Issue published April 1, 2019 Previous issue | Next issue

- Volume 129, Issue 4
Go to section:
On the cover: miR-30c represses fibrin-mediated tumor angiogenesis
To promote their growth, cancer cells misappropriate angiogenic signals, including endothelial cell–expressed Serpine1, which encodes the plasminogen activator inhibitor PAI-1. The inhibition of plasmin leads to persistent perivascular fibrin deposition and growth factor sequestration in the tumor microenvironment. In this issue of the JCI, McCann et al. reveal an essential role for miR-30c in controlling fibrin-mediated tumor angiogenesis. They discovered that TGF-β–driven reduction in miR-30c enhances PAI-1 expression and perivascular fibrin deposition in endothelial cells that support angiogenesis. They further demonstrate that miR-30c mimics decrease whereas miR-30c antagomiRs increase fibrin-mediated endothelial sprouting and tumor growth. The cover image shows endothelial cell sprouting in a fibrin matrix. Image credit: James McCann.
-
Viewpoint
×
Abstract
The American Society for Clinical Investigation (ASCI), a nonprofit honorary society, was established to support physician-scientists by serving as a benchmark of excellence in medical research, a forum to celebrate advances in medicine, and a vehicle to communicate advances that bridge basic and translational research and their implementation across the growing myriad of medical specialties. A core intention of the Society is to engage the medical research community broadly through transparent communications of our activities and initiatives with the institutions that comprise the base for our membership. Recognizing the importance in identifying and actuating a strategy to support the Society’s broad mission, the current leadership has undertaken a strategic plan that initiates with the goal of revamping its Institutional Representatives program. While the Society has grown with the historical privilege of close connections to institutions through an informal web created largely by the elected membership, we aim to improve institutional engagement towards overall goals of embracing and enhancing diversity of our community and implementing future collaborative programs to support physician-scientists. We briefly review ASCI’s history, mission, and structure, and present the blueprint of the new Institutional Representatives program.
Authors
Kieren A. Marr, W. Kimryn Rathmell, John B. Hawley, Karen D. Guth
-
Review Series
×
Abstract
Gastrointestinal (GI) allergic disease is an umbrella term used to describe a variety of adverse, food antigen–driven, immune-mediated diseases. Although these diseases vary mechanistically, common elements include a breakdown of immunologic tolerance, a biased type 2 immune response, and an impaired mucosal barrier. These pathways are influenced by diverse factors such as diet, infections, exposure to antibiotics and chemicals, GI microbiome composition, and genetic and epigenetic elements. Early childhood has emerged as a critical period when these factors have a dramatic impact on shaping the immune system and therefore triggering or protecting against the onset of GI allergic diseases. In this Review, we will discuss the latest findings on the molecular and cellular mechanisms that govern GI allergic diseases and how these findings have set the stage for emerging preventative and treatment strategies.
Authors
Nurit P. Azouz, Marc E. Rothenberg
×Abstract
Allergen-specific immunotherapy has shown promise for the treatment of food allergy and is currently being evaluated in clinical trials. Although immunotherapy can induce desensitization, the mechanisms underlying this process are not completely understood. Recent advances in high-throughput technologies along with concomitant advances in data analytics have enabled monitoring of cells at the single-cell level and increased the research focus on upstream cellular factors involved in the efficacy of immunotherapy, particularly the role of T cells. As our appreciation of different T cell subsets and their plasticity increases, the initial simplistic view that restoring Th1/Th2 balance by decreasing Th2 or increasing Th1 responses can ameliorate food allergy is being enhanced by a more complex model involving other T cell subsets, particularly Tregs. In this Review, we focus on the current understanding of T cell functions in food allergy, tolerance, and immunotherapy.
Authors
Vanitha Sampath, Kari C. Nadeau
×Abstract
The epithelial cell–derived cytokines thymic stromal lymphopoietin (TSLP), IL-33, and IL-25 are central regulators of type 2 immunity, which drives a broad array of allergic responses. Often characterized as “alarmins” that are released by the barrier epithelium in response to external insults, these epithelial cell–derived cytokines were initially thought to act only early in allergic inflammation. Indeed, TSLP can condition dendritic cells to initiate type 2 responses, and IL-33 may influence susceptibility to asthma through its role in establishing the immune environment in the perinatal lungs. However, TSLP, IL-33, and IL-25 all regulate a broad spectrum of innate immune cell populations and are particularly potent in eliciting and activating type 2 innate lymphoid cells (ILC2s) that may act throughout allergic inflammation. Recent data suggest that a TSLP/ILC axis may mediate steroid resistance in asthma. Recent identification of memory Th2 cell subsets that are characterized by high receptor expression for TSLP, IL-33, and IL-25 further supports a role for these cytokines in allergic exacerbations. There is therefore growing interest in developing biologics that target TSLP, IL-33, and IL-25. This Review provides an overview of TSLP, IL-33, and IL-25 and the development of blocking antibodies that target these epithelial cell–derived cytokines.
Authors
Florence Roan, Kazushige Obata-Ninomiya, Steven F. Ziegler
×Abstract
The rising prevalence of allergies represents an increasing socioeconomic burden. A detailed understanding of the immunological mechanisms that underlie the development of allergic disease, as well as the processes that drive immune tolerance to allergens, will be instrumental in designing therapeutic strategies to treat and prevent allergic disease. Improved characterization of individual patients through the use of specific biomarkers and improved definitions of disease endotypes are paving the way for the use of targeted therapeutic approaches for personalized treatment. Allergen-specific immunotherapy and biologic therapies that target key molecules driving the Th2 response are already used in the clinic, and a wave of novel drug candidates are under development. In-depth analysis of the cells and tissues of patients treated with such targeted interventions provides a wealth of information on the mechanisms that drive allergies and tolerance to allergens. Here, we aim to deliver an overview of the current state of specific inhibitors used in the treatment of allergy, with a particular focus on asthma and atopic dermatitis, and provide insights into the roles of these molecules in immunological mechanisms of allergic disease.
Authors
Willem van de Veen, Mübeccel Akdis
×Abstract
Allergic diseases have in common a dysfunctional epithelial barrier, which allows the penetration of allergens and microbes, leading to the release of type 2 cytokines that drive allergic inflammation. The accessibility of skin, compared with lung or gastrointestinal tissue, has facilitated detailed investigations into mechanisms underlying epithelial barrier dysfunction in atopic dermatitis (AD). This Review describes the formation of the skin barrier and analyzes the link between altered skin barrier formation and the pathogenesis of AD. The keratinocyte differentiation process is under tight regulation. During epidermal differentiation, keratinocytes sequentially switch gene expression programs, resulting in terminal differentiation and the formation of a mature stratum corneum, which is essential for the skin to prevent allergen or microbial invasion. Abnormalities in keratinocyte differentiation in AD skin result in hyperproliferation of the basal layer of epidermis, inhibition of markers of terminal differentiation, and barrier lipid abnormalities, compromising skin barrier and antimicrobial function. There is also compelling evidence for epithelial dysregulation in asthma, food allergy, eosinophilic esophagitis, and allergic rhinosinusitis. This Review examines current epithelial barrier repair strategies as an approach for allergy prevention or intervention.
Authors
Elena Goleva, Evgeny Berdyshev, Donald Y.M. Leung
×Abstract
The neuronal and immune systems exhibit bidirectional interactions that play a critical role in tissue homeostasis, infection, and inflammation. Neuron-derived neuropeptides and neurotransmitters regulate immune cell functions, whereas inflammatory mediators produced by immune cells enhance neuronal activation. In recent years, accumulating evidence suggests that peripheral neurons and immune cells are colocalized and affect each other in local tissues. A variety of cytokines, inflammatory mediators, neuropeptides, and neurotransmitters appear to facilitate this crosstalk and positive-feedback loops between multiple types of immune cells and the central, peripheral, sympathetic, parasympathetic, and enteric nervous systems. In this Review, we discuss these recent findings regarding neuro-immune crosstalk that are uncovering molecular mechanisms that regulate inflammation. Finally, neuro-immune crosstalk has a key role in the pathophysiology of allergic diseases, and we present evidence indicating that neuro-immune interactions regulate asthma pathophysiology through both direct and indirect mechanisms.
Authors
Hiroki Kabata, David Artis
×Abstract
In industrialized societies the incidence of allergic diseases like atopic dermatitis, food allergies, and asthma has risen alarmingly over the last few decades. This increase has been attributed, in part, to lifestyle changes that alter the composition and function of the microbes that colonize the skin and mucosal surfaces. Strategies that reverse these changes to establish and maintain a healthy microbiome show promise for the prevention and treatment of allergic disease. In this Review, we will discuss evidence from preclinical and clinical studies that gives insights into how the microbiota of skin, intestinal tract, and airways influence immune responses in the context of allergic sensitization.
Authors
Andrea M. Kemter, Cathryn R. Nagler
×Abstract
A rapidly developing paradigm for modern health care is a proactive and individualized response to patients’ symptoms, combining precision diagnosis and personalized treatment. Precision medicine is becoming an overarching medical discipline that will require a better understanding of biomarkers, phenotypes, endotypes, genotypes, regiotypes, and theratypes of diseases. The 100-year-old personalized allergen-specific management of allergic diseases has particularly contributed to early awareness in precision medicine. Polyomics, big data, and systems biology have demonstrated a profound complexity and dynamic variability in allergic disease between individuals, as well as between regions. Escalating health care costs together with questionable efficacy of the current management of allergic diseases facilitated the emergence of the endotype-driven approach. We describe here a precision medicine approach that stratifies patients based on disease mechanisms to optimize management of allergic diseases.
Authors
Ioana Agache, Cezmi A. Akdis
×Abstract
Environmental exposures interplay with human host factors to promote the development and progression of allergic diseases. The worldwide prevalence of allergic disease is rising as a result of complex gene-environment interactions that shape the immune system and host response. Research shows an association between the rise of allergic diseases and increasingly modern Westernized lifestyles, which are characterized by increased urbanization, time spent indoors, and antibiotic usage. These environmental changes result in increased exposure to air and traffic pollution, fungi, infectious agents, tobacco smoke, and other early-life and lifelong risk factors for the development and exacerbation of asthma and allergic diseases. It is increasingly recognized that the timing, load, and route of allergen exposure affect allergic disease phenotypes and development. Still, our ability to prevent allergic diseases is hindered by gaps in understanding of the underlying mechanisms and interaction of environmental, viral, and allergen exposures with immune pathways that impact disease development. This Review highlights epidemiologic and mechanistic evidence linking environmental exposures to the development and exacerbation of allergic airway responses.
Authors
Liza Bronner Murrison, Eric B. Brandt, Jocelyn Biagini Myers, Gurjit K. Khurana Hershey
-
Review
×
Abstract
Oncolytic virotherapy (OVT) is a promising approach in which WT or engineered viruses selectively replicate and destroy tumor cells while sparing normal ones. In the last two decades, different oncolytic viruses (OVs) have been modified and tested in a number of preclinical studies, some of which have led to clinical trials in cancer patients. These clinical trials have revealed several critical limitations with regard to viral delivery, spread, resistance, and antiviral immunity. Here, we focus on promising research strategies that have been developed to overcome the aforementioned obstacles. Such strategies include engineering OVs to target a broad spectrum of tumor cells while evading the immune system, developing unique delivery mechanisms, combining other immunotherapeutic agents with OVT, and using clinically translatable mouse tumor models to potentially translate OVT more readily into clinical settings.
Authors
Jordi Martinez-Quintanilla, Ivan Seah, Melissa Chua, Khalid Shah
-
Commentaries
×
Abstract
The identification of JAK2 mutations as disease-initiating in myeloproliferative neoplasms (MPNs) has led to new and effective therapies for these diseases. In a study published in this issue of the JCI, Stivala et al. explored the key observation that JAK inhibition successfully suppresses MAPK activation in MPN cell lines and primary MPN cells in vitro, and the finding that it failed to completely and effectively suppress MAPK activation in vivo in two mouse models. The authors went on to show that dual inhibition of JAK and the MAP kinase pathway provided enhanced therapeutic efficacy in the in vivo models of MPN.
Authors
David A. Williams
×Abstract
Genetically engineered T cells have shown promising activity in the treatment of cancer. However, these cells are also potentially susceptible to immune-suppressive pathways in the tumor microenvironment that may limit their efficacy. In this issue of the JCI, Yamamoto et al. describe a new cellular engineering approach to prevent Fas-mediated inhibition of T cell function, which may be exploited to improve cellular therapy for cancer.
Authors
Madhav V. Dhodapkar
×Abstract
Chronic unresolved inflammation contributes to the development of nonalcoholic steatohepatitis (NASH), a disorder characterized by lipotoxicity, fibrosis, and progressive liver dysfunction. In this issue of the JCI, Han et al. report that maresin 1 (MaR1), a proresolving lipid mediator, mitigates NASH by reprograming macrophages to an antiinflammatory phenotype. Mechanistically, they identified retinoic acid–related orphan receptor α (RORα) as both a target and autocrine regulator of MaR1 production. Because NASH is associated with many widely occurring metabolic diseases, including obesity and type 2 diabetes, identification of this endogenous protective pathway could have broad therapeutic implications.
Authors
Matthew Spite
×Abstract
Survivors of sepsis and other forms of critical illness frequently experience significant and disabling cognitive and affective disorders. Inflammation, ischemia, and glial cell dysfunction contribute to this persistent brain injury. In this issue of the JCI, Hippensteel et al. show that endothelial injury in animal models of sepsis or endotoxemia leads to shedding of heparan fragments from the endothelial glycocalyx. These fragments directly sequester brain-derived neurotrophic factor and impair hippocampal long-term potentiation, an electrophysiologic correlate of memory. The authors further explore the specific characteristics of heparan fragments that bind neurotrophins and the presence of these fragments in the circulation of patients who survive sepsis. This study highlights an important mechanism by which vascular injury can impair brain function.
Authors
Benjamin H. Singer
×Abstract
In this issue of the JCI, Casas et al. define a previously unknown role of the NADPH oxidase catalytic subunit NOX5 in cerebral infarction. Using a mouse expressing human NOX5 in the endothelium, the investigators show that NOX5 is activated and plays a deleterious role in promoting edema, infarction, and ultimately, worsened neurological function following cerebral ischemia. They provide evidence that this is due to the breakdown of the blood-brain barrier (BBB) and that a unique pharmacological inhibitor of NOX5, ML090, if given early, around the time of reoxygenation, can maintain BBB integrity. Future studies of NOX5 inhibition in humans, particularly in the setting of thrombolysis, are warranted.
Authors
Luciana Simão do Carmo, Bradford C. Berk, David G. Harrison
×Abstract
Motoneurons are particularly sensitive to mutations in mitofusin-2 (MFN2) that cause the neurological disorder Charcot-Marie-Tooth disease type 2A (CMT2A). MFN2 is a mitochondrial outer membrane protein that, together with its homologue MFN1, fuses mitochondria in most tissues. In this issue of the JCI, Zhou and colleagues show that increasing MFN1 expression in neurons can curtail neurological defects in a CMT2A mouse model. These results show that the ratio of MFN1 to MFN2 can explain the tissue specificity of CMT2A and indicate that augmentation of MFN1 in the nervous system has potential as a possible therapeutic strategy for CMT2A.
Authors
Keiko Iwata, Luca Scorrano
-
Research Articles
María Isabel Cuartero, Juan de la Parra, Alberto Pérez-Ruiz, Isabel Bravo-Ferrer, Violeta Durán-Laforet, Alicia García-Culebras, Juan Manuel García-Segura, Jagroop Dhaliwal, Paul W. Frankland, Ignacio Lizasoain, María Ángeles MoroMaría Isabel Cuartero, Juan de la Parra, Alberto Pérez-Ruiz, Isabel Bravo-Ferrer, Violeta Durán-Laforet, Alicia García-Culebras, Juan Manuel García-Segura, Jagroop Dhaliwal, Paul W. Frankland, Ignacio Lizasoain, María Ángeles Moro×
Abstract
Poststroke cognitive impairment is considered one of the main complications during the chronic phase of ischemic stroke. In the adult brain, the hippocampus regulates both encoding and retrieval of new information through adult neurogenesis. Nevertheless, the lack of predictive models and studies based on the forgetting processes hinders the understanding of memory alterations after stroke. Our aim was to explore whether poststroke neurogenesis participates in the development of long-term memory impairment. Here, we show a hippocampal neurogenesis burst that persisted 1 month after stroke and that correlated with an impaired contextual and spatial memory performance. Furthermore, we demonstrate that the enhancement of hippocampal neurogenesis after stroke by physical activity or memantine treatment weakened existing memories. More importantly, stroke-induced newborn neurons promoted an aberrant hippocampal circuitry remodeling with differential features at ipsi- and contralesional levels. Strikingly, inhibition of stroke-induced hippocampal neurogenesis by temozolomide treatment or using a genetic approach (Nestin-CreERT2/NSE-DTA mice) impeded the forgetting of old memories. These results suggest that hippocampal neurogenesis modulation could be considered as a potential approach for treatment of poststroke cognitive impairment.
Authors
María Isabel Cuartero, Juan de la Parra, Alberto Pérez-Ruiz, Isabel Bravo-Ferrer, Violeta Durán-Laforet, Alicia García-Culebras, Juan Manuel García-Segura, Jagroop Dhaliwal, Paul W. Frankland, Ignacio Lizasoain, María Ángeles Moro
Tori N. Yamamoto, Ping-Hsien Lee, Suman K. Vodnala, Devikala Gurusamy, Rigel J. Kishton, Zhiya Yu, Arash Eidizadeh, Robert Eil, Jessica Fioravanti, Luca Gattinoni, James N. Kochenderfer, Terry J. Fry, Bulent Arman Aksoy, Jeffrey E. Hammerbacher, Anthony C. Cruz, Richard M. Siegel, Nicholas P. Restifo, Christopher A. KlebanoffTori N. Yamamoto, Ping-Hsien Lee, Suman K. Vodnala, Devikala Gurusamy, Rigel J. Kishton, Zhiya Yu, Arash Eidizadeh, Robert Eil, Jessica Fioravanti, Luca Gattinoni, James N. Kochenderfer, Terry J. Fry, Bulent Arman Aksoy, Jeffrey E. Hammerbacher, Anthony C. Cruz, Richard M. Siegel, Nicholas P. Restifo, Christopher A. Klebanoff×Abstract
Across clinical trials, T cell expansion and persistence following adoptive cell transfer (ACT) have correlated with superior patient outcomes. Herein, we undertook a pan-cancer analysis to identify actionable ligand-receptor pairs capable of compromising T cell durability following ACT. We discovered that FASLG, the gene encoding the apoptosis-inducing ligand FasL, is overexpressed within the majority of human tumor microenvironments (TMEs). Further, we uncovered that Fas, the receptor for FasL, is highly expressed on patient-derived T cells used for clinical ACT. We hypothesized that a cognate Fas-FasL interaction within the TME might limit both T cell persistence and antitumor efficacy. We discovered that genetic engineering of Fas variants impaired in the ability to bind FADD functioned as dominant negative receptors (DNRs), preventing FasL-induced apoptosis in Fas-competent T cells. T cells coengineered with a Fas DNR and either a T cell receptor or chimeric antigen receptor exhibited enhanced persistence following ACT, resulting in superior antitumor efficacy against established solid and hematologic cancers. Despite increased longevity, Fas DNR–engineered T cells did not undergo aberrant expansion or mediate autoimmunity. Thus, T cell–intrinsic disruption of Fas signaling through genetic engineering represents a potentially universal strategy to enhance ACT efficacy across a broad range of human malignancies.
Authors
Tori N. Yamamoto, Ping-Hsien Lee, Suman K. Vodnala, Devikala Gurusamy, Rigel J. Kishton, Zhiya Yu, Arash Eidizadeh, Robert Eil, Jessica Fioravanti, Luca Gattinoni, James N. Kochenderfer, Terry J. Fry, Bulent Arman Aksoy, Jeffrey E. Hammerbacher, Anthony C. Cruz, Richard M. Siegel, Nicholas P. Restifo, Christopher A. Klebanoff
Stefania Crippa, Valeria Rossella, Annamaria Aprile, Laura Silvestri, Silvia Rivis, Samantha Scaramuzza, Stefania Pirroni, Maria Antonietta Avanzini, Luca Basso-Ricci, Raisa Jofra Hernandez, Marco Zecca, Sarah Marktel, Fabio Ciceri, Alessandro Aiuti, Giuliana Ferrari, Maria Ester BernardoStefania Crippa, Valeria Rossella, Annamaria Aprile, Laura Silvestri, Silvia Rivis, Samantha Scaramuzza, Stefania Pirroni, Maria Antonietta Avanzini, Luca Basso-Ricci, Raisa Jofra Hernandez, Marco Zecca, Sarah Marktel, Fabio Ciceri, Alessandro Aiuti, Giuliana Ferrari, Maria Ester Bernardo×Abstract
BACKGROUND. The human bone marrow (BM) niche contains a population of mesenchymal stromal cells (MSCs) that provide physical support and regulate hematopoietic stem cell (HSC) homeostasis. β-Thalassemia (BT) is a hereditary disorder characterized by altered hemoglobin beta-chain synthesis amenable to allogeneic HSC transplantation and HSC gene therapy. Iron overload (IO) is a common complication in BT patients affecting several organs. However, data on the BM stromal compartment are scarce. METHODS. MSCs were isolated and characterized from BM aspirates of healthy donors (HDs) and BT patients. The state of IO was assessed and correlated with the presence of primitive MSCs in vitro and in vivo. Hematopoietic supportive capacity of MSCs was evaluated by transwell migration assay and 2D coculture of MSCs with human CD34+ HSCs. In vivo, the ability of MSCs to facilitate HSC engraftment was tested in a xenogenic transplant model, whereas the capacity to sustain human hematopoiesis was evaluated in humanized ossicle models. RESULTS. We report that, despite iron chelation, BT BM contains high levels of iron and ferritin, indicative of iron accumulation in the BM niche. We found a pauperization of the most primitive MSC pool caused by increased ROS production in vitro which impaired MSC stemness properties. We confirmed a reduced frequency of primitive MSCs in vivo in BT patients. We also discovered a weakened antioxidative response and diminished expression of BM niche–associated genes in BT-MSCs. This caused a functional impairment in MSC hematopoietic supportive capacity in vitro and in cotransplantation models. In addition, BT-MSCs failed to form a proper BM niche in humanized ossicle models. CONCLUSION. Our results suggest an impairment in the mesenchymal compartment of BT BM niche and highlight the need for novel strategies to target the niche to reduce IO and oxidative stress before transplantation. FUNDING. This work was supported by the SR-TIGET Core grant from Fondazione Telethon and by Ricerca Corrente.
Authors
Stefania Crippa, Valeria Rossella, Annamaria Aprile, Laura Silvestri, Silvia Rivis, Samantha Scaramuzza, Stefania Pirroni, Maria Antonietta Avanzini, Luca Basso-Ricci, Raisa Jofra Hernandez, Marco Zecca, Sarah Marktel, Fabio Ciceri, Alessandro Aiuti, Giuliana Ferrari, Maria Ester Bernardo
Silvia Pozzi, Sai Sampath Thammisetty, Philippe Codron, Reza Rahimian, Karine Valérie Plourde, Geneviève Soucy, Christine Bareil, Daniel Phaneuf, Jasna Kriz, Claude Gravel, Jean-Pierre JulienSilvia Pozzi, Sai Sampath Thammisetty, Philippe Codron, Reza Rahimian, Karine Valérie Plourde, Geneviève Soucy, Christine Bareil, Daniel Phaneuf, Jasna Kriz, Claude Gravel, Jean-Pierre Julien×Abstract
The cytoplasmic aggregation of TAR DNA-binding protein-43 (TDP-43) is a hallmark of degenerating neurons in amyotrophic lateral sclerosis (ALS) and subsets of frontotemporal dementia (FTD). In order to reduce TDP-43 pathology, we generated single-chain (scFv) antibodies against the RNA recognition motif 1 (RRM1) of TDP-43, which is involved in abnormal protein self-aggregation and interaction with p65 NF-κB. Virus-mediated delivery into the nervous system of a scFv antibody, named VH7Vk9, reduced microgliosis in a mouse model of acute neuroinflammation and mitigated cognitive impairment, motor defects, TDP-43 proteinopathy, and neuroinflammation in transgenic mice expressing ALS-linked TDP-43 mutations. These results suggest that antibodies targeting the RRM1 domain of TDP-43 might provide new therapeutic avenues for the treatment of ALS and FTD.
Authors
Silvia Pozzi, Sai Sampath Thammisetty, Philippe Codron, Reza Rahimian, Karine Valérie Plourde, Geneviève Soucy, Christine Bareil, Daniel Phaneuf, Jasna Kriz, Claude Gravel, Jean-Pierre Julien
Simona Stivala, Tamara Codilupi, Sime Brkic, Anne Baerenwaldt, Nilabh Ghosh, Hui Hao-Shen, Stephan Dirnhofer, Matthias S. Dettmer, Cedric Simillion, Beat A. Kaufmann, Sophia Chiu, Matthew Keller, Maria Kleppe, Morgane Hilpert, Andreas S. Buser, Jakob R. Passweg, Thomas Radimerski, Radek C. Skoda, Ross L. Levine, Sara C. MeyerSimona Stivala, Tamara Codilupi, Sime Brkic, Anne Baerenwaldt, Nilabh Ghosh, Hui Hao-Shen, Stephan Dirnhofer, Matthias S. Dettmer, Cedric Simillion, Beat A. Kaufmann, Sophia Chiu, Matthew Keller, Maria Kleppe, Morgane Hilpert, Andreas S. Buser, Jakob R. Passweg, Thomas Radimerski, Radek C. Skoda, Ross L. Levine, Sara C. Meyer×Abstract
Constitutive JAK2 signaling is central to myeloproliferative neoplasm (MPN) pathogenesis and results in activation of STAT, PI3K/AKT, and MEK/ERK signaling. However, the therapeutic efficacy of current JAK2 inhibitors is limited. We investigated the role of MEK/ERK signaling in MPN cell survival in the setting of JAK inhibition. Type I and II JAK2 inhibition suppressed MEK/ERK activation in MPN cell lines in vitro, but not in Jak2V617F and MPLW515L mouse models in vivo. JAK2 inhibition ex vivo inhibited MEK/ERK signaling, suggesting that cell-extrinsic factors maintain ERK activation in vivo. We identified PDGFRα as an activated kinase that remains activated upon JAK2 inhibition in vivo, and PDGF-AA/PDGF-BB production persisted in the setting of JAK inhibition. PDGF-BB maintained ERK activation in the presence of ruxolitinib, consistent with its function as a ligand-induced bypass for ERK activation. Combined JAK/MEK inhibition suppressed MEK/ERK activation in Jak2V617F and MPLW515L mice with increased efficacy and reversal of fibrosis to an extent not seen with JAK inhibitors. This demonstrates that compensatory ERK activation limits the efficacy of JAK2 inhibition and dual JAK/MEK inhibition provides an opportunity for improved therapeutic efficacy in MPNs and in other malignancies driven by aberrant JAK-STAT signaling.
Authors
Simona Stivala, Tamara Codilupi, Sime Brkic, Anne Baerenwaldt, Nilabh Ghosh, Hui Hao-Shen, Stephan Dirnhofer, Matthias S. Dettmer, Cedric Simillion, Beat A. Kaufmann, Sophia Chiu, Matthew Keller, Maria Kleppe, Morgane Hilpert, Andreas S. Buser, Jakob R. Passweg, Thomas Radimerski, Radek C. Skoda, Ross L. Levine, Sara C. Meyer
Niraj Shenoy, Tushar D. Bhagat, John Cheville, Christine Lohse, Sanchari Bhattacharyya, Alexander Tischer, Venkata Machha, Shanisha Gordon-Mitchell, Gaurav Choudhary, Li-Fan Wong, LouAnn Gross, Emily Ressigue, Bradley Leibovich, Stephen A. Boorjian, Ulrich Steidl, Xiaosheng Wu, Kith Pradhan, Benjamin Gartrell, Beamon Agarwal, Lance Pagliaro, Masako Suzuki, John M. Greally, Dinesh Rakheja, R. Houston Thompson, Katalin Susztak, Thomas Witzig, Yiyu Zou, Amit VermaNiraj Shenoy, Tushar D. Bhagat, John Cheville, Christine Lohse, Sanchari Bhattacharyya, Alexander Tischer, Venkata Machha, Shanisha Gordon-Mitchell, Gaurav Choudhary, Li-Fan Wong, LouAnn Gross, Emily Ressigue, Bradley Leibovich, Stephen A. Boorjian, Ulrich Steidl, Xiaosheng Wu, Kith Pradhan, Benjamin Gartrell, Beamon Agarwal, Lance Pagliaro, Masako Suzuki, John M. Greally, Dinesh Rakheja, R. Houston Thompson, Katalin Susztak, Thomas Witzig, Yiyu Zou, Amit Verma×Abstract
Although clear cell renal cell carcinoma (ccRCC) has been shown to result in widespread aberrant cytosine methylation and loss of 5-hydroxymethylcytosine (5hmC), the prognostic impact and therapeutic targeting of this epigenetic aberrancy has not been fully explored. Analysis of 576 primary ccRCC samples demonstrated that loss of 5hmC was strongly associated with aggressive clinicopathologic features and was an independent adverse prognostic factor. Loss of 5hmC also predicted reduced progression-free survival after resection of nonmetastatic disease. The loss of 5hmC in ccRCC was not due to mutational or transcriptional inactivation of ten eleven translocation (TET) enzymes, but to their functional inactivation by l-2-hydroxyglutarate (L2HG), which was overexpressed due to the deletion and underexpression of L2HG dehydrogenase (L2HGDH). Ascorbic acid (AA) reduced methylation and restored genome-wide 5hmC levels via TET activation. Fluorescence quenching of the recombinant TET-2 protein was unaffected by L2HG in the presence of AA. Pharmacologic AA treatment led to reduced growth of ccRCC in vitro and reduced tumor growth in vivo, with increased intratumoral 5hmC. These data demonstrate that reduced 5hmC is associated with reduced survival in ccRCC and provide a preclinical rationale for exploring the therapeutic potential of high-dose AA in ccRCC.
Authors
Niraj Shenoy, Tushar D. Bhagat, John Cheville, Christine Lohse, Sanchari Bhattacharyya, Alexander Tischer, Venkata Machha, Shanisha Gordon-Mitchell, Gaurav Choudhary, Li-Fan Wong, LouAnn Gross, Emily Ressigue, Bradley Leibovich, Stephen A. Boorjian, Ulrich Steidl, Xiaosheng Wu, Kith Pradhan, Benjamin Gartrell, Beamon Agarwal, Lance Pagliaro, Masako Suzuki, John M. Greally, Dinesh Rakheja, R. Houston Thompson, Katalin Susztak, Thomas Witzig, Yiyu Zou, Amit Verma
Fangyang Wang, Damián Gatica, Zhang Xiao Ying, Luke F. Peterson, Peter Kim, Denzil Bernard, Kamlai Saiya-Cork, Shaomeng Wang, Mark S. Kaminski, Alfred E. Chang, Tycel Phillips, Daniel J. Klionsky, Sami N. MalekFangyang Wang, Damián Gatica, Zhang Xiao Ying, Luke F. Peterson, Peter Kim, Denzil Bernard, Kamlai Saiya-Cork, Shaomeng Wang, Mark S. Kaminski, Alfred E. Chang, Tycel Phillips, Daniel J. Klionsky, Sami N. Malek×Abstract
The discovery of recurrent mutations in subunits of the vacuolar-type H+-translocating ATPase (v-ATPase) in follicular lymphoma (FL) highlights a role for the amino acid– and energy-sensing pathway to mTOR in the pathogenesis of this disease. Here, through the use of complementary experimental approaches involving mammalian cells and Saccharomyces cerevisiae, we have demonstrated that mutations in the human v-ATPase subunit ATP6V1B2 (also known as Vma2 in yeast) activate autophagic flux and maintain mTOR/TOR in an active state. Engineered lymphoma cell lines and primary FL B cells carrying mutated ATP6V1B2 demonstrated a remarkable ability to survive low leucine concentrations. The treatment of primary FL B cells with inhibitors of autophagy uncovered an addiction for survival for FL B cells harboring ATP6V1B2 mutations. These data support the idea of mutational activation of autophagic flux by recurrent hotspot mutations in ATP6V1B2 as an adaptive mechanism in FL pathogenesis and as a possible new therapeutically targetable pathway.
