Cancer Immunotherapy
Series edited by Yiping Yang
In the mid-1800s, Rudolf Virchow noted the presence of surfeit inflammatory cells in many tumors. Roughly 50 years later, Paul Ehrlich postulated that the immune system both recognizes and protects against cancer. Since then, researchers have been trying to elucidate the relationship between cancer, inflammation, and the innate and adaptive immune systems, starting with the theory of immunosurveillance introduced by Lewis Thomas and further developed by Sir MacFarlane Burnet. We now know that tumor cells display antigens that are recognized by immune cells, but that anti-tumor immunity can be circumvented directly by tumor cells themselves via a variety of escape mechanisms. The goal of cancer immunotherapy is to mount an effective anti-tumor immune response by repairing, stimulating or, enhancing the immune system’s response to cancer cells. Reviews in this series detail progress in cancer immunoediting, immunosuppressive cells in the tumor microenvironment, cancer-associated inflammation, therapeutic cancer vaccines, genomic approaches in immunotherapy, adoptive transfer of genetically engineered T cells, and checkpoint blockade therapy.
Articles in series
Abstract
The recent clinical successes of immune checkpoint blockade and chimeric antigen receptor T cell therapies represent a turning point in cancer immunotherapy. These successes also underscore the importance of understanding basic tumor immunology for successful clinical translation in treating patients with cancer. The Reviews in this Review Series focus on current developments in cancer immunotherapy, highlight recent advances in our understanding of basic aspects of tumor immunology, and suggest how these insights can lead to the development of new immunotherapeutic strategies.
Authors
Yiping Yang
Abstract
Cancer immunoediting explains the dual role by which the immune system can both suppress and/or promote tumor growth. Although cancer immunoediting was first demonstrated using mouse models of cancer, strong evidence that it occurs in human cancers is now accumulating. In particular, the importance of CD8+ T cells in cancer immunoediting has been shown, and more broadly in those tumors with an adaptive immune resistance phenotype. This Review describes the characteristics of the adaptive immune resistance tumor microenvironment and discusses data obtained in mouse and human settings. The role of other immune cells and factors influencing the effector function of tumor-specific CD8+ T cells is covered. We also discuss the temporal occurrence of cancer immunoediting in metastases and whether it differs from immunoediting in the primary tumor of origin.
Authors
Michele W.L. Teng, Jerome Galon, Wolf-Herman Fridman, Mark J. Smyth
Abstract
Cancer development and its response to therapy are strongly influenced by innate and adaptive immunity, which either promote or attenuate tumorigenesis and can have opposing effects on therapeutic outcome. Chronic inflammation promotes tumor development, progression, and metastatic dissemination, as well as treatment resistance. However, cancer development and malignant progression are also associated with accumulation of genetic alterations and loss of normal regulatory processes, which cause expression of tumor-specific antigens and tumor-associated antigens (TAAs) that can activate antitumor immune responses. Although signals that trigger acute inflammatory reactions often stimulate dendritic cell maturation and antigen presentation, chronic inflammation can be immunosuppressive. This antagonism between inflammation and immunity also affects the outcome of cancer treatment and needs to be considered when designing new therapeutic approaches.
Authors
Shabnam Shalapour, Michael Karin
Abstract
Our understanding of the role of myeloid-derived suppressor cells (MDSCs) in cancer is becoming increasingly complex. In addition to their eponymous role in suppressing immune responses, they directly support tumor growth, differentiation, and metastasis in a number of ways that are only now beginning to be appreciated. It is because of this increasingly complex role that these cells may become an important factor in the treatment of human cancer. In this Review, we discuss the most pertinent and controversial issues of MDSC biology and their role in promoting cancer progression and highlight how these cells may be used in the clinic, both as prognostic factors and as therapeutic targets.
Authors
Douglas Marvel, Dmitry I. Gabrilovich
Abstract
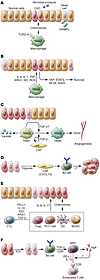
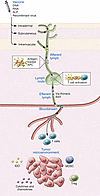
The generation of an inflammatory environment is favorable and often decisive for the growth of both primary tumors and metastases. Tumor cells either express membrane molecules or release tumor-derived soluble factors able to alter myelopoiesis. Tumor-reprogrammed myeloid cells not only create a tolerogenic environment by blocking T cell functions and proliferation, but also directly drive tumor growth by promoting cancer stemness, angiogenesis, stroma deposition, epithelial-to-mesenchymal transition, and metastasis formation. In this Review, we discuss the interplay between immunosuppressive and protumoral myeloid cells and detail their immune-regulatory mechanisms, the molecular pathways involved in their differentiation, as well as their potential role as prognostic and diagnostic biomarkers and prospective targets for innovative approaches to treat tumor-bearing hosts.
