCIIlo residential macrophages and an influx of increased pro-inflammatory TIM4loMHCIIhi macrophages in the peritoneal cavity. Cytokine levels were persistently elevated in MIM. Furthermore, dienogest (a synthetic progestin) and fingolimod (a selective immunosuppressor) reduced hyperalgesia and neuroinflammation. Our results indicate that recurrent retrograde menstruation can be a peripheral stimulus that induces nociceptive pain and creates a composite chronic inflammatory stimulus, leading to neuroinflammation and sensitization of the central nervous system. The circuits of neuroplasticity and stimulation of peripheral organs via a feedback loop of neuroinflammation may mediate widespread endometriosis-associated CPP. These findings in mice were further supported by results from the spontaneously developed advanced endometriosis in rhesus macaques via recurrent retrograde menstruation.
Authors
Madeleine E. Harvey, Mingxin Shi, Yeongseok Oh, Taylor M. Page, Debra A. Mitchell, Addie Luo, Ov D. Slayden, James A. MacLean, Anjali Sharma, Kanako Hayashi
Pauline Morigny, Honglei Ji, Laura Cussonneau, Sabrina Zorzato, Yun Kwon, Fabien Riols, Doris Kaltenecker, Alisa Maier, Vignesh Karthikaisamy, Samantha Corrà, Tanja Krauss, Claudine Seeliger, Syed Qaaifah Gillani, Joël J. Tissink, Sandra Lacas-Gervais, Tuna Felix Samanci, Adriano Maida, Raul Terron-Exposito, Angela Trinca, Christine von Toerne, Leonardo Nogara, Melina Claussnitzer, Olga Prokopchuk, Jeannine Bachmann, Mauricio Berriel Diaz, Laure B. Bindels, Ondrej Kuda, Hans Hauner, Mark Haid, Stephan Herzig, Carlo Fiore Viscomi, Jerome Gilleron, Anja Zeigerer, Bert Blaauw, Maria RohmPauline Morigny, Honglei Ji, Laura Cussonneau, Sabrina Zorzato, Yun Kwon, Fabien Riols, Doris Kaltenecker, Alisa Maier, Vignesh Karthikaisamy, Samantha Corrà, Tanja Krauss, Claudine Seeliger, Syed Qaaifah Gillani, Joël J. Tissink, Sandra Lacas-Gervais, Tuna Felix Samanci, Adriano Maida, Raul Terron-Exposito, Angela Trinca, Christine von Toerne, Leonardo Nogara, Melina Claussnitzer, Olga Prokopchuk, Jeannine Bachmann, Mauricio Berriel Diaz, Laure B. Bindels, Ondrej Kuda, Hans Hauner, Mark Haid, Stephan Herzig, Carlo Fiore Viscomi, Jerome Gilleron, Anja Zeigerer, Bert Blaauw, Maria Rohm×Abstract
Cachexia is a metabolic wasting syndrome affecting many patients with cancer, with poor survival outcomes. Disturbed lipid metabolism is a hallmark of cachexia, and our previous work has identified increased levels of circulating ceramides, which are bioactive lipids with adverse effects in metabolic diseases, as biomarkers for cachexia in mouse models and patients. Here, we investigated the role of ceramides on cachexia development using the well-established C26 colon carcinoma model. We demonstrated that elevated ceramides in cachexia arose from increased liver synthesis. We showed that ceramides directly contributed to impaired mitochondrial function and energy homeostasis in cachexia target tissues. Targeting ceramide synthesis using miRNA interference, or myriocin, an approved compound targeting the key synthesis enzyme serine palmitoyltransferase (SPT), improved markers of muscle atrophy in cachectic male mice. Importantly, we demonstrated that key enzymes involved in ceramide production were also elevated in livers, but not in other organs, of patients with cancer cachexia, correlating with disease severity. Our data place ceramides as contributors to metabolic dysfunction in cachexia and highlight the suitability of the ceramide synthesis pathway for therapeutic targeting.