Authors
Fangyang Wang, Damián Gatica, Zhang Xiao Ying, Luke F. Peterson, Peter Kim, Denzil Bernard, Kamlai Saiya-Cork, Shaomeng Wang, Mark S. Kaminski, Alfred E. Chang, Tycel Phillips, Daniel J. Klionsky, Sami N. Malek
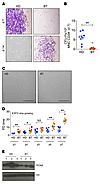
Shaikamjad Umesalma, Courtney A. Kaemmer, Jordan L. Kohlmeyer, Blake Letney, Angela M. Schab, Jacqueline A. Reilly, Ryan M. Sheehy, Jussara Hagen, Nitija Tiwari, Fenghuang Zhan, Mariah R. Leidinger, Thomas M. O’Dorisio, Joseph Dillon, Ronald A. Merrill, David K. Meyerholz, Abbey L. Perl, Bart J. Brown, Terry A. Braun, Aaron T. Scott, Timothy Ginader, Agshin F. Taghiyev, Gideon K. Zamba, James R. Howe, Stefan Strack, Andrew M. Bellizzi, Goutham Narla, Benjamin W. Darbro, Frederick W. Quelle, Dawn E. QuelleShaikamjad Umesalma, Courtney A. Kaemmer, Jordan L. Kohlmeyer, Blake Letney, Angela M. Schab, Jacqueline A. Reilly, Ryan M. Sheehy, Jussara Hagen, Nitija Tiwari, Fenghuang Zhan, Mariah R. Leidinger, Thomas M. O’Dorisio, Joseph Dillon, Ronald A. Merrill, David K. Meyerholz, Abbey L. Perl, Bart J. Brown, Terry A. Braun, Aaron T. Scott, Timothy Ginader, Agshin F. Taghiyev, Gideon K. Zamba, James R. Howe, Stefan Strack, Andrew M. Bellizzi, Goutham Narla, Benjamin W. Darbro, Frederick W. Quelle, Dawn E. Quelle×RABL6A inhibits tumor-suppressive PP2A/AKT signaling to drive pancreatic neuroendocrine tumor growth
Abstract
Hyperactivated AKT/mTOR signaling is a hallmark of pancreatic neuroendocrine tumors (PNETs). Drugs targeting this pathway are used clinically, but tumor resistance invariably develops. A better understanding of factors regulating AKT/mTOR signaling and PNET pathogenesis is needed to improve current therapies. We discovered that RABL6A, a new oncogenic driver of PNET proliferation, is required for AKT activity. Silencing RABL6A caused PNET cell-cycle arrest that coincided with selective loss of AKT-S473 (not T308) phosphorylation and AKT/mTOR inactivation. Restoration of AKT phosphorylation rescued the G1 phase block triggered by RABL6A silencing. Mechanistically, loss of AKT-S473 phosphorylation in RABL6A-depleted cells was the result of increased protein phosphatase 2A (PP2A) activity. Inhibition of PP2A restored phosphorylation of AKT-S473 in RABL6A-depleted cells, whereas PP2A reactivation using a specific small-molecule activator of PP2A (SMAP) abolished that phosphorylation. Moreover, SMAP treatment effectively killed PNET cells in a RABL6A-dependent manner and suppressed PNET growth in vivo. The present work identifies RABL6A as a new inhibitor of the PP2A tumor suppressor and an essential activator of AKT in PNET cells. Our findings offer what we believe is a novel strategy of PP2A reactivation for treatment of PNETs as well as other human cancers driven by RABL6A overexpression and PP2A inactivation.
Authors
Shaikamjad Umesalma, Courtney A. Kaemmer, Jordan L. Kohlmeyer, Blake Letney, Angela M. Schab, Jacqueline A. Reilly, Ryan M. Sheehy, Jussara Hagen, Nitija Tiwari, Fenghuang Zhan, Mariah R. Leidinger, Thomas M. O’Dorisio, Joseph Dillon, Ronald A. Merrill, David K. Meyerholz, Abbey L. Perl, Bart J. Brown, Terry A. Braun, Aaron T. Scott, Timothy Ginader, Agshin F. Taghiyev, Gideon K. Zamba, James R. Howe, Stefan Strack, Andrew M. Bellizzi, Goutham Narla, Benjamin W. Darbro, Frederick W. Quelle, Dawn E. Quelle
James V. McCann, Lin Xiao, Dae Joong Kim, Omar F. Khan, Piotr S. Kowalski, Daniel G. Anderson, Chad V. Pecot, Salma H. Azam, Joel S. Parker, Yihsuan S. Tsai, Alisa S. Wolberg, Stephen D. Turner, Kohei Tatsumi, Nigel Mackman, Andrew C. DudleyJames V. McCann, Lin Xiao, Dae Joong Kim, Omar F. Khan, Piotr S. Kowalski, Daniel G. Anderson, Chad V. Pecot, Salma H. Azam, Joel S. Parker, Yihsuan S. Tsai, Alisa S. Wolberg, Stephen D. Turner, Kohei Tatsumi, Nigel Mackman, Andrew C. Dudley×Abstract
In tumors, extravascular fibrin forms provisional scaffolds for endothelial cell (EC) growth and motility during angiogenesis. We report that fibrin-mediated angiogenesis was inhibited and tumor growth delayed following postnatal deletion of Tgfbr2 in the endothelium of Cdh5-CreERT2 Tgfbr2fl/fl mice (Tgfbr2iECKO mice). ECs from Tgfbr2iECKO mice failed to upregulate the fibrinolysis inhibitor plasminogen activator inhibitor 1 (Serpine1, also known as PAI-1), due in part to uncoupled TGF-β–mediated suppression of miR-30c. Bypassing TGF-β signaling with vascular tropic nanoparticles that deliver miR-30c antagomiRs promoted PAI-1–dependent tumor growth and increased fibrin abundance, whereas miR-30c mimics inhibited tumor growth and promoted vascular-directed fibrinolysis in vivo. Using single-cell RNA-Seq and a NanoString miRNA array, we also found that subtypes of ECs in tumors showed spectrums of Serpine1 and miR-30c expression levels, suggesting functional diversity in ECs at the level of individual cells; indeed, fresh EC isolates from lung and mammary tumor models had differential abilities to degrade fibrin and launch new vessel sprouts, a finding that was linked to their inverse expression patterns of miR-30c and Serpine1 (i.e., miR-30chi Serpine1lo ECs were poorly angiogenic and miR-30clo Serpine1hi ECs were highly angiogenic). Thus, by balancing Serpine1 expression in ECs downstream of TGF-β, miR-30c functions as a tumor suppressor in the tumor microenvironment through its ability to promote fibrin degradation and inhibit blood vessel formation.
Authors
James V. McCann, Lin Xiao, Dae Joong Kim, Omar F. Khan, Piotr S. Kowalski, Daniel G. Anderson, Chad V. Pecot, Salma H. Azam, Joel S. Parker, Yihsuan S. Tsai, Alisa S. Wolberg, Stephen D. Turner, Kohei Tatsumi, Nigel Mackman, Andrew C. Dudley
Harald Krenzlin, Prajna Behera, Viola Lorenz, Carmela Passaro, Mykola Zdioruk, Michal O. Nowicki, Korneel Grauwet, Hong Zhang, Magdalena Skubal, Hirotaka Ito, Rachel Zane, Michael Gutknecht, Marion B. Griessl, Franz Ricklefs, Lai Ding, Sharon Peled, Arun Rooj, C. David James, Charles S. Cobbs, Charles H. Cook, E. Antonio Chiocca, Sean E. LawlerHarald Krenzlin, Prajna Behera, Viola Lorenz, Carmela Passaro, Mykola Zdioruk, Michal O. Nowicki, Korneel Grauwet, Hong Zhang, Magdalena Skubal, Hirotaka Ito, Rachel Zane, Michael Gutknecht, Marion B. Griessl, Franz Ricklefs, Lai Ding, Sharon Peled, Arun Rooj, C. David James, Charles S. Cobbs, Charles H. Cook, E. Antonio Chiocca, Sean E. Lawler×Abstract
Cytomegalovirus (CMV) has been implicated in glioblastoma (GBM); however, a mechanistic connection in vivo has not been established. The purpose of this study is to characterize the effects of murine CMV (MCMV) on GBM growth in murine models. Syngeneic GBM models were established in mice perinatally infected with MCMV. We found that tumor growth was markedly enhanced in MCMV+ mice, with a significant reduction in overall survival compared with that of controls (P < 0.001). We observed increased angiogenesis and tumor blood flow in MCMV+ mice. MCMV reactivation was observed in intratumoral perivascular pericytes and tumor cells in mouse and human GBM specimens, and pericyte coverage of tumor vasculature was strikingly augmented in MCMV+ mice. We identified PDGF-D as a CMV-induced factor essential for pericyte recruitment, angiogenesis, and tumor growth. The antiviral drug cidofovir improved survival in MCMV+ mice, inhibiting MCMV reactivation, PDGF-D expression, pericyte recruitment, and tumor angiogenesis. These data show that MCMV potentiates GBM growth in vivo by increased pericyte recruitment and angiogenesis due to alterations in the secretome of CMV-infected cells. Our model provides evidence for a role of CMV in GBM growth and supports the application of antiviral approaches for GBM therapy.
Authors
Harald Krenzlin, Prajna Behera, Viola Lorenz, Carmela Passaro, Mykola Zdioruk, Michal O. Nowicki, Korneel Grauwet, Hong Zhang, Magdalena Skubal, Hirotaka Ito, Rachel Zane, Michael Gutknecht, Marion B. Griessl, Franz Ricklefs, Lai Ding, Sharon Peled, Arun Rooj, C. David James, Charles S. Cobbs, Charles H. Cook, E. Antonio Chiocca, Sean E. Lawler
×Abstract
Retinoic acid–related orphan receptor α (RORα) is considered a key regulator of polarization in liver macrophages that is closely related to nonalcoholic steatohepatitis (NASH) pathogenesis. However, hepatic microenvironments that support the function of RORα as a polarity regulator were largely unknown. Here, we identified maresin 1 (MaR1), a docosahexaenoic acid (DHA) metabolite with a function of specialized proresolving mediator, as an endogenous ligand of RORα. MaR1 enhanced the expression and transcriptional activity of RORα and thereby increased the M2 polarity of liver macrophages. Administration of MaR1 protected mice from high-fat diet–induced NASH in a RORα-dependent manner. Surprisingly, RORα increased the level of MaR1 through transcriptional induction of 12-lipoxygenase (12-LOX), a key enzyme in MaR1 biosynthesis. Furthermore, we demonstrated that modulation of 12-LOX activity enhanced the protective function of DHA against NASH. Together, these results suggest that the MaR1/RORα/12-LOX autoregulatory circuit could offer potential therapeutic strategies for curing NASH.