Authors
Stefano Ugel, Francesco De Sanctis, Susanna Mandruzzato, Vincenzo Bronte
Abstract
The relationship between cancer and the immune system is complex and provides unique therapeutic opportunities. Cytotoxic T lymphocyte antigen-4 (CTLA-4) is a regulatory molecule that suppresses T cell effector function following initial activation by costimulatory signals. Fully human monoclonal antibodies targeting CTLA-4 have been shown to increase T cell function and antitumor responses in patients with advanced metastatic melanoma. Responses observed with such immune checkpoint therapy can follow a different pattern from that seen with cytotoxic chemotherapy or targeted therapy and may continue after therapy is discontinued. In addition, the toxicities that are associated with anti–CTLA-4 therapy may differ from those of conventional therapies and consist of inflammatory events in parts of the body that do not contain cancerous cells. Early recognition of these inflammatory events and intervention is important, and the identification of predictive biomarkers continues to be an unfulfilled need in the field of immunotherapy. Combinatorial approaches with targeted therapies, radiation therapy, chemotherapy, or other immune checkpoint agonists/antagonists have the potential to increase the efficacy of CTLA-4 blockade.
Authors
Elizabeth Buchbinder, F. Stephen Hodi
Abstract
Major progress has been made toward our understanding of the programmed death-1/programmed death ligand-1 (PD-1/PD-L1) pathway (referred to as the PD pathway). mAbs are already being used to block the PD pathway to treat human cancers (anti-PD therapy), especially advanced solid tumors. This therapy is based on principles that were discovered through basic research more than a decade ago, but the great potential of this pathway to treat a broad spectrum of advanced human cancers is just now becoming apparent. In this Review, we will briefly review the history and development of anti-PD therapy, from the original benchwork to the most up-to-date clinical results. We will then focus the discussion on three basic principles that define this unique therapeutic approach and highlight how anti-PD therapy is distinct from other immunotherapeutic approaches, namely tumor site immune modulation, targeting tumor-induced immune defects, and repairing ongoing (rather than generating de novo) tumor immunity. We believe that these fundamental principles set the standard for future immunotherapies and will guide our efforts to develop more efficacious and less toxic immune therapeutics to treat human cancers.
Authors
Lieping Chen, Xue Han
Abstract
Twenty-five years after its inception, the genetic engineering of T cells is now a therapeutic modality pursued at an increasing number of medical centers. This immunotherapeutic strategy is predicated on gene transfer technology to instruct T lymphocytes to recognize and reject tumor cells. Chimeric antigen receptors (CARs) are synthetic receptors that mediate antigen recognition, T cell activation, and — in the case of second-generation CARs — costimulation to augment T cell functionality and persistence. We demonstrated over a decade ago that human T cells engineered with a CD19-specific CAR eradicated B cell malignancies in mice. Several phase I clinical trials eventually yielded dramatic results in patients with leukemia or lymphoma, especially acute lymphoblastic leukemia (ALL). This review recounts the milestones of CD19 CAR therapy and summarizes lessons learned from the CD19 paradigm.
Authors
Michel Sadelain
Abstract
The clinical benefit of therapeutic cancer vaccines has been established. Whereas regression of lesions was shown for premalignant lesions caused by HPV, clinical benefit in cancer patients was mostly noted as prolonged survival. Suboptimal vaccine design and an immunosuppressive cancer microenvironment are the root causes of the lack of cancer eradication. Effective cancer vaccines deliver concentrated antigen to both HLA class I and II molecules of DCs, promoting both CD4 and CD8 T cell responses. Optimal vaccine platforms include DNA and RNA vaccines and synthetic long peptides. Antigens of choice include mutant sequences, selected cancer testis antigens, and viral antigens. Drugs or physical treatments can mitigate the immunosuppressive cancer microenvironment and include chemotherapeutics, radiation, indoleamine 2,3-dioxygenase (IDO) inhibitors, inhibitors of T cell checkpoints, agonists of selected TNF receptor family members, and inhibitors of undesirable cytokines. The specificity of therapeutic vaccination combined with such immunomodulation offers an attractive avenue for the development of future cancer therapies.
Authors
Cornelis J.M. Melief, Thorbald van Hall, Ramon Arens, Ferry Ossendorp, Sjoerd H. van der Burg
Abstract
It is now well established that the immune system can recognize developing cancers and that therapeutic manipulation of immunity can induce tumor regression. The capacity to manifest remarkably durable responses in some patients has been ascribed in part to T cells that can (a) kill tumor cells directly, (b) orchestrate diverse antitumor immune responses, (c) manifest long-lasting memory, and (d) display remarkable specificity for tumor-derived proteins. This specificity stems from fundamental differences between cancer cells and their normal counterparts in that the former develop protein-altering mutations and undergo epigenetic and genetic alterations, resulting in aberrant protein expression. These events can result in formation of tumor antigens. The identification of mutated and aberrantly expressed self-tumor antigens has historically been time consuming and laborious. While mutant antigens are usually expressed in a tumor-specific manner, aberrantly expressed antigens are often shared between cancers and, therefore, in the past, have been the major focus of therapeutic cancer vaccines. However, advances in next-generation sequencing and epitope prediction now permit the rapid identification of mutant tumor neoantigens. This review focuses on a discussion of mutant tumor neoantigens and their use in personalizing cancer immunotherapies.
Authors
Matthew M. Gubin, Maxim N. Artyomov, Elaine R. Mardis, Robert D. Schreiber



Copyright © 2026 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)