Commentary
Abstract
Organized adaptive immunity can emerge in the CNS under specific inflammatory and stromal conditions. The study by Yang et al. in this issue of the JCI reports that experimental ischemic stroke induced germinal center–like B cell follicles through microglial MIF–CD74/CXCR4 signaling and in situ B cell proliferation, promoting chronic neuroinflammation. These findings align with a growing body of evidence that the brain and meninges can support ectopic lymphoid structures in multiple sclerosis, during aging, and in certain gliomas. This Commentary integrates these observations to highlight shared principles, disease-specific outcomes, and unresolved questions regarding the identity and function of lymphoid aggregates in the CNS.
Authors
Catalina Lee-Chang
Safeguarding lymphatic identity: cooperative Erg and Fli1 activity in lymphatic vascular homeostasis
Abstract
Although transcriptional programs driving lymphatic endothelial cell (LEC) specification are being increasingly characterized, far less is known about the postnatal mechanisms that preserve lymphatic vessel identity and function. In this issue of the JCI, Yang et al. show that the E26 transformation-specific (ETS) transcription factors ETS-related gene (Erg) and Friend leukemia integration 1 (Fli1) cooperatively maintain adult LEC homeostasis by sustaining transcriptionally distinct LEC populations, vascular integrity, immune-vascular interactions, and repression of proinflammatory and prothrombotic gene programs. These findings extend the known roles of Erg and Fli1 beyond the blood endothelium and provide mechanistic insight into human lymphatic disease associated with Erg haploinsufficiency.
Authors
Kelly de Korodi, Tatiana V. Petrova
Abstract
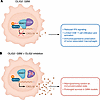
Immunotherapy has shown limited efficacy in glioblastoma (GBM), reflecting profound immune evasion and an immunosuppressive microenvironment. In this Commentary, we highlight recent work by Zhang and colleagues identifying the transcription factor OLIG2 as a central mediator of immune evasion in GBM. Though OLIG2 has an established role in promoting GBM progression through its effects on glioma stem-like cells (GSCs), Zhang et al. demonstrated a further role for OLIG2 in suppressing antitumor immunity: in human GSCs and GSCs from mouse models of GBM, OLIG2 expression epigenetically repressed the interferon-responsive chemokine CXCL10, thereby limiting cytotoxic T cell infiltration. These findings provide a mechanistic explanation for immune resistance in GBM and support targeting tumor-intrinsic chromatin programs to enhance responses to immunotherapy.
Authors
Raymond Sun, Chao Gao, Rongze Olivia Lu
Abstract
Chronic stress triggers a range of physiological responses that could dysregulate the immune system and metabolic processes, thereby increasing susceptibility to various diseases. In this issue of the JCI, Wu et al. identified a metabolic bridge between chronic stress and liver cancer progression. Chronic stress–induced glucocorticoids promoted aminopeptidase N (ANPEP) expression and subsequent reprogramming of amino acid metabolism, leading to increased liver cancer growth and metastasis. ANPEP facilitated stabilization of the cystine-glutamate transporter system Xc– and increased l-cystine influx, thereby enhancing cellular antioxidant capacity to prevent ferroptosis. Silencing ANPEP in combination with sorafenib treatment showed a synergistic inhibitory effect on liver cancer progression. These findings uncover ANPEP as a valuable target for therapeutic interventions to treat patients with liver cancer experiencing chronic stress.
Authors
Maowu Luo, Weibo Luo
Abstract
Germline variants in the gene encoding succinate dehydrogenase subunit B (SDHB) occur in around 10% of all patients with pheochromocytomas and paragangliomas (PPGLs). Diagnosis of these variants has profound implications not only for the patient but also their first-degree relatives in terms of risk for PPGLs and other SDHB-associated tumors (renal cell cancer and gastrointestinal stromal tumors). Appropriate surveillance of SDHB variant carriers is associated with reduced mortality from these cancers. Curation of disease-causing (pathogenic) variants from benign variants is therefore crucial; however, this task is often difficult for missense variants when their impact on biological function is unclear. In this issue of the JCI, Lee et al. have described a newly developed cellular complementation assay for SDHB function that may assist variant curation in clinical practice and thereby improve outcomes for patients inheriting these cancer-risk variants.