Authors
Yong-Hyun Han, Kyong-Oh Shin, Ju-Yeon Kim, Daulat B. Khadka, Hyeon-Ji Kim, Yong-Moon Lee, Won-Jea Cho, Ji-Young Cha, Bong-Jin Lee, Mi-Ock Lee
Sarah Tomkovich, Christine M. Dejea, Kathryn Winglee, Julia L. Drewes, Liam Chung, Franck Housseau, Jillian L. Pope, Josee Gauthier, Xiaolun Sun, Marcus Mühlbauer, Xiuli Liu, Payam Fathi, Robert A. Anders, Sepideh Besharati, Ernesto Perez-Chanona, Ye Yang, Hua Ding, Xinqun Wu, Shaoguang Wu, James R. White, Raad Z. Gharaibeh, Anthony A. Fodor, Hao Wang, Drew M. Pardoll, Christian Jobin, Cynthia L. SearsSarah Tomkovich, Christine M. Dejea, Kathryn Winglee, Julia L. Drewes, Liam Chung, Franck Housseau, Jillian L. Pope, Josee Gauthier, Xiaolun Sun, Marcus Mühlbauer, Xiuli Liu, Payam Fathi, Robert A. Anders, Sepideh Besharati, Ernesto Perez-Chanona, Ye Yang, Hua Ding, Xinqun Wu, Shaoguang Wu, James R. White, Raad Z. Gharaibeh, Anthony A. Fodor, Hao Wang, Drew M. Pardoll, Christian Jobin, Cynthia L. Sears×Abstract
Mucus-invasive bacterial biofilms are identified on the colon mucosa of approximately 50% of colorectal cancer (CRC) patients and approximately 13% of healthy subjects. Here, we test the hypothesis that human colon biofilms comprise microbial communities that are carcinogenic in CRC mouse models. Homogenates of human biofilm-positive colon mucosa were prepared from tumor patients (tumor and paired normal tissues from surgical resections) or biofilm-positive biopsies from healthy individuals undergoing screening colonoscopy; homogenates of biofilm-negative colon biopsies from healthy individuals undergoing screening colonoscopy served as controls. After 12 weeks, biofilm-positive, but not biofilm-negative, human colon mucosal homogenates induced colon tumor formation in 3 mouse colon tumor models (germ-free ApcMinΔ850/+;Il10–/– or ApcMinΔ850/+ and specific pathogen–free ApcMinΔ716/+ mice). Remarkably, biofilm-positive communities from healthy colonoscopy biopsies induced colon inflammation and tumors similarly to biofilm-positive tumor tissues. By 1 week, biofilm-positive human tumor homogenates, but not healthy biopsies, displayed consistent bacterial mucus invasion and biofilm formation in mouse colons. 16S rRNA gene sequencing and RNA-Seq analyses identified compositional and functional microbiota differences between mice colonized with biofilm-positive and biofilm-negative communities. These results suggest human colon mucosal biofilms, whether from tumor hosts or healthy individuals undergoing screening colonoscopy, are carcinogenic in murine models of CRC.
Authors
Sarah Tomkovich, Christine M. Dejea, Kathryn Winglee, Julia L. Drewes, Liam Chung, Franck Housseau, Jillian L. Pope, Josee Gauthier, Xiaolun Sun, Marcus Mühlbauer, Xiuli Liu, Payam Fathi, Robert A. Anders, Sepideh Besharati, Ernesto Perez-Chanona, Ye Yang, Hua Ding, Xinqun Wu, Shaoguang Wu, James R. White, Raad Z. Gharaibeh, Anthony A. Fodor, Hao Wang, Drew M. Pardoll, Christian Jobin, Cynthia L. Sears
Kwi Hye Koh, Yanxia Cao, Steve Mangos, Nicholas J. Tardi, Ranadheer R. Dande, Ha Won Lee, Beata Samelko, Mehmet M. Altintas, Vincent P. Schmitz, Hyun Lee, Kamalika Mukherjee, Vasil Peev, David J. Cimbaluk, Jochen Reiser, Eunsil HahmKwi Hye Koh, Yanxia Cao, Steve Mangos, Nicholas J. Tardi, Ranadheer R. Dande, Ha Won Lee, Beata Samelko, Mehmet M. Altintas, Vincent P. Schmitz, Hyun Lee, Kamalika Mukherjee, Vasil Peev, David J. Cimbaluk, Jochen Reiser, Eunsil Hahm×Abstract
Soluble urokinase receptor (suPAR) is a circulatory molecule that activates αvβ3 integrin on podocytes, causes foot process effacement, and contributes to proteinuric kidney disease. While active integrin can be targeted by antibodies and small molecules, endogenous inhibitors haven’t been discovered yet. Here we report what we believe is a novel renoprotective role for the inducible costimulator ligand (ICOSL) in early kidney disease through its selective binding to podocyte αvβ3 integrin. Contrary to ICOSL’s immune-regulatory role, ICOSL in nonhematopoietic cells limited the activation of αvβ3 integrin. Specifically, ICOSL contains the arginine-glycine-aspartate (RGD) motif, which allowed for a high-affinity and selective binding to αvβ3 and modulation of podocyte adhesion. This binding was largely inhibited either by a synthetic RGD peptide or by a disrupted RGD sequence in ICOSL. ICOSL binding favored the active αvβ3 rather than the inactive form and showed little affinity for other integrins. Consistent with the rapid induction of podocyte ICOSL by inflammatory stimuli, glomerular ICOSL expression was increased in biopsies of early-stage human proteinuric kidney diseases. Icosl deficiency in mice resulted in an increased susceptibility to proteinuria that was rescued by recombinant ICOSL. Our work identified a potentially novel role for ICOSL, which serves as an endogenous αvβ3-selective antagonist to maintain glomerular filtration.
Authors
Kwi Hye Koh, Yanxia Cao, Steve Mangos, Nicholas J. Tardi, Ranadheer R. Dande, Ha Won Lee, Beata Samelko, Mehmet M. Altintas, Vincent P. Schmitz, Hyun Lee, Kamalika Mukherjee, Vasil Peev, David J. Cimbaluk, Jochen Reiser, Eunsil Hahm
Yuan Tian, Mariana Babor, Jerome Lane, Grégory Seumois, Shu Liang, N.D. Suraj Goonawardhana, Aruna D. De Silva, Elizabeth J. Phillips, Simon A. Mallal, Ricardo da Silva Antunes, Alba Grifoni, Pandurangan Vijayanand, Daniela Weiskopf, Bjoern Peters, Alessandro SetteYuan Tian, Mariana Babor, Jerome Lane, Grégory Seumois, Shu Liang, N.D. Suraj Goonawardhana, Aruna D. De Silva, Elizabeth J. Phillips, Simon A. Mallal, Ricardo da Silva Antunes, Alba Grifoni, Pandurangan Vijayanand, Daniela Weiskopf, Bjoern Peters, Alessandro Sette×Abstract
Accumulating evidence demonstrates that CD8+ T cells contribute to protection from severe dengue virus (DENV) disease and vaccine efficacy. Nevertheless, molecular programs associated with DENV-specific CD8+ T cell subsets have not been defined. Here, we studied the transcriptomic profiles of human DENV-specific CD8+ T cells isolated after stimulation with DENV epitopes from donors who had been infected with DENV multiple times and would therefore be expected to have significant levels of adaptive immunity. We found that DENV-specific CD8+ T cells mainly consisted of effector memory subsets, namely CD45RA−CCR7− effector memory (Tem) and CD45RA+CCR7− effector memory re-expressing CD45RA (Temra) cells, which enacted specific gene expression profiles upon stimulation with cognate antigens. DENV-specific CD8+ T cell subsets in general, and Temra cells in particular, were fully activated and polyfunctional, yet associated with relatively narrow transcriptional responses. Furthermore, we found that DENV-specific CD8+ Tem and Temra cells showed some unique T cell receptor features in terms of overlap and variable (V) gene usage. This study provides a transcriptomic definition of DENV-specific activated human CD8+ T cell subsets and defines a benchmark profile that vaccine-specific responses could aim to reproduce.
