Review
Abstract
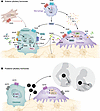
Bone is a highly dynamic and purposefully organized structure that remodels constantly throughout adult life. Disordered bone remodeling, in which resorption of old bone by osteoclasts exceeds new bone formation by osteoblasts, results in bone loss, which, in turn, is associated with debilitating conditions, including osteoporosis and metastatic bone disease. The past decade has revealed vital new insights into the role of the central nervous system in skeletal regulation. These studies have led to a better understanding of physiologic circuitry, enabled us to revisit disease pathophysiology, and in doing so, prompted the creation of candidate therapeutics. The central neural control of bone is exerted through two arms — an amplitude-modulated (AM) neurohormonal arm that relies on changes in circulating levels of anterior and posterior pituitary hormones, which act on bone directly, and a frequency-modulated (FM) arm that arises from changes in the firing frequency of sympathetic, parasympathetic, and sensory nerves that innervate bone. Here, we review the medical consequences arising from the dysfunction of the AM and FM arms, as well as studies that have unmasked promising therapeutic targets.
Authors
Mone Zaidi, Se-Min Kim, Vitaly Ryu, Daria Lizneva, Terry F. Davies, Clifford J. Rosen, Tony Yuen, Andrea Giustina
Abstract
Although combination antiretroviral therapy (ART) has dramatically reduced the incidence of severe HIV-associated neurological disease, the central nervous system (CNS) remains a viral sanctuary in which inflammation and brain injury persist despite systemic viral suppression. Here, we synthesize evidence that ongoing HIV-associated brain injury is sustained not primarily by unchecked viral replication but by persistent viral transcription from defective proviruses, immune-mediated synaptic dysfunction driven by bystander activation, and long-lived microglial reprogramming shaped by epigenetic “training.” We highlight how emerging single-cell multiomics and “liquid biopsy” approaches are redefining our understanding of the CNS reservoir at high resolution. We further discuss the growing emphasis on biologically anchored, molecularly defined disease subtypes as a means to disentangle HIV-specific pathology from the confounding overlap of aging and multimorbidity, which have increased in the ART era. Finally, we underscore the necessity of human-centered translational studies to validate preclinical findings, outlining how these molecular insights pave the way for precision therapeutics and CNS-targeted cure strategies.
Authors
Paraskevas Filippidis, Shelli F. Farhadian
Abstract
Neurodegenerative diseases arise from interactions among pathogenic proteins, immune responses, and diverse environmental or age-related stressors that disrupt CNS homeostasis. CNS resident microglia detect self-derived danger signals through pattern recognition receptors, and their activation can promote clearance of aberrant proteins, including amyloid-β, tau, α-synuclein, and TAR DNA-binding protein 43. However, microglial activation may also drive maladaptive states that amplify neuroinflammation. Microglial transitions are further shaped by receptor-mediated signaling and antigen presentation pathways that integrate environmental cues with functional responses. Adaptive immune cells contribute additional layers of regulation, with CD8+ and CD4+ T cells exerting neuroprotective or neurotoxic effects depending on disease context, activation state, and antigen specificity. The identification of granzyme K–expressing CD8+ T cells in several neurodegenerative conditions highlights the growing recognition that distinct T cell subsets may have specialized roles in disease. Aging, repetitive head injury, and viral infection further alter microglial phenotypes, weaken barrier integrity, promote T cell recruitment, and prime the CNS for chronic inflammation. In this review, we synthesize current knowledge of innate and adaptive immune mechanisms in neurodegeneration, examine how external factors influence these responses, and consider how these insights may guide future therapeutic strategies.