Authors
Pauline Morigny, Honglei Ji, Laura Cussonneau, Sabrina Zorzato, Yun Kwon, Fabien Riols, Doris Kaltenecker, Alisa Maier, Vignesh Karthikaisamy, Samantha Corrà, Tanja Krauss, Claudine Seeliger, Syed Qaaifah Gillani, Joël J. Tissink, Sandra Lacas-Gervais, Tuna Felix Samanci, Adriano Maida, Raul Terron-Exposito, Angela Trinca, Christine von Toerne, Leonardo Nogara, Melina Claussnitzer, Olga Prokopchuk, Jeannine Bachmann, Mauricio Berriel Diaz, Laure B. Bindels, Ondrej Kuda, Hans Hauner, Mark Haid, Stephan Herzig, Carlo Fiore Viscomi, Jerome Gilleron, Anja Zeigerer, Bert Blaauw, Maria Rohm
Kohsuke Isomoto, Koji Haratani, Takahiro Tsujikawa, Shuta Tomida, Yusuke Makutani, Masayuki Takeda, Kimio Yonesaka, Kaoru Tanaka, Tsutomu Iwasa, Kazuko Sakai, Kazuto Nishio, Akihiko Ito, Kazuhiko Nakagawa, Hidetoshi HayashiKohsuke Isomoto, Koji Haratani, Takahiro Tsujikawa, Shuta Tomida, Yusuke Makutani, Masayuki Takeda, Kimio Yonesaka, Kaoru Tanaka, Tsutomu Iwasa, Kazuko Sakai, Kazuto Nishio, Akihiko Ito, Kazuhiko Nakagawa, Hidetoshi Hayashi×Abstract
BACKGROUND Immune checkpoint inhibitors (ICIs) targeting the programmed cell death 1 axis have revolutionized metastatic non–small cell lung cancer (mNSCLC) treatment. However, disease progression remains a concern, and the role of the complex tumor microenvironment (TME) in treatment failure is not fully understood.METHODS In this biomarker study involving 103 patients with mNSCLC, including 81 patients who received ICI treatment, we evaluated the association between heterogeneous immune cell subsets and ICI efficacy through single-cell spatial profiling of pretreatment tumor tissue, using a 29-marker multiplex IHC platform built for in-depth dissection of the TME.RESULTS Among various types of intratumoral lymphocytes, including Th1, Treg, and NK cells, only CD8+ T cells (tumor-infiltrating lymphocytes [TILs]) were associated with ICI efficacy. Computational tissue segmentation underscored the importance of direct physical interactions between CD8+ TILs and cancer cells for ICI efficacy. TIL phenotyping identified CD39/CD103/Ki-67 positivity as a hallmark of exhausted yet functional tumor-reactive CD8+ TILs. Immunosuppressive tumor-associated macrophages (TAMs) and cancer-associated fibroblasts were independent unfavorable adversaries. High CD73 expression on cancer cells was suggested to confer tolerance to ICI in EGFR/ALK-oncogene+ NSCLC, potentially through M2-TAM accumulation and aberrant angiogenesis.CONCLUSION Our study delineates the clinical relevance of heterogeneous immune cell subsets in ICI-treated mNSCLC, aiding the development of targeted therapeutic strategies.FUNDING Osaka Cancer Society, KANAE Foundation for the Promotion of Medical Science, SGH Foundation, and YOKOYAMA Foundation for Clinical Pharmacology.
Authors
Kohsuke Isomoto, Koji Haratani, Takahiro Tsujikawa, Shuta Tomida, Yusuke Makutani, Masayuki Takeda, Kimio Yonesaka, Kaoru Tanaka, Tsutomu Iwasa, Kazuko Sakai, Kazuto Nishio, Akihiko Ito, Kazuhiko Nakagawa, Hidetoshi Hayashi
Yixin Wang, Hongpeng Huang, Feng Shao, Rachana Eshwaran, Miao Qin, Noor Karim, Yonggang Ren, Gergana Dobreva, Hans-Peter Hammes, Thomas Wieland, Yuxi FengYixin Wang, Hongpeng Huang, Feng Shao, Rachana Eshwaran, Miao Qin, Noor Karim, Yonggang Ren, Gergana Dobreva, Hans-Peter Hammes, Thomas Wieland, Yuxi Feng×Abstract
Diabetic retinopathy involves early retinal vascular barrier breakdown and pericyte loss, yet the initiating molecular events remain poorly defined. Vascular endothelial cadherin (VE-cadherin), a key regulator of endothelial integrity, is notably reduced in diabetic and prediabetic nucleoside diphosphate kinase B–deficient (NDPKB-deficient) mouse retinas, particularly in the retinal deep capillary layer, and this decline precedes pericyte loss. In vitro, high glucose (HG) and NDPKB deficiency induced VE-cadherin Y685 phosphorylation, promoting its junctional internalization, activating the hexosamine biosynthesis pathway, and increasing angiopoietin 2 (Ang2), resulting in impaired endothelial barrier function and disrupting pericyte attachment. Preventing Y685 phosphorylation through VE-cadherin Y685F mutation blocked these HG- and NDPKB-driven pathological effects. Pharmacological intervention experiments identified protein O-linked β-N-acetyl glucosamine (O-GlcNAc) modification as a mediator of Y685-dependent Ang2 upregulation. In vivo, VE-cadherin Y685F-knockin mice were protected from diabetes- and prediabetes-induced vascular hyperpermeability, exhibited reduced protein O-GlcNAcylation and Ang2 induction, and maintained neuronal function. O-GlcNAc–enriched retinal proteomics further showed that the Y685F mutation restored balanced neurovascular and mitochondrial pathways. These findings highlight the potential of targeting VE-cadherin Y685 phosphorylation as a promising therapeutic approach to maintain retinal vascular integrity and attenuate the pathological progression of diabetic and prediabetic retinopathy.
Authors
Yixin Wang, Hongpeng Huang, Feng Shao, Rachana Eshwaran, Miao Qin, Noor Karim, Yonggang Ren, Gergana Dobreva, Hans-Peter Hammes, Thomas Wieland, Yuxi Feng
Gaelle Haddad, Junyu Guo, Yin Xi, Emin Albayrak, Mahrukh Huseni, Habib Hamidi, Romain Banchereau, Edward Kadel, Sarita Dubey, Corey Carter, Payal Kapur, James Brugarolas, Ivan PedrosaGaelle Haddad, Junyu Guo, Yin Xi, Emin Albayrak, Mahrukh Huseni, Habib Hamidi, Romain Banchereau, Edward Kadel, Sarita Dubey, Corey Carter, Payal Kapur, James Brugarolas, Ivan Pedrosa×Abstract
BACKGROUND The relationship between molecular subgroups in clear-cell renal cell carcinoma (ccRCC) and metastatic tropism is poorly understood.METHODS We analyzed over 5,000 metastatic sites from 305 treatment-naive ccRCC patients in the IMmotion150 phase II clinical trial, where patients were randomized to atezolizumab, atezolizumab/bevacizumab, or sunitinib.RESULTS Angiogenic tumors (clusters 1 and 2) had a higher rate of pancreatic (21% vs. 6.9%; P = 0.002) and lower absolute number of lymph node (2.5 vs. 4.2; P = 0.006) metastases. In contrast, proliferative tumors (clusters 4 and 5) exhibited a higher absolute number of lymph node metastases (5.5 vs. 3.5; P = 0.019). Patients with pancreatic metastases receiving sunitinib had higher odds of overall response (OR, 7.13; 95% CI, 1.81–28.07; P = 0.0049) and longer progression-free survival than those without pancreatic metastases (P = 0.02).CONCLUSION ccRCC metastatic tropism relates to molecular clusters that predict response to therapy for tumors that metastasize to the pancreas.TRIAL REGISTRATION ClinicalTrials.gov NCT01984242FUNDING NIH grants R01CA154475 and P50CA196516.
Authors
Gaelle Haddad, Junyu Guo, Yin Xi, Emin Albayrak, Mahrukh Huseni, Habib Hamidi, Romain Banchereau, Edward Kadel, Sarita Dubey, Corey Carter, Payal Kapur, James Brugarolas, Ivan Pedrosa
×Abstract
Skraban-Deardorff syndrome, a rare neurodevelopmental disorder caused by WD repeat domain 26 (WDR26) haploinsufficiency, is characterized by intellectual disability, seizures, autistic-like behaviors, and craniofacial anomalies. Despite its genetic association with variants disrupting the C-terminal to LisH (CTLH) E3 ubiquitin ligase complex, the molecular mechanisms linking WDR26 dysfunction to neurodevelopmental deficits remain unclear. Here, we demonstrate that Wdr26 heterozygous-KO mice (Wdr26+/–) recapitulated core clinical features of the syndrome, including learning and memory impairments, social dysfunction, heightened seizure susceptibility, and motor deficits, alongside rare craniofacial and dental abnormalities. Mechanistically, Wdr26 haploinsufficiency stabilized RUNX1 translocation partner 1 (RUNX1T1), a transcriptional coactivator critical for neuronal differentiation, by impairing its ubiquitination and proteasomal degradation, consequently disrupting the level of microtubule-associated protein 2 (MAP2), a key regulator of dendritic architecture and synaptic plasticity. Early intervention in neonatal Wdr26+/– mice (P0.5) using AAV-shRNA–mediated Runx1t1 knockdown reversed MAP2 overexpression and behavioral deficits. Notably, the antipsychotic risperidone ameliorated cognitive and social impairments in Wdr26+/– mice by upregulating WDR26 levels, suggesting a potential therapeutic avenue. Our findings not only establish the animal model as a robust preclinical tool but also define the WDR26/RUNX1T1/MAP2 regulatory axis as pivotal to the syndrome’s pathogenesis, while identifying actionable therapeutic targets.
Authors
Xingyun Xu, Yaohui Zhou, Shiyao Xu, Hongjie Zhou, Xuexia Lin, Yuhao Luo, Yu Xu, Zhigang Miao, Wei Ge, Hao Yang, Xingshun Xu
×Abstract
Single-agent anti-PD-1 antibodies are ineffective for pancreatic ductal adenocarcinoma (PDAC) due to the immunosuppressive tumor-microenvironment (TME). KRAS mutations contribute to the inflammatory TME and therapeutic resistance by upregulating IL-8 via MAPK pathways. Thus, this study attempted to overcome the resistance to anti-PD-1 antibodies by targeting downstream KRAS-effectors. The study found that the resistance to anti-PD-1 antibodies can be overcome through MEK1/2-inhibition. The combination of anti-PD-1 antibodies and MEK inhibitors displayed antitumor activity in Kras mutated (Krasmut) KPC mouse tumors, but not WT (KrasWT) Panc02 tumors. The combination of anti-PD-1 antibodies and MEK inhibitors induced recruitment of tumor-associated neutrophils (TANs) via CXCR2, an IL-8 receptor, and increased memory CD8+ T cells and IFN-γ production in treatment-sensitive tumors. However, larger tumors still resisted the combination of anti-PD-1 antibody and MEK inhibitor, likely due to hypoxia/necrosis-induced NETosis and associated paucity of CD8+ T cells. The subsequent addition of anti-CXCR2 antibody overcame this resistance by blocking TAN-infiltration to hypoxic/necrotic areas. Consistently, a risk-score based on the NETosis-MAPK signaling interaction is significantly associated with poorer survival in human PDAC. This study thus provides a new venue for overcoming resistance to strategies targeting KRAS signaling.
Authors
Brian Herbst, Alex Blair, Yiming Li, Elizabeth M. Jaffee, Lei Zheng
Yanrong Zhu, Gang Li, Yilei Guo, Yue He, Wanyi Zhang, Lei Gao, Jing Zhang, Pengxiang Guo, Haochang Lin, Wenjie Zhang, Zhifeng Wei, Yufeng Xia, Yue DaiYanrong Zhu, Gang Li, Yilei Guo, Yue He, Wanyi Zhang, Lei Gao, Jing Zhang, Pengxiang Guo, Haochang Lin, Wenjie Zhang, Zhifeng Wei, Yufeng Xia, Yue Dai×Abstract
Understanding susceptibility factors of sepsis is crucial for early diagnosis and development of personalized treatment strategies. However, the genetic determinants for initiation and progression of sepsis remain unclear. Here, we showed that the expression levels of estrogen receptor β (ERβ) were significantly reduced in the peripheral blood of patients with sepsis and were negatively correlated with disease severity. The results from human samples and experimental animals demonstrated that ERβ deficiency enhanced the body’s susceptibility to sepsis by inducing macrophage pyroptosis, thereby impairing bacterial clearance. Mechanistically, ERβ deficiency enhanced fatty acid oxidation, increased acetyl-CoA levels, and promoted acetylation of stomatin-like protein 2 (Stoml2) at K221, leading to mitochondrial dysfunction and macrophage pyroptosis. Mutating the Stoml2 K221 site mitigated these effects and improved survival of septic mice. These findings suggest ERβ deficiency as a potential genetic factor in sepsis susceptibility.
Authors
Yanrong Zhu, Gang Li, Yilei Guo, Yue He, Wanyi Zhang, Lei Gao, Jing Zhang, Pengxiang Guo, Haochang Lin, Wenjie Zhang, Zhifeng Wei, Yufeng Xia, Yue Dai
×Abstract
Glioblastoma (GBM) is a highly aggressive brain tumor characterized by extensive crosstalk between glioblastoma stem cells (GSCs) and immunosuppressive microglia, with our previous work identifying CLOCK and TFPI2 as key regulators of this interaction. Here, we uncover a ‘symbiotic exclusivity’ pattern between CLOCK and TFPI2, showing that, despite mutually exclusive amplifications, they sustain symbiotic regulatory interactions in GBM. The CLOCK-BMAL1 complex transcriptionally upregulates TFPI2, while TFPI2-driven hypoxia inducible factor 1 α (HIF-1α) signaling activates nuclear factor k B (NF-kB) P65 to upregulate the CLOCK-BMAL1 complex, creating a positive feedback loop to promote stemness, immunosuppression, and tumor progression. Disrupting the CLOCK-TFPI2 interplay through dual inhibition of their downstream effectors reduces GSC stemness and immunosuppressive microglia, activates antitumor immunity, and synergizes with anti-PD1 therapy to achieve complete tumor regression in 50%–62.5% of tumor-bearing mice. This study uncovers a promising therapeutic strategy for a broader subset of patients with GBM with high expression of either CLOCK or TFPI2, and provides a framework for identifying ‘symbiotic exclusivity’ genes in cancer.
Authors
Fei Zhou, Lizhi Pang, Yang Liu, Fatima Khan, Peiwen Chen
Qun Lin, Jinpeng Luo, Zhuxi Duan, Jieer Luo, Wei Zhang, Yuan Xia, Yinduo Zeng, Xiaolin Fang, Jiahui Liang, Jiayi Chen, Qianchong Lin, Yilin Quan, Ruiyu Hu, Hongcai Liu, Qiang Liu, Jun Li, Chang GongQun Lin, Jinpeng Luo, Zhuxi Duan, Jieer Luo, Wei Zhang, Yuan Xia, Yinduo Zeng, Xiaolin Fang, Jiahui Liang, Jiayi Chen, Qianchong Lin, Yilin Quan, Ruiyu Hu, Hongcai Liu, Qiang Liu, Jun Li, Chang Gong×Abstract
Bone metastasis remains a major cause of morbidity in estrogen receptor–positive breast cancer, with RANKL inhibitor resistance emerging as a critical clinical challenge. Nearly 40% of patients develop progressive skeletal lesions despite denosumab therapy, highlighting an urgent need to identify resistance mechanisms and alternative therapeutic strategies. We identified a RANKL-independent osteoclast activation pathway mediated by the CRKL/circCCDC50/NFATc1 axis. Mechanistically, CRKL promoted EIF4A3-dependent circCCDC50 biogenesis, which was packaged into large oncosomes and transferred to osteoclast precursors. Nuclear circCCDC50 recruited CARM1 to epigenetically activate NFATc1 transcription, establishing a self-reinforcing loop that sustained osteolysis despite RANKL blockade. Pharmacological inhibition of CARM1 (TP-064) effectively suppressed osteoclastogenesis and bone metastasis in denosumab-resistant models. These findings revealed a targetable resistance mechanism and provided a clinically actionable strategy to overcome microenvironment-driven metastasis through dual targeting of tumor and bone niches.
Authors
Qun Lin, Jinpeng Luo, Zhuxi Duan, Jieer Luo, Wei Zhang, Yuan Xia, Yinduo Zeng, Xiaolin Fang, Jiahui Liang, Jiayi Chen, Qianchong Lin, Yilin Quan, Ruiyu Hu, Hongcai Liu, Qiang Liu, Jun Li, Chang Gong
×Abstract
Gemcitabine-based chemotherapy is the standard treatment regimen for advanced intrahepatic cholangiocarcinoma (iCCA), but the frequent presence of chemoresistance limits its efficacy. Here, we identified isocitrate dehydrogenase 1 (IDH1) as the crucial target that confers chemoresistance of iCCA to gemcitabine using a druggable CRISPR/Cas9 library. The positive association between IDH1 expression and chemoresistance was revealed in a gemcitabine-treated iCCA cohort and with cell-based drug sensitivity assays. Utilizing patient-derived organoids, cell line–derived xenografts, and patient-derived xenografts, we demonstrated that IDH1 knockdown or IDH1 pharmacological inhibition facilitated gemcitabine efficacy in these preclinical iCCA models carrying wild-type IDH1 (wtIDH1). Mechanistically, wtIDH1 oxidizes isocitrate to generate α-ketoglutarate and NNADPH, thereby creating a mechanism to manage the oxidative stress induced by gemcitabine, maintaining cellular redox homeostasis, and, ultimately, leading to chemoresistance to gemcitabine. Significantly, ivosidenib, the FDA-approved allosteric IDH1 inhibitor, demonstrated synergistic antitumor efficacy with gemcitabine in wtIDH1 preclinical iCCA models through boosting intracellular oxidative stress under physiological conditions. The low level of Mg2+, an ion that competitively hinders binding of ivosidenib on wtIDH1, in the iCCA tumor microenvironment contributed to the expanded therapeutic window for use of ivosidenib in patients with iCCA. Our work revealed the potency of combining targeting IDH1 and chemotherapy against wtIDH1 iCCA and other tumors.
Authors
Xiuxian Li, Zhixiao Song, Shusheng Lin, Man Luo, Shaoru Liu, Yang Liu, Fapeng Zhang, Leibo Xu, Chao Liu, Honghua Zhang
×Abstract
Epigenetic dysregulation is associated with immune evasion and immune checkpoint blockade (ICB) resistance. Here, using in vivo CRISPR/Cas9 screens targeting epigenetics-related factors in mouse tumor models treated with ICB, we identified chromobox 4 (CBX4) as a key negative regulator of the immune tumor microenvironment (TME). Single-cell RNA-seq and spatial transcriptomics analyses of patients receiving neoadjuvant anti–programmed cell death protein 1 (anti–PD-1) therapy revealed high CBX4 expression in both tumor cells and immunosuppressive tumor-associated macrophage subpopulations, with preferential accumulation in nonresponders. Deficiency of CBX4 in macrophages or tumor cells induced robust antitumor immunity and increased infiltration and the cytotoxic activity of CD8+ T cells and NK cells, thereby heightening the sensitivity of ICB treatment. Mechanistically, CBX4 targeted H3K9me3- and H3K27me3-marked endogenous retroelements such as RLTR4-Mm-int. Loss of CBX4 derepressed retrotransposons, activating cytosolic RNA-sensing pathways and triggering the type I IFN response, ultimately leading to a robustly inflamed TME. Moreover, we uncovered a negative correlation between CBX4 expression, immune responses, and retrotransposon levels, and were able to determine the prognosis of patients with hepatocellular carcinoma (HCC) undergoing ICB therapy. Our study establishes CBX4 as an epigenetic immune checkpoint through the epigenetic silencing of retrotransposons, remodeling the immune TME and thus providing a promising therapeutic target to enhance tumor immunogenicity and overcome immunotherapy resistance.