Authors
Yuan Tian, Mariana Babor, Jerome Lane, Grégory Seumois, Shu Liang, N.D. Suraj Goonawardhana, Aruna D. De Silva, Elizabeth J. Phillips, Simon A. Mallal, Ricardo da Silva Antunes, Alba Grifoni, Pandurangan Vijayanand, Daniela Weiskopf, Bjoern Peters, Alessandro Sette
×Abstract
Pancreatic ductal adenocarcinoma (PDAC) represents an immune quiescent tumor that is resistant to immune checkpoint inhibitors. Previously, our group has shown that a GM-CSF–secreting allogenic pancreatic tumor cell vaccine (GVAX) may prime the tumor microenvironment by inducing intratumoral T cell infiltration. Here, we show that untreated PDACs express minimal indoleamine-2,3-dioxygenase (IDO1); however, GVAX therapy induced IDO1 expression on tumor epithelia as well as vaccine-induced tertiary lymphoid aggregates. IDO1 expression plays a role in regulating the polarization of Th1, Th17, and possibly T regulatory cells in PDAC tumors. IDO1 inhibitor enhanced antitumor efficacy of GVAX in a murine model of PDACs. The combination of vaccine and IDO1 inhibitor enhanced intratumoral T cell infiltration and function, but adding anti–PD-L1 antibody to the combination did not offer further synergy and in fact may have had a negative interaction, decreasing the number of intratumoral effector T cells. Additionally, IDO1 inhibitor in the presence of vaccine therapy did not significantly modulate intratumoral myeloid-derived suppressor cells quantitatively, but diminished their suppressive effect on CD8+ proliferation. Our study supports the combination of IDO1 inhibitor and vaccine therapy; however, it does not support the combination of IDO1 inhibitor and anti–PD-1/PD-L1 antibody for T cell–inflamed tumors such as PDACs treated with vaccine therapy.
Authors
Alex B. Blair, Jennifer Kleponis, Dwayne L. Thomas II, Stephen T. Muth, Adrian G. Murphy, Victoria Kim, Lei Zheng
Yueqin Zhou, Sharon Carmona, A.K.M.G. Muhammad, Shaughn Bell, Jesse Landeros, Michael Vazquez, Ritchie Ho, Antonietta Franco, Bin Lu, Gerald W. Dorn II, Shaomei Wang, Cathleen M. Lutz, Robert H. BalohYueqin Zhou, Sharon Carmona, A.K.M.G. Muhammad, Shaughn Bell, Jesse Landeros, Michael Vazquez, Ritchie Ho, Antonietta Franco, Bin Lu, Gerald W. Dorn II, Shaomei Wang, Cathleen M. Lutz, Robert H. Baloh×Abstract
Mitofusin-2 (MFN2) is a mitochondrial outer-membrane protein that plays a pivotal role in mitochondrial dynamics in most tissues, yet mutations in MFN2, which cause Charcot-Marie-Tooth disease type 2A (CMT2A), primarily affect the nervous system. We generated a transgenic mouse model of CMT2A that developed severe early onset vision loss and neurological deficits, axonal degeneration without cell body loss, and cytoplasmic and axonal accumulations of fragmented mitochondria. While mitochondrial aggregates were labeled for mitophagy, mutant MFN2 did not inhibit Parkin-mediated degradation, but instead had a dominant negative effect on mitochondrial fusion only when MFN1 was at low levels, as occurs in neurons. Finally, using a transgenic approach, we found that augmenting the level of MFN1 in the nervous system in vivo rescued all phenotypes in mutant MFN2R94Q-expressing mice. These data demonstrate that the MFN1/MFN2 ratio is a key determinant of tissue specificity in CMT2A and indicate that augmentation of MFN1 in the nervous system is a viable therapeutic strategy for the disease.
Authors
Yueqin Zhou, Sharon Carmona, A.K.M.G. Muhammad, Shaughn Bell, Jesse Landeros, Michael Vazquez, Ritchie Ho, Antonietta Franco, Bin Lu, Gerald W. Dorn II, Shaomei Wang, Cathleen M. Lutz, Robert H. Baloh
Ana I. Casas, Pamela W.M. Kleikers, Eva Geuss, Friederike Langhauser, Thure Adler, Dirk H. Busch, Valerie Gailus-Durner, Martin Hrabê de Angelis, Javier Egea, Manuela G. Lopez, Christoph Kleinschnitz, Harald H.H.W. SchmidtAna I. Casas, Pamela W.M. Kleikers, Eva Geuss, Friederike Langhauser, Thure Adler, Dirk H. Busch, Valerie Gailus-Durner, Martin Hrabê de Angelis, Javier Egea, Manuela G. Lopez, Christoph Kleinschnitz, Harald H.H.W. Schmidt×Abstract
Ischemic stroke is a predominant cause of disability worldwide, with thrombolytic or mechanical removal of the occlusion being the only therapeutic option. Reperfusion bears the risk of an acute deleterious calcium-dependent breakdown of the blood-brain barrier. Its mechanism, however, is unknown. Here, we identified type 5 NADPH oxidase (NOX5), a calcium-activated, ROS-forming enzyme, as the missing link. Using a humanized knockin (KI) mouse model and in vitro organotypic cultures, we found that reoxygenation or calcium overload increased brain ROS levels in a NOX5-dependent manner. In vivo, postischemic ROS formation, infarct volume, and functional outcomes were worsened in NOX5-KI mice. Of clinical and therapeutic relevance, in a human blood-barrier model, pharmacological NOX inhibition also prevented acute reoxygenation-induced leakage. Our data support further evaluation of poststroke recanalization in the presence of NOX inhibition for limiting stroke-induced damage.
Authors
Ana I. Casas, Pamela W.M. Kleikers, Eva Geuss, Friederike Langhauser, Thure Adler, Dirk H. Busch, Valerie Gailus-Durner, Martin Hrabê de Angelis, Javier Egea, Manuela G. Lopez, Christoph Kleinschnitz, Harald H.H.W. Schmidt
Joseph A. Hippensteel, Brian J. Anderson, James E. Orfila, Sarah A. McMurtry, Robert M. Dietz, Guowei Su, Joshay A. Ford, Kaori Oshima, Yimu Yang, Fuming Zhang, Xiaorui Han, Yanlei Yu, Jian Liu, Robert J. Linhardt, Nuala J. Meyer, Paco S. Herson, Eric P. SchmidtJoseph A. Hippensteel, Brian J. Anderson, James E. Orfila, Sarah A. McMurtry, Robert M. Dietz, Guowei Su, Joshay A. Ford, Kaori Oshima, Yimu Yang, Fuming Zhang, Xiaorui Han, Yanlei Yu, Jian Liu, Robert J. Linhardt, Nuala J. Meyer, Paco S. Herson, Eric P. Schmidt×Abstract
Septic patients frequently develop cognitive impairment that persists beyond hospital discharge. The impact of sepsis on electrophysiological and molecular determinants of learning is underexplored. We observed that mice that survived sepsis or endotoxemia experienced loss of hippocampal long-term potentiation (LTP), a brain-derived neurotrophic factor–mediated (BDNF-mediated) process responsible for spatial memory formation. Memory impairment occurred despite preserved hippocampal BDNF content and could be reversed by stimulation of BDNF signaling, suggesting the presence of a local BDNF inhibitor. Sepsis is associated with degradation of the endothelial glycocalyx, releasing heparan sulfate fragments (of sufficient size and sulfation to bind BDNF) into the circulation. Heparan sulfate fragments penetrated the hippocampal blood-brain barrier during sepsis and inhibited BDNF-mediated LTP. Glycoarray approaches demonstrated that the avidity of heparan sulfate for BDNF increased with sulfation at the 2-O position of iduronic acid and the N position of glucosamine. Circulating heparan sulfate in endotoxemic mice and septic humans was enriched in 2-O– and N-sulfated disaccharides; furthermore, the presence of these sulfation patterns in the plasma of septic patients at intensive care unit (ICU) admission predicted persistent cognitive impairment 14 days after ICU discharge or at hospital discharge. Our findings indicate that circulating 2-O– and N-sulfated heparan sulfate fragments contribute to septic cognitive impairment.
