Review
Abstract
Bone is a highly dynamic and purposefully organized structure that remodels constantly throughout adult life. Disordered bone remodeling, in which resorption of old bone by osteoclasts exceeds new bone formation by osteoblasts, results in bone loss, which, in turn, is associated with debilitating conditions, including osteoporosis and metastatic bone disease. The past decade has revealed vital new insights into the role of the central nervous system in skeletal regulation. These studies have led to a better understanding of physiologic circuitry, enabled us to revisit disease pathophysiology, and in doing so, prompted the creation of candidate therapeutics. The central neural control of bone is exerted through two arms — an amplitude-modulated (AM) neurohormonal arm that relies on changes in circulating levels of anterior and posterior pituitary hormones, which act on bone directly, and a frequency-modulated (FM) arm that arises from changes in the firing frequency of sympathetic, parasympathetic, and sensory nerves that innervate bone. Here, we review the medical consequences arising from the dysfunction of the AM and FM arms, as well as studies that have unmasked promising therapeutic targets.
Authors
Mone Zaidi, Se-Min Kim, Vitaly Ryu, Daria Lizneva, Terry F. Davies, Clifford J. Rosen, Tony Yuen, Andrea Giustina
Abstract
Although combination antiretroviral therapy (ART) has dramatically reduced the incidence of severe HIV-associated neurological disease, the central nervous system (CNS) remains a viral sanctuary in which inflammation and brain injury persist despite systemic viral suppression. Here, we synthesize evidence that ongoing HIV-associated brain injury is sustained not primarily by unchecked viral replication but by persistent viral transcription from defective proviruses, immune-mediated synaptic dysfunction driven by bystander activation, and long-lived microglial reprogramming shaped by epigenetic “training.” We highlight how emerging single-cell multiomics and “liquid biopsy” approaches are redefining our understanding of the CNS reservoir at high resolution. We further discuss the growing emphasis on biologically anchored, molecularly defined disease subtypes as a means to disentangle HIV-specific pathology from the confounding overlap of aging and multimorbidity, which have increased in the ART era. Finally, we underscore the necessity of human-centered translational studies to validate preclinical findings, outlining how these molecular insights pave the way for precision therapeutics and CNS-targeted cure strategies.
Authors
Paraskevas Filippidis, Shelli F. Farhadian
Abstract
Urothelial cancers of the urinary tract are the fourth most common malignancy in men, with a shifting demographic affecting younger patients and an increasing incidence in females. In this Review, we discuss recent discoveries and paradigm-shifting clinical trials that impact all stages of urothelial cancer. New therapeutics and drug-delivery devices have led to multiple approvals for treatments of non-muscle invasive bladder cancer. The addition of chemotherapy, immunotherapy, and antibody-drug conjugates is transforming perioperative treatment for patients with muscle-invasive bladder cancer. The use of liquid biomarkers, circulating tumor DNA, and urinary tumor DNA is aiding the identification of patients at risk for local recurrence and possibly those who can avoid systemic therapy. Finally, integrating biomarkers and systemic treatments is creating a paradigm that could lead to the successful treatment of bladder cancer without requiring bladder removal. Overall, these advancements in biomarkers and novel therapeutics are likely to dramatically improve survival for bladder cancer.
Authors
Joshua J. Meeks
Abstract
Diabetic retinopathy (DR), the most common microvascular complication in patients with diabetes mellitus (DM), is a leading cause of vision loss worldwide. Sustained hyperglycemia plays a central role in promoting DR. However, tight glycemic control does not prevent — and indeed sometimes worsens — DR, highlighting the importance of ongoing studies aimed at improving our understanding of this complex disease. Over the last few decades, the dogma that DR is a vascular disease that results in secondary neuronal injury has evolved, as emerging evidence suggests that neurodegeneration occurs in parallel with or prior to vascular cell injury in the retina of patients with DM. This has led to appreciation of DR as a neurovascular disease, characterized by microvascular injury and neurodegeneration, both of which contribute to vision loss. Here, we explore how molecular stress (i.e., glucose dysregulation, dysmetabolism, oxidative stress, and inflammation) promote retinal vascular cell and neuronal injury in patients with DM. We focus on how these processes influence, and are influenced by, genes regulated by the HIF family of transcription factors in glial, vascular, neuronal, and inflammatory cells, with the goal of identifying new therapeutic avenues for the prevention or early treatment of patients with this vision-threating disease.
Authors
Chuanyu Guo, Akrit Sodhi
Abstract
Circadian clocks govern daily rhythms in cellular and physiological processes, including cell cycle, DNA repair, metabolism, and immune function, that influence cancer development and treatment response. Disruption of circadian regulators either promotes or suppresses malignancy depending on tumor type and biological context. This duality likely reflects systemic rewiring of circadian physiology and direct interactions between clock components and oncogenic pathways. These insights hold clinical relevance for the field of chronotherapy, which seeks to enhance therapeutic efficacy and minimize toxicity by aligning drug administration with circadian rhythms or by targeting elements of the molecular clock. In this Review, we highlight the promise of integrating circadian biology into precision oncology and underscore the importance of cancer type–specific investigations to harness the full therapeutic potential of chronotherapy in cancer.
