Metabolism
Abstract
Obesity-linked steatosis is a significant risk factor for hepatocellular carcinoma (HCC); however, the molecular mechanisms underlying the transition from Metabolic dysfunction-associated steatotic liver disease (MASLD) to HCC remains unclear. We explored the role of the endoplasmic reticulum (ER)-associated protein NgBR, an essential component of the cis-prenyltransferases (cis-PTase) enzyme, in chronic liver disease. Hepatocyte-specific NgBR deletion in mice (N-LKO) intensifies triacylglycerol (TAG) accumulation, inflammatory responses, ER/oxidative stress, and fibrosis, ultimately resulting in HCC development with 100% penetrance after four months on a high-fat diet. Similarly, liver-specific knockout of DHDDS (D-LKO) NgBR’s cis-PTase partner and a knock-in model carrying a human NgBR mutation that impairs cis-PTase activity developed HCC under high-fat diet conditions, although with lower penetrance. Single cell transcriptomic atlas from affected livers provides a detailed molecular analysis of the transition from liver pathophysiology to HCC development. Mechanistically, NgBR deficiency promotes excessive hepatic TAG accumulation by enhancing lipid uptake and impairing very-low-density lipoprotein (VLDL) secretion. Importantly, pharmacological inhibition of diacylglycerol acyltransferase-2 (DGAT2), a key enzyme in TAG synthesis, abrogates diet-induced liver damage and HCC burden in N-LKO mice. Overall, our findings establish cis-PTase as a critical suppressor of MASLD-HCC conversion and suggest DGAT2 inhibition may serve as a promising therapeutic approach to delay HCC formation in advanced metabolic dysfunction-associated steatohepatitis (MASH).
Authors
Abhishek K. Singh, Balkrishna Chaube, Kathryn M. Citrin, Joseph Fowler, Sungwoon Lee, Jonatas Catarino, James Knight, Sarah C. Lowery, Sonal Shree, Keira E. Mahoney, Nabil E. Boutagy, Inmaculada Ruz-Maldonado, Kathy Harry, Marya Shanabrough, Trenton T. Ross, Stacy A. Malaker, Yajaira Suárez, Carlos Fernández-Hernando, Kariona A. Grabińska, William C. Sessa
Abstract
Pseudoxanthoma Elasticum (PXE) is a rare disease caused by loss of function of the gene Abcc6 and characterized by ectopic calcification of multiple tissues, but the physiological reasons underlying ectopic calcification in PXE remain unclear. In a murine model of Abcc6 deficient PXE where animals develop robust cardiac calcification after heart injury, we show the critical importance of the liver in mediating ectopic cardiac calcification. Tissue-specific deletion of Abcc6 in the liver, but not in the heart was sufficient to cause post-injury cardiac calcification. Metabolomics and gene expression demonstrated deficiencies in nucleotide metabolism, cellular energetics and defects in cellular respiration, underlying ectopic calcification in PXE. Functional abnormalities in cellular respiration in the injured heart were similar in globally or liver-specific Abcc6-deficient animals demonstrating that hepatic Abcc6 expression regulates cellular respiration in the injured heart. We show that ectopic calcification in PXE is primarily dystrophic and treatment with clodronate or etidronate, that prevent the growth of calcium hydroxyapatite mineralization, was sufficient to rescue the phenotype of ectopic cardiac calcification in Abcc6-deficient states. Taken together, these observations highlight the role of the liver in regulating target tissue metabolic and mitochondrial function in causing ectopic calcification in Abcc6-deficient states.
Authors
Yijie Wang, Baiming Sun, Feiyang Ma, Bo Tao, Yiqian Gu, Zhiqiang Zhou, Jason Kim, Linlin Zhang, Zhihao Liu, Johanna ten Hoeve, Linsey Stiles, Lucia Fernandez-del-Rio, Calvin Pan, Orian Shirihai, Shili Xu, Thomas G. Graeber, Tamer Sallam, Matteo Pellegrini, Aldons J. Lusis, Arjun Deb
Abstract
Stem cells are critical for the homeostasis of adult tissues. Thyroid hormone (TH), whose intracellular concentration is increased by type 2 deiodinase (D2), is involved in many functions, but its role in quiescence is unknown. Here we show that D2 marks quiescent stem cells in muscle and skin. Genetic D2-depletion in quiescent muscle stem cells triggers their transition from G0 to a GAlert–like state. This increases the proliferative potential of the stem cells, but impairs their self-renewal capacity, leading to depletion of the stem cell pool and regenerative failure over time. Mechanistically, TH sustains Notch signaling, and active Notch overexpression partially rescues D2-depletion. Transient pharmacological inhibition of D2 accelerates muscle regeneration and skin wound healing by promoting stem cell expansion. In conclusion, we show that D2 is a critical metabolic enzyme in maintaining stem cell quiescence and in regulating self-renewal.
Authors
Maria Angela De Stefano, Raffaele Ambrosio, Cristina Luongo, Tommaso Porcelli, Daniela Di Girolamo, Caterina Miro, Monica Dentice, Caterina Missero, Domenico Salvatore
Abstract
The link between glutaminolysis and osteoarthritis (OA) has only recently begun to be elucidated. Here, we report the association of obesity- and injury-induced cartilage damage with impaired glutaminolysis in chondrocytes. Defective glutaminolysis triggered the onset and progression of OA, with enhanced catabolism and decreased anabolism. Supplementation of α-ketoglutarate (αKG), a key component in glutaminolysis and an epigenetic factor, effectively protected cartilage against degradation in vivo via a TCA cycle– and HIF-1α–independent manner. Mechanistically, OA pathogenic factors increased H3K27me3 deposition on promoters of key glutaminolysis genes, including Slc1a5 and Gls1, leading to impaired glutaminolysis. Conversely, αKG facilitated Kdm6b-dependent H3K27me3 demethylation of not only glutaminolysis genes to rescue Gln metabolism but also Ube2o to reverse OA. Elevated Ube2o expression led to TRAF6 ubiquitination and subsequent inhibition of NF-κB signaling, thereby reversing the pathological reprogramming of glycolysis and oxidative phosphorylation and protecting against cartilage destruction. Collectively, these results demonstrated that OA pathogenic factors impair glutaminolysis through epigenetic regulation, which further exacerbate OA. Moreover, αKG restores metabolic homeostasis and alleviates OA through H3K27me3 demethylation.
Authors
Shuaijun Li, Jiefeng Huang, Ting Shang, Laiya Lu, Orion R. Fan, Peisheng Jin, Xin Zou, Zixin Cai, Wuyan Lu, Shuangmeng Jia, Linxiao Li, Ke Fang, Fengting Niu, Jiaojiao Li, Cheng Zhao, Qian Wang, Ruizhu Sun, Si Shi, Feng Yin, Yun Zhang, Yi Eve Sun, Lei Cui
Abstract
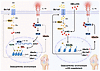
Neonatal life is marked by rapid antigen exposure, necessitating establishment of peripheral immune tolerance via conversion of naïve CD4+ T cells into regulatory T cells (Tregs). Here, we demonstrated heightened capacity for FOXP3 expression and tolerogenic function among cord blood versus adult blood naive CD4+ T cells and showed that this is linked to their unique metabolic profile and elevated expression of the NADase, CD38. Early-life naïve CD4+ T cells demonstrated a metabolic preference for glycolysis, which directly facