Nephrology
Abstract
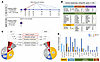
BACKGROUND. Anti-nephrin autoantibodies have emerged as a putative pathogenic driver in a subset of patients with podocytopathies, including those with post-transplant disease recurrence. METHODS. We measured anti-nephrin autoantibodies in a cohort of 65 patients with podocytopathy associated with steroid-sensitive nephrotic syndrome (n = 39) and steroid-resistant nephrotic syndrome (n = 26), and in 34 patients with post-transplant podocytopathy recurrence. Fourteen patients with membranous nephropathy and 20 healthy volunteers served as controls. ELISA and immunoprecipitation assays were performed to detect anti-nephrin IgG using two different recombinant human nephrin proteins. Immunofluorescence analysis was performed to assess the deposition of IgG and their colocalization with nephrin in renal biopsies. RESULTS. When using murine antigen-based ELISA, the highest positivity was found in healthy volunteers (55%), correlating with levels of circulating natural anti-α-galactose-α-1,3-galactose antibodies. This cross-reactivity was abrogated with recombinant human nephrin expressed in human cells. In this setting, very low prevalence (<5%) of anti-nephrin antibody-positive patients was found in steroid-sensitive and steroid-resistant nephrotic syndrome cohorts and in patients with post-transplant disease recurrence. These frequencies were comparable to healthy volunteers. Using confocal and super-resolution microscopy, only trace amounts of IgM, but no IgG, were found in the glomeruli of analyzed biopsies, which did not colocalize with nephrin. CONCLUSIONS. With the methodology presented here, anti-nephrin reactivity was extremely rare and occurred at comparably low frequencies in healthy controls, native-kidney podocytopathies, and post-transplant disease recurrence. This suggests that these autoantibodies are not inherently disease-specific and may not serve as a broad biomarker across podocytopathies. TRIAL REGISTRATION. ClinicalTrials.gov NCT06334692. FUNDING. Private donation.
Authors
Francesco Pecoraro, Luca Perico, Federica Casiraghi, Paola Rizzo, Matias Trillini, Andrea Angeletti, Manuel Alfredo Podestà, Xhuliana Kajana, Agnese Spennacchio, Marta Todeschini, Marilena Mister, Giuseppe Castellano, Ariela Benigni, Giuseppe Remuzzi
Abstract
Sphingosine-1-phosphate lyase (SPL) insufficiency syndrome (SPLIS) or nephrotic syndrome type 14 (NPHS14), is an autosomal recessive multisystem disorder caused by loss-of-function mutations in SGPL1, encoding the enzyme responsible for the terminal degradation of sphingosine-1-phosphate (S1P). We investigated a patient carrying a previously undescribed c.1084T>A (p.Ser362Thr) SGPL1 variant and analyzed the metabolic and cellular consequences of SPL deficiency using patient fibroblasts, SGPL1-knockout HEK293T cells, and Sgpl1–/– and Sgpl1rosa+fl/fl mice. Metabolic stable isotope labelling revealed that SPL deficiency does not invariably result in S1P accumulation. Instead, SPL-deficient cells maintain near-normal S1P levels through (i) feedback regulation of de novo sphingolipid synthesis via the ORMDL–ceramide axis and (ii) increased diversion of excess ceramides into glycosphingolipids. However, perturbation of sphingolipid homeostasis — either by exogenous sphingolipid load or disruption of compensatory regulation — induces pathological intracellular S1P accumulation. In vivo, Sgpl1–/– mice exhibited pronounced urinary S1P excretion and renal S1P enrichment, accompanied by cytoskeletal disorganization and impaired epithelial morphogenesis. Mechanistically, we identify aberrant Rho–ROCK signaling as a key mediator of S1P-driven cytoskeletal dysregulation. Pharmacological ROCK inhibition with Fasudil mitigated renal cytoskeletal defects in Sgpl1–/– and Sgpl1rosa+fl/fl mice and partially restored epithelial architecture. These findings redefine the metabolic consequences of SPL deficiency and identify S1P-driven Rho–ROCK hyperactivation as a tractable therapeutic target in SPLIS.
Authors
Adam Majcher, Ranjha Khan, Kathrin Buder, Florence Bourquin, Julie D. Saba, Thorsten Hornemann
Abstract
Repetitive injuries are an important trigger of progressive fibrosis. To study if repetitive injuries induce an accelerated profibrotic process, also called “fibrosis-memory,” we established an experimental system with two consecutive, clearly separated insults in a model of renal fibrosis with reversible and irreversible unilateral ureteral obstruction. We found that a preceding fibrotic event of one kidney markedly enhanced subsequent development of fibrosis in the contralateral kidney. Aggravation of fibrosis during the second insult was dependent on memory CD4+ T cells. T cell depletion abrogated the fibrosis-memory effect, while adoptive transfer of memory T cells from fibrotic mice enhanced fibrosis in the recipients. Moreover, IL-3 production by memory CD4+ T cells was essential for aggravation of fibrosis in memory situations. In patients with systemic sclerosis, IL-3 expression by T cells was markedly increased, especially after a long disease duration accompanied by involvement of internal organs. In summary, our data identify IL-3–mediated fibrosis-memory as an important driver of progressive fibrosis.
Authors
Simone Buchtler, Antje Frühauf, Sophia Neumayer, Kathrin Schmidbauer, Yvonne Talke, Frederike Winter-Köhler, Saidou Balam, Karin Landgraf, Claudia Gebhard, Michael Rehli, Florian Volker Schlieckau, Maria Beck, Florian Günther, Martin Fleck, Kerstin Renner, Matthias Mack
Abstract
BACKGROUND Kidney stone disease (KSD) affects approximately 10% of the population. While genetic factors are known to play a role in KSD, determining the clinical relevance of rare variants in KSD genes identified in adults remains challenging.METHODS The Swiss Kidney Stone Cohort is a multicenter longitudinal, observational study consisting of kidney stone formers (KSFs) (n = 701) and non-kidney stone formers (NKSFs) (n = 200). Blood and urine samples were collected at enrollment and over 3 years for deep biochemical phenotyping. Results were correlated with rare genetic variants in established KSD genes identified through whole-exome sequencing and classified according to American College of Medical Genetics and Genomics and the Association of Molecular Pathology (ACMG/AMP) criteria.RESULTS Collectively, we found rare (likely) pathogenic (LP/P) variants representing strong KSD risk factors in 6.8% of KSFs, predominantly in genes involved in renal phosphate handling and cystinuria. Detailed biochemical analyses confirmed that KSFs carrying heterozygous LP/P SLC34A3 variants exhibited significant hyperphosphaturia. In contrast, monoallelic LP/P variants in SLC34A1, SLC9A3R1, or CYP24A1, which were also frequent in NKSFs, did not result in the expected biochemical alterations, calling into question their causative role as strong KSD risk factors. In cystinuria, monoallelic SLC7A9 variants represented intermediate risk factors, since they caused biochemical alterations but required additional factors for KSD occurrence, based on frequent LP/P variants in NKSFs. The presence of strong risk factors was associated with higher kidney stone (KS) recurrence over the 3-year observation period, supporting a predictive value for genetic testing.CONCLUSIONS Correlation of genetic findings with thorough biochemical phenotyping and comparison with NKSFs redefines the clinical relevance of variants in KSD genes and has prognostic value.
Authors
Johannes Münch, Jana Petrovska, Joana Figueiro-Silva, Isabel Rubio-Aliaga, Elena M. Cabello, Ivan Ivanovski, Michael Papik, Beatrice Oneda, Daniel G. Fuster, Harald Seeger, Thomas Ernandez, Florian Buchkremer, Gregoire Wuerzner, Nasser A. Dhayat, Alexander Ritter, Stephan Segerer, Beat Roth, Anita Rauch, Pietro Manuel Ferraro, Olivier Bonny, Carsten A. Wagner, Ruxandra Bachmann-Gagescu
Abstract
Background Youth with type 2 diabetes (T2D) and severe obesity face high risk of diabetic kidney disease, which metabolic bariatric surgery (MBS) can mitigate. This study explores structural and molecular changes in kidneys after vertical sleeve gastrectomy (VSG), a form of MBS. Methods Paired analyses, including metabolic profiling, kidney volume assessment, histological evaluation, and single-cell RNA sequencing (scRNAseq) on kidney biopsies from five youth with T2D and obesity pre- and 12 months post-VSG in the IMPROVE-T2D (Impact of Metabolic surgery on Pancreatic, Renal and cardiOVascular hEalth in youth with T2D) cohort. Circulating proteomics with kidney transcriptomics, were linked using data from an independent cohort of youth with obesity, with or without T2D, undergoing MBS in Teen-Longitudinal Assessment of Bariatric Surgery (Teen-LABS, n=64). Results Post-VSG, participants lost weight and had improvements in insulin sensitivity and metabolic parameters. Kidney changes included reduced renal hyperfiltration, total kidney volume, mesangial matrix area, and microalbuminuria. scRNAseq in proximal tubule (PT) and thick ascending limb cells indicated repression of glycolysis, gluconeogenesis, and tricarboxylic acid cycle genes, with upregulation of AMP-activated protein kinase (AMPK) and Forkhead box O3 (FOXO3). Decreased metabolic signaling aligned with reduced ribosomal phosphorylated S6K (pS6K), suggesting attenuated mTORC1 activity. JAK-STAT pathway activation in PT was diminished, correlating with lower circulating ligands from Teen-LABS proteomic data. Conclusion MBS/VSG prompts kidney molecular adaptations, providing potential targets for non-surgical interventions against obesity- and diabetes-associated kidney disease.
Authors
Abhijit S. Naik, Fadhl M. Alakwaa, Viji Nair, Phillip J. McCown, Jennifer A. Schaub, Edgar A. Otto, Rajasree Menon, Francesca Annese, Ye Ji Choi, Hailey E. Hampson, Thomas H. Inge, John Hartman, Sean Eddy, Cathy Smith, Jeffrey B. Hodgin, Ken Inoki, Swayam Prakash Srivastava, Kareem Al-Fagih, Shota Yoshida, Jesse A. Goodrich, Melanie G. Cree, Phoom Narongkiatikhun, Long Yuan, Kalie L. Tommerdahl, Pottumarthi Prasad, Daniël H. van Raalte, Megan M. Kelsey, Justin R. Ryder, Tyler J. Dobbs, Patricia Ladd, Subramaniam Pennathur, Robert G. Nelson, Yusuke Okabayashi, Victor G. Puelles, Jenna Ferrence-Salo, Jeffrey A. Beamish, Frank C. Brosius, Kristen J. Nadeau, Laura Pyle, Matthias Kretzler, Petter Bjornstad
Abstract
The urokinase plasminogen activator receptor (uPAR) is a membrane-bound protein found on the surface of immune cells. Through the action of proteases, uPAR is cleaved to produce several circulating proteins in the bloodstream, including the soluble form suPAR and the fragments D1 and D2D3. Initially studied in the context of infectious diseases and cancer, recent research has revealed roles for suPAR and its related proteins as mediators linking innate immunity to the pathogenesis of kidney and cardiovascular diseases, as well as insulin-dependent diabetes. While these proteins have long been recognized as prognostic biomarkers, growing clinical, experimental, and genetic evidence highlights their active involvement in the onset and progression of these diverse conditions. This Review examines suPAR’s evolution from its discovery as a modulator of innate immunity to its current status as a key driver in chronic kidney and cardiovascular diseases. Furthermore, we explore the molecular mechanisms through which suPAR and D2D3 contribute to multiorgan damage, emphasizing emerging opportunities for therapeutic interventions across interconnected organ systems.
Authors
Jochen Reiser, Salim S. Hayek, Sanja Sever
Abstract
Authors
Dalin Zhang, Chun-Lung Chiu, Fernando Jose Garcia Marques, Abel Bermudez, Christian R. Hoerner, Nicholas Hadi, Elise Wang, Thomas J. Metzner, Ludimila Trabanino, John T. Leppert, Hongjuan Zhao, Robert Tibshirani, Alice C. Fan, Sharon J. Pitteri, James D. Brooks
Abstract
Deposits of hydroxyapatite called Randall's plaques are found in the renal papilla of calcium oxalate kidney stone formers and likely serve as the nidus for stone formation, but their pathogenesis is unknown. Claudin-2 is a paracellular ion channel that mediates calcium reabsorption in the renal proximal tubule. To investigate the role of renal claudin-2, we generated kidney tubule-specific claudin-2 conditional knockout mice (KS-Cldn2 KO). KS-Cldn2 KO mice exhibited transient hypercalciuria in early life. Normalization of urine calcium was accompanied by a compensatory increase in expression and function of renal tubule calcium transporters, including in the thick ascending limb. Despite normocalciuria, KS-Cldn2 KO mice developed papillary hydroxyapatite deposits, beginning at 6 months of age, that resembled Randall's plaques and tubule plugs. Bulk chemical tissue analysis and laser ablation-inductively coupled plasma mass spectrometry revealed a gradient of intrarenal calcium concentration along the corticomedullary axis in normal mice, that was accentuated in KS-Cldn2 KO mice. Our findings provide evidence for the “vas washdown” hypothesis for Randall's plaque formation, and identify the corticomedullary calcium gradient as a target for therapies to prevent kidney stone disease.
Authors
Christine V. Behm, Duuamene Nyimanu, Ony Araujo Galdino, Sadhana Kanoo, Young Chul Kim, Natalia Lopez, Helen Goodluck, Peter S. Rowe, Andrew P. Evan, André J. Sommer, Matthew N. Barr, Tracy Punshon, Volker Vallon, Brian P. Jackson, James C. Williams Jr., Alan S.L. Yu
Abstract
Clinically, blockade of renal glucose resorption by sodium–glucose cotransporter 2 (SGLT2) inhibitors slows progression of kidney disease, yet the underlying mechanisms are not fully understood. We hypothesized that altered renal metabolites underlie observed kidney protection when SGLT2 function is lost. S-adenosylmethionine (SAM) levels were increased in kidneys from mice lacking SGLT2 function on a diabetogenic high-fat diet (SPHFD) compared with WT mice fed HFD. Elevated SAM in SPHFD was associated with improved kidney function and decreased expression of NF-κB pathway–related genes. Injured proximal tubular cells that emerged under HFD conditions in WT mice and humans consistently showed reduction in expression of the SAM synthetase Mat2a/MAT2A, while MAT2A inhibition, which reduces SAM production, abrogated kidney protection in SPHFD mice. Histone H3 lysine 27 (H3K27) repressive trimethylation of NF-κB–related genes was increased in SPHFD, consistent with SAM’s role as a methyl donor. Our data support a model whereby SGLT2 loss enhances SAM levels within the kidney, leading to epigenetic repression of inflammatory genes and kidney protection under metabolic stress.
Authors
Hiroshi Maekawa, Yalu Zhou, Yuki Aoi, Margaret E. Fain, Dorian S. Kaminski, Hyewon Kong, Zachary L. Sebo, Ram P. Chakrabarty, Benjamin C. Howard, Grant Andersen, Biliana Marcheva, Peng Gao, Pinelopi Kapitsinou, Joseph Bass, Ali Shilatifard, Navdeep S. Chandel, Susan E. Quaggin
Abstract
The role of endothelial dysfunction in tubulointerstitial fibrosis associated with chronic kidney disease (CKD) is not well understood. In this study, we demonstrate that the activation of the endothelial tyrosine kinase TIE2 alleviates renal pathology in experimental CKD in mice. TIE2 activation was achieved using a human angiopoietin-2 (ANGPT2)-binding and TIE2-activating antibody (ABTAA), or through adult-induced endothelial-specific knockout of the vascular endothelial protein tyrosine phosphatase gene (Veptp). Both methods significantly protected CKD mice from endothelial dysfunction, peritubular capillary loss, tubular epithelial injury, and tubulointerstitial fibrosis. Conversely, silencing TIE2 through adult-induced endothelial-specific knockout of the Tie2 gene exacerbated CKD pathology. Additionally, we found that endothelial dysfunction promotes renal fibrosis not through endothelial-to-mesenchymal transition as previously expected, but by inducing the expression of pro-fibrotic PDGFB in tubular epithelial cells, a process that is inhibited by TIE2 activation. Our findings suggest that TIE2 activation via ABTAA warrants investigation as a therapy in human CKD, where there is a substantial unmet medical need.
Authors
Riikka Pietilä, Amanda M. Marks-Hultström, Liqun He, Sami Nanavazadeh, Susan E. Quaggin, Christer Betsholtz, Marie Jeansson



Copyright © 2026 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)