Authors
Rebecca M. Mello, Selma Masri, Katja A. Lamia
Abstract
Metastatic hormone-sensitive prostate cancer (mHSPC) is a clinically and molecularly heterogeneous disease. Recent insights into the biology underlying disease presentation, volume of disease, and response to therapies are starting to point toward biomarkers to improve selection for intensified and deintensified treatment strategies. In addition, the therapeutic landscape is rapidly changing, with new biomarker-driven studies targeting genotype (e.g., BRCA or PTEN mutant) and phenotype (e.g., prostate-specific membrane antigen status) in development for mHSPC. A better understanding of tumor heterogeneity, clonal evolution, and metastatic homing in prostate cancer will hopefully inform future strategies for local and systemic disease control, personalized monitoring strategies, and improved patient outcomes.
Authors
Alice Bernard-Tessier, Himisha Beltran
Abstract
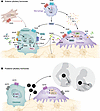
Cells release extracellular vesicles (EVs) with cargo that originates from distinct subcellular compartments, including the nucleus, cytoplasm, and plasma membrane. Given their diverse cargo, EVs play multiple roles in physiology and pathology, including in immune dysregulation and autoimmune pathogenesis. For example, EVs can act as autoantigens by transporting immunogenic molecules from the nucleus or cytoplasm, whereas EVs carrying membrane-bound MHCs from antigen-presenting cells can activate adaptive immunity by presenting self-antigens to T cells. EV-associated cytoplasmic peptidases or proteasomes contribute to immune regulation by modulating antigen processing and presentation. Moreover, EVs also drive inflammatory responses by shuttling a variety of proinflammatory molecules that sustain autoimmune responses. Intriguingly, emerging evidence indicates that EVs might contribute to autoimmune surveillance by activating cytosolic surveillance sensors, modulating immune checkpoints, regulating NK/T cell cytotoxicity, and altering macrophage and DC phagocytosis, representing an exciting and underexplored frontier in autoimmune research. By tackling critical knowledge gaps, this Review explores the emerging roles of EVs and their diverse cargo in driving autoimmune diseases, suggesting new perspectives on their potential as innovative therapeutic targets.
Authors
Yin Zhao, Xing Lyu, Xiuhua Wu, Yu Liu, Na Zhang, Wei Wei, Ming-Lin Liu
Abstract
Advances in cancer therapy have greatly extended patient survival but have also introduced a growing burden of cardiovascular toxicity that threatens long-term outcomes. These toxicities encompass a broad and often unpredictable range of clinical presentations, complicating oncologic care. Understanding how chemotherapy, targeted agents, and immune modulators impair cardiovascular function is essential for early detection, prevention, and management. Emerging insights into the cellular and molecular mechanisms, ranging from immune activation to transcriptional reprogramming and disrupted intercellular communication, underscore the complexity of cancer therapy–induced cardiac injury. Unraveling these mechanisms will be key to developing personalized, mechanism-based strategies that preserve cardiac function without compromising anticancer efficacy. As survivorship continues to improve, mitigating cardiotoxicity remains a critical priority for preserving both the quality and duration of life of patients.
Authors
Giulia Guerra, Marco Mergiotti, Hossein Ardehali, Emilio Hirsch, Alessandra Ghigo
Abstract
Connections between the digestive system and the brain have been postulated for over 2000 years. Despite this, only recently have specific mechanisms of gut-brain interaction been identified. Due in large part to increased interest in the microbiome, the wide use of incretin-based therapies (i.e., glucagon-like peptide 1 [GLP-1] receptor agonists), technological advancements, increased understanding of neuroimmunology, and the identification of a direct enteroendocrine cell–neural circuit, research in the past 10 years has made it abundantly clear that the gut-brain connection plays a role both in clinical disease as well as the actions of therapeutics. In this Review, we describe mechanisms by which the gut and brain communicate and highlight human and animal studies that implicate changes in gut-brain communication in disease states in gastroenterology, neurology, psychiatry, and endocrinology. Furthermore, we define how GLP-1 receptor agonists for obesity and guanylyl cyclase C agonists for irritable bowel syndrome leverage gut-brain mechanisms to improve patient outcomes. This Review illustrates the critical nature of gut-brain communication in human disease and the potential to target gut-brain pathways for therapeutic benefit.
Authors
Zachary S. Lorsch, Rodger A. Liddle
Abstract
The urokinase plasminogen activator receptor (uPAR) is a membrane-bound protein found on the surface of immune cells. Through the action of proteases, uPAR is cleaved to produce several circulating proteins in the bloodstream, including the soluble form suPAR and the fragments D1 and D2D3. Initially studied in the context of infectious diseases and cancer, recent research has revealed roles for suPAR and its related proteins as mediators linking innate immunity to the pathogenesis of kidney and cardiovascular diseases, as well as insulin-dependent diabetes. While these proteins have long been recognized as prognostic biomarkers, growing clinical, experimental, and genetic evidence highlights their active involvement in the onset and progression of these diverse conditions. This Review examines suPAR’s evolution from its discovery as a modulator of innate immunity to its current status as a key driver in chronic kidney and cardiovascular diseases. Furthermore, we explore the molecular mechanisms through which suPAR and D2D3 contribute to multiorgan damage, emphasizing emerging opportunities for therapeutic interventions across interconnected organ systems.
Authors
Jochen Reiser, Salim S. Hayek, Sanja Sever
No posts were found with this tag.



Copyright © 2026 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)