Authors
Yvonne L. Latour, Dorian B. McGavern
Abstract
Lysosomes function as metabolic control centers that integrate degradation, nutrient sensing, and stress signaling. In neurons, which must maintain proteostasis and energetic balance throughout life, lysosomal homeostasis determines cellular resilience. Emerging evidence identifies lysosomal injury and defective repair as common denominators across neurodegenerative diseases. Damage to the lysosomal membrane caused by oxidative stress, lipid imbalance, or genetic mutations triggers a hierarchical quality control cascade. Early lesions recruit the endosomal sorting complex required for transport (ESCRT) machinery for mechanical resealing, while larger ruptures activate lipid-centered recovery modules. When repair fails, lysophagy eliminates irreparable organelles and a TFEB-dependent transcriptional program regenerates the lysosomal pool. These tightly coupled responses safeguard neurons from catastrophic proteostatic collapse. Their impairment, through mutations in lysosomal proteins, or through aging, produces the lysosomal fragility that underlies Alzheimer disease, Parkinson disease, amyotrophic lateral sclerosis/frontotemporal dementia, and Huntington disease. Crosstalk between lysosomes, mitochondria, and ER integrates local damage with systemic metabolic adaptation, while dysregulated lysosomal exocytosis and inflammation propagate pathology. Understanding how ESCRT complexes, lipid transport, and transcriptional renewal cooperate to preserve lysosomal integrity reveals unifying principles of neurodegeneration and defines molecular targets for intervention. Restoring lysosomal repair and renewal offers a rational path toward preventing neuronal loss.
Authors
Stefano De Tito, Sharon A. Tooze
Abstract
Recent advances in genomic technologies have greatly enhanced our understanding of neurodegeneration. Techniques like whole-genome sequencing, long-read sequencing, and large-scale population studies have expanded the range of identified genetic risk factors, uncovering new disease mechanisms and biological pathways that could serve as therapeutic targets. However, translating these genetic insights into clinical practice remains difficult because of challenges in interpreting variants and the limited functional validation of new discoveries. This Review highlights the key genomic technologies advancing diagnosis and research in neurodegeneration. We focus on improvements in variant classification, detection of structural variants and repeat expansions, and combining transcriptomic, proteomic, and functional data to better determine variant pathogenicity. The ongoing integration of genomics, molecular neurobiology, and data science offers great potential for more accurate, biologically informed diagnosis and treatment of neurodegenerative disorders.
Authors
Maurizio Grassano, Alice B. Schindler, Bryan J. Traynor, Sonja W. Scholz
Abstract
Nearly two-thirds of patients with Alzheimer disease (AD) are women, most of them postmenopausal. While sex differences in AD have historically been attributed to women’s relative longevity, accumulating evidence challenges that view, pointing to female sex–specific biological underpinnings. In particular, neuroendocrine aging and the hormonal shifts that accompany the menopause transition have emerged as potentially modifiable AD risk factors in women. Yet, key neuroendocrine aging-related factors linked to increased AD and dementia risk, such as early menopause, premenopausal bilateral oophorectomy, frequent vasomotor symptoms, and midlife cognitive and mood disturbances, remain underinvestigated. Additionally, although a growing evidence base highlights the potential of menopause hormone therapy for AD prevention, particularly in women undergoing oophorectomy, progress remains hindered by a lack of clinical trials and biomarker-driven studies. This Review calls for a paradigm shift: from viewing AD risk as a byproduct of generalized aging to validating midlife neuroendocrine aging as a distinct window of vulnerability, and an opportunity for prevention. By 2050, over 1.2 billion women worldwide will be in or approaching menopause. The stakes are global, and the opportunity is urgent: to redefine AD prevention through sex-specific, time-sensitive, and biologically informed strategies that translate science into scalable, actionable care.
Authors
Lisa Mosconi
Abstract
Amyotrophic lateral sclerosis (ALS) and frontotemporal dementia (FTD) are progressive neurodegenerative diseases characterized by the nuclear clearance and cytoplasmic aggregation of transactive response DNA/RNA-binding protein of 43 kDa (TDP43). Alternative splicing of TARDBP, the gene encoding TDP43, leads to a surprising diversity of RNA and protein isoforms with unique functions and potential implications for disease pathogenesis. Here, we review the production, properties, and functional consequences of alternative splicing in the development of ALS and FTD, focusing primarily on TDP43 due to its integral connection with the pathogenesis of sporadic as well as familial forms of these diseases. We synthesize current evidence on the biology of alternative TARDBP splicing, highlight key questions regarding its role in TDP43 proteinopathies such as ALS and FTD, and touch on the larger phenomenon of alternative splicing and its relationship to disease.