Authors
Roderick Clifton-Bligh
Abstract
Comparative biology approaches have produced foundational discoveries in the mechanisms underlying thrombosis and hemostasis. In this issue of the JCI, work by Dahlgren and colleagues continues in this tradition using an approach that integrated a multispecies investigation of conserved function with genomic exploration and discovery. Dahlgren et al. describe the identification of pathogenic variants in the ER-associated degradation pathway protein SEL1L in a rare platelet disorder affecting horses. After establishing a conserved role for SEL1L in zebrafish, mouse, and human platelet function, the study found evidence for SEL1L variants in association with bleeding phenotypes in human GWAS. Altogether, the findings elucidate a previously unrecognized component of platelet function, laying the groundwork for mechanistic explanation of a subset of human bleeding phenotypes and providing a powerful endorsement of integrative, collaborative research.
Authors
Caitlin D. Schneider, James P. Luyendyk
Abstract
Checkpoint inhibitor–associated autoimmune diabetes (CIADM) is a life-altering and potentially life-threatening complication of immune checkpoint inhibitor (ICI) treatment in patients with cancer. Risk factors and predictors of this complication remain largely unknown. In this issue of the JCI, Wu et al. examined serum and PBMCs from 14 ICI-treated patients who developed CIADM and 28 matched controls. They identified several variables that were present prior to ICI treatment, including reduced pancreatic volume, islet autoantibodies, and biomarkers indicating immune cell activation, that together are highly predictive of development of CIADM. These findings could have profound clinical implications including treatment decisions, monitoring, and potential future prevention strategies.
Authors
Kevan C. Herold, Ana Luisa Perdigoto
Abstract
The fingertip is one of the only known complex structures in mammals that can fully regenerate following amputation. This phenomenon can be studied in mice using the amputation of the digit tip, the regenerative success of which has been shown to be reliant on effective bone clearance prior to new bone formation. In this issue of the JCI, Vishlaghi et al. investigated whether local lymphatic vessels are involved in this process. Interestingly, they found that inhibiting lymphangiogenesis resulted in accelerated clearance of damaged tissue and bone, thereby improving subsequent digit regeneration. This study is the first to our knowledge to report lymphatic involvement in digit regeneration and raises questions regarding the underlying mechanisms at play.
Authors
Matthijs Luxen, Francesca Lazzeri-Barcelo, Ralf H. Adams
Abstract
The retinoid chromophore 11-cis-retinal triggers an intracellular cascade known as phototransduction that converts light into electrochemical signals. Enzymatic regeneration of 11-cis-retinal sustains vision, prevents the buildup of toxic byproducts, and is supported largely by the retinal pigmented epithelium. Directly visualizing rapidly changing retinoid intermediates in patients with inherited retinal diseases (IRDs) could provide essential therapeutic insights. In this issue, Engfer et al. introduced a groundbreaking strategy using the mouse retina as a genetically malleable model for the mammalian eye. Using cell-specific expression of lecithin:retinol acyltransferase to trap mobile retinols, they mapped the availability of 11-cis- and all-trans-retinoids within different retinal compartments under normal and diseased conditions. Their findings elucidate retinoid distribution in the retina and highlight important differences between mouse and human Müller glia. Here, we contextualize these advances within decades of research defining the visual cycle and retinoid biology, outlining the profound implications for therapeutic development for IRDs.
Authors
Ala Moshiri, Akrit Sodhi
Abstract
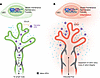
Cardiac allograft vasculopathy (CAV) is a fibroproliferative form of transplant rejection with limited treatment options other than retransplantation. In this issue, See and colleagues examined human explanted allografts with CAV. They found that a high proportion of intragraft plasma cells produce antibodies that recognize the heme catabolic end product, bilirubin. Clonotypic profiling revealed that bilirubin-reactive antibody-producing plasma cells develop from graft-infiltrating innate-like B cells, a subset often characterized by their rapid production of polyreactive natural antibodies as an early defense against infection. CAV but not nonrejecting graft tissue contained bilirubin deposits along with macrophages that expressed genes involved in heme catabolism. These findings raise the intriguing possibility that graft-derived bilirubin-specific antibodies target local heme catabolism to promote CAV.
Authors
Fuyi Liao, Andrew E. Gelman
No posts were found with this tag.



Copyright © 2026 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)