Authors
Zhibo Ma, Wenlong Jia, Xi Zhou, Jing Liu, Qingwen Li, Ruizhi Chang, Gu Shiqi, Naonao Yuan, Zhishui Chen, Peixiang Lan
×Abstract
VPS13A is an intracellular lipid transfer protein comprising more than 3,000 amino acids. Mutations in human VPS13A cause VPS13A disease, a neurodegenerative disorder that affects movement and cognition. VPS13A forms a complex with the membrane protein XK to mediate ATP-induced phospholipid scrambling in the plasma membrane. Here, we established a mouse cell system expressing full-length mouse VPS13A and examined its interaction with XK. Mutational analysis revealed that VPS13A binds to XK through a C-terminal β-strand that interacts with a β-hairpin in the central region of XK, an interaction essential for scramblase activity. The XK paralog XKR2, which contains a similar β-hairpin structure, also associates with VPS13A and supports phospholipid scrambling. We analyzed 10 mouse VPS13A variants corresponding to human patient mutations and classified them into 4 groups: (a) L67P, I90K, and W2453R, which showed reduced expression; (b) A1091P and M3080R, which were normally expressed but lacked scramblase activity; (c) S1446P, Q2689H, Y2713C, and R3084H, which modestly impaired expression or activity; and (d) I2763R, which altered cell size and disrupted ER independently of XK. These findings define the VPS13A–XK interaction interface, clarify the functional impact of disease-causing mutations, and reveal an unexpected gain-of-function mutation of a VPS13A variant.
Authors
Xing Lin, Yuta Ryoden, Chigure Suzuki, Hiroyuki Ishikawa, Takaharu Sakuragi, Yasuo Uchiyama, Shigekazu Nagata
Jun Fang, Jeremy M. Simon, Tao Wang, Yunpeng Gao, Xianju Bi, Lianxin Hu, Chengheng Liao, Cheng Zhang, Yayoi Adachi, Jin Zhou, Hongyi Liu, Qian Liang, James A. Nathan, Ram Mani, James Brugarolas, Qing ZhangJun Fang, Jeremy M. Simon, Tao Wang, Yunpeng Gao, Xianju Bi, Lianxin Hu, Chengheng Liao, Cheng Zhang, Yayoi Adachi, Jin Zhou, Hongyi Liu, Qian Liang, James A. Nathan, Ram Mani, James Brugarolas, Qing Zhang×Abstract
Resistance to HIF-2α inhibitors such as belzutifan underscores the need to better understand how HIF-2α is transcriptionally regulated in clear cell renal cell carcinoma (ccRCC). Here, we uncover a cytokine-driven enhancer mechanism that sustains HIF-2α expression through the JAK1/STAT3 signaling pathway. Using a genome-wide CRISPR screen in von Hippel–Lindau–deficient (VHL-deficient) ccRCC cells, we identified SOCS3 as a key negative regulator of HIF-2α. Mechanistically, loss of SOCS3 activates JAK1/STAT3 signaling, leading to the recruitment of STAT3 to distal enhancers upstream of endothelial PAS domain-containing protein (EPAS1) that physically loop to its promoter to drive HIF-2α transcription. This cytokine-enhancer circuit was recapitulated in samples from patients with ccRCC and functionally validated using CRISPR interference (CRISPRi), which disrupted enhancer-promoter looping and reduced tumor growth in HIF-2α–dependent models. SOCS3 overexpression or pharmacologic inhibition of JAK1/STAT3 markedly suppressed HIF-2α expression and tumor progression both in vitro and in vivo. Unlike prior studies focusing on VHL/HIF occupancy–driven enhancer activation, this work defines a trans-acting cytokine–JAK1/STAT3 pathway that transcriptionally controls EPAS1. Together, these findings reveal a targetable enhancer mechanism that sustains HIF-2α expression and suggest that combined inhibition of JAK1/STAT3 and HIF-2α may overcome therapeutic resistance in kidney cancer.
Authors
Jun Fang, Jeremy M. Simon, Tao Wang, Yunpeng Gao, Xianju Bi, Lianxin Hu, Chengheng Liao, Cheng Zhang, Yayoi Adachi, Jin Zhou, Hongyi Liu, Qian Liang, James A. Nathan, Ram Mani, James Brugarolas, Qing Zhang



Copyright © 2026 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)