Authors
Morgan R. Miller, Megan Dykstra, Sami Barmada
Abstract
Neurodegenerative diseases are characterized by protein misfolding and the selective vulnerability of specific neuronal subtypes. This selective vulnerability presents a paradox; most neurodegenerative disease genes are expressed broadly throughout the brain, and some ubiquitously, but only certain types of neurons are lost while others are resistant. The molecular basis for selective neuronal vulnerability has remained a mystery, but recent genomics technological innovations are starting to provide mechanistic insights. Here, we review how single-cell genomics techniques — single-cell transcriptomics, single-cell epigenomics, and spatial transcriptomics — advance our molecular understanding of selective vulnerability and neurodegeneration across Alzheimer disease, Parkinson disease, amyotrophic lateral sclerosis, frontotemporal dementia, and Huntington disease. Together, these approaches reveal the cell types affected in disease, define disease-associated molecular states, nominate candidate determinants of vulnerability and degeneration, and situate degenerating neurons within their local tissue context. Continued development and application of these techniques, including single-cell perturbation screens, will expand descriptive atlases of relevant cell types in health and disease and identify causal mechanisms, revealing the molecular basis of vulnerability and degeneration and informing therapeutic development.
Authors
Olivia Gautier, Thao P. Nguyen, Aaron D. Gitler
Abstract
Urothelial cancers of the urinary tract are the fourth most common malignancy in men, with a shifting demographic affecting younger patients and an increasing incidence in females. In this Review, we discuss recent discoveries and paradigm-shifting clinical trials that impact all stages of urothelial cancer. New therapeutics and drug-delivery devices have led to multiple approvals for treatments of non-muscle invasive bladder cancer. The addition of chemotherapy, immunotherapy, and antibody-drug conjugates is transforming perioperative treatment for patients with muscle-invasive bladder cancer. The use of liquid biomarkers, circulating tumor DNA, and urinary tumor DNA is aiding the identification of patients at risk for local recurrence and possibly those who can avoid systemic therapy. Finally, integrating biomarkers and systemic treatments is creating a paradigm that could lead to the successful treatment of bladder cancer without requiring bladder removal. Overall, these advancements in biomarkers and novel therapeutics are likely to dramatically improve survival for bladder cancer.
Authors
Joshua J. Meeks
Abstract
Diabetic retinopathy (DR), the most common microvascular complication in patients with diabetes mellitus (DM), is a leading cause of vision loss worldwide. Sustained hyperglycemia plays a central role in promoting DR. However, tight glycemic control does not prevent — and indeed sometimes worsens — DR, highlighting the importance of ongoing studies aimed at improving our understanding of this complex disease. Over the last few decades, the dogma that DR is a vascular disease that results in secondary neuronal injury has evolved, as emerging evidence suggests that neurodegeneration occurs in parallel with or prior to vascular cell injury in the retina of patients with DM. This has led to appreciation of DR as a neurovascular disease, characterized by microvascular injury and neurodegeneration, both of which contribute to vision loss. Here, we explore how molecular stress (i.e., glucose dysregulation, dysmetabolism, oxidative stress, and inflammation) promote retinal vascular cell and neuronal injury in patients with DM. We focus on how these processes influence, and are influenced by, genes regulated by the HIF family of transcription factors in glial, vascular, neuronal, and inflammatory cells, with the goal of identifying new therapeutic avenues for the prevention or early treatment of patients with this vision-threating disease.
Authors
Chuanyu Guo, Akrit Sodhi
No posts were found with this tag.