Authors
Joseph A. Hippensteel, Brian J. Anderson, James E. Orfila, Sarah A. McMurtry, Robert M. Dietz, Guowei Su, Joshay A. Ford, Kaori Oshima, Yimu Yang, Fuming Zhang, Xiaorui Han, Yanlei Yu, Jian Liu, Robert J. Linhardt, Nuala J. Meyer, Paco S. Herson, Eric P. Schmidt
Tina Gruosso, Mathieu Gigoux, Venkata Satya Kumar Manem, Nicholas Bertos, Dongmei Zuo, Irina Perlitch, Sadiq Mehdi Ismail Saleh, Hong Zhao, Margarita Souleimanova, Radia Marie Johnson, Anne Monette, Valentina Muñoz Ramos, Michael Trevor Hallett, John Stagg, Réjean Lapointe, Atilla Omeroglu, Sarkis Meterissian, Laurence Buisseret, Gert Van den Eynden, Roberto Salgado, Marie-Christine Guiot, Benjamin Haibe-Kains, Morag ParkTina Gruosso, Mathieu Gigoux, Venkata Satya Kumar Manem, Nicholas Bertos, Dongmei Zuo, Irina Perlitch, Sadiq Mehdi Ismail Saleh, Hong Zhao, Margarita Souleimanova, Radia Marie Johnson, Anne Monette, Valentina Muñoz Ramos, Michael Trevor Hallett, John Stagg, Réjean Lapointe, Atilla Omeroglu, Sarkis Meterissian, Laurence Buisseret, Gert Van den Eynden, Roberto Salgado, Marie-Christine Guiot, Benjamin Haibe-Kains, Morag Park×Abstract
Understanding the tumor immune microenvironment (TIME) promises to be key for optimal cancer therapy, especially in triple-negative breast cancer (TNBC). Integrating spatial resolution of immune cells with laser capture microdissection gene expression profiles, we defined distinct TIME stratification in TNBC, with implications for current therapies including immune checkpoint blockade. TNBCs with an immunoreactive microenvironment exhibited tumoral infiltration of granzyme B+CD8+ T cells (GzmB+CD8+ T cells), a type 1 IFN signature, and elevated expression of multiple immune inhibitory molecules including indoleamine 2,3-dioxygenase (IDO) and programmed cell death ligand 1 (PD-L1), and resulted in good outcomes. An “immune-cold” microenvironment with an absence of tumoral CD8+ T cells was defined by elevated expression of the immunosuppressive marker B7-H4, signatures of fibrotic stroma, and poor outcomes. A distinct poor-outcome immunomodulatory microenvironment, hitherto poorly characterized, exhibited stromal restriction of CD8+ T cells, stromal expression of PD-L1, and enrichment for signatures of cholesterol biosynthesis. Metasignatures defining these TIME subtypes allowed us to stratify TNBCs, predict outcomes, and identify potential therapeutic targets for TNBC.
Authors
Tina Gruosso, Mathieu Gigoux, Venkata Satya Kumar Manem, Nicholas Bertos, Dongmei Zuo, Irina Perlitch, Sadiq Mehdi Ismail Saleh, Hong Zhao, Margarita Souleimanova, Radia Marie Johnson, Anne Monette, Valentina Muñoz Ramos, Michael Trevor Hallett, John Stagg, Réjean Lapointe, Atilla Omeroglu, Sarkis Meterissian, Laurence Buisseret, Gert Van den Eynden, Roberto Salgado, Marie-Christine Guiot, Benjamin Haibe-Kains, Morag Park
-
Retraction
Terence K. Lee, Saravana R.K. Murthy, Niamh X. Cawley, Savita Dhanvantari, Stephen M. Hewitt, Hong Lou, Tracy Lau, Stephanie Ma, Thanh Huynh, Robert A. Wesley, Irene O. Ng, Karel Pacak, Ronnie T. Poon, Y. Peng LohTerence K. Lee, Saravana R.K. Murthy, Niamh X. Cawley, Savita Dhanvantari, Stephen M. Hewitt, Hong Lou, Tracy Lau, Stephanie Ma, Thanh Huynh, Robert A. Wesley, Irene O. Ng, Karel Pacak, Ronnie T. Poon, Y. Peng Loh×
Abstract
Authors
Terence K. Lee, Saravana R.K. Murthy, Niamh X. Cawley, Savita Dhanvantari, Stephen M. Hewitt, Hong Lou, Tracy Lau, Stephanie Ma, Thanh Huynh, Robert A. Wesley, Irene O. Ng, Karel Pacak, Ronnie T. Poon, Y. Peng Loh
-
Expressions of Concern
Peter Huebener, Jean-Philippe Pradere, Celine Hernandez, Geum-Youn Gwak, Jorge Matias Caviglia, Xueru Mu, John D. Loike, Rosalind E. Jenkins, Daniel J. Antoine, Robert F. SchwabePeter Huebener, Jean-Philippe Pradere, Celine Hernandez, Geum-Youn Gwak, Jorge Matias Caviglia, Xueru Mu, John D. Loike, Rosalind E. Jenkins, Daniel J. Antoine, Robert F. Schwabe×
Abstract
Authors
Peter Huebener, Jean-Philippe Pradere, Celine Hernandez, Geum-Youn Gwak, Jorge Matias Caviglia, Xueru Mu, John D. Loike, Rosalind E. Jenkins, Daniel J. Antoine, Robert F. Schwabe
×Abstract
Authors
Celine Hernandez, Peter Huebener, Jean-Philippe Pradere, Daniel J. Antoine, Richard A. Friedman, Robert F. Schwabe
-
Corrigenda
Donghyun D. Lee, Ricardo Leão, Martin Komosa, Marco Gallo, Cindy H. Zhang, Tatiana Lipman, Marc Remke, Abolfazl Heidari, Nuno Miguel Nunes, Joana D. Apolónio, Aryeh J. Price, Ramon Andrade De Mello, João S. Dias, David Huntsman, Thomas Hermanns, Peter J. Wild, Robert Vanner, Gelareh Zadeh, Jason Karamchandani, Sunit Das, Michael D. Taylor, Cynthia E. Hawkins, Jonathan D. Wasserman, Arnaldo Figueiredo, Robert J. Hamilton, Mark D. Minden, Khalida Wani, Bill Diplas, Hai Yan, Kenneth Aldape, Mohammad R. Akbari, Arnavaz Danesh, Trevor J. Pugh, Peter B. Dirks, Pedro Castelo-Branco, Uri TaboriDonghyun D. Lee, Ricardo Leão, Martin Komosa, Marco Gallo, Cindy H. Zhang, Tatiana Lipman, Marc Remke, Abolfazl Heidari, Nuno Miguel Nunes, Joana D. Apolónio, Aryeh J. Price, Ramon Andrade De Mello, João S. Dias, David Huntsman, Thomas Hermanns, Peter J. Wild, Robert Vanner, Gelareh Zadeh, Jason Karamchandani, Sunit Das, Michael D. Taylor, Cynthia E. Hawkins, Jonathan D. Wasserman, Arnaldo Figueiredo, Robert J. Hamilton, Mark D. Minden, Khalida Wani, Bill Diplas, Hai Yan, Kenneth Aldape, Mohammad R. Akbari, Arnavaz Danesh, Trevor J. Pugh, Peter B. Dirks, Pedro Castelo-Branco, Uri Tabori×
Abstract
Authors
Donghyun D. Lee, Ricardo Leão, Martin Komosa, Marco Gallo, Cindy H. Zhang, Tatiana Lipman, Marc Remke, Abolfazl Heidari, Nuno Miguel Nunes, Joana D. Apolónio, Aryeh J. Price, Ramon Andrade De Mello, João S. Dias, David Huntsman, Thomas Hermanns, Peter J. Wild, Robert Vanner, Gelareh Zadeh, Jason Karamchandani, Sunit Das, Michael D. Taylor, Cynthia E. Hawkins, Jonathan D. Wasserman, Arnaldo Figueiredo, Robert J. Hamilton, Mark D. Minden, Khalida Wani, Bill Diplas, Hai Yan, Kenneth Aldape, Mohammad R. Akbari, Arnavaz Danesh, Trevor J. Pugh, Peter B. Dirks, Pedro Castelo-Branco, Uri Tabori
Peter Huebener, Jean-Philippe Pradere, Celine Hernandez, Geum-Youn Gwak, Jorge Matias Caviglia, Xueru Mu, John D. Loike, Rosalind E. Jenkins, Daniel J. Antoine, Robert F. SchwabePeter Huebener, Jean-Philippe Pradere, Celine Hernandez, Geum-Youn Gwak, Jorge Matias Caviglia, Xueru Mu, John D. Loike, Rosalind E. Jenkins, Daniel J. Antoine, Robert F. Schwabe×Abstract
Authors
Peter Huebener, Jean-Philippe Pradere, Celine Hernandez, Geum-Youn Gwak, Jorge Matias Caviglia, Xueru Mu, John D. Loike, Rosalind E. Jenkins, Daniel J. Antoine, Robert F. Schwabe
×Abstract
Authors
Celine Hernandez, Peter Huebener, Jean-Philippe Pradere, Daniel J. Antoine, Richard A. Friedman, Robert F. Schwabe



Copyright © 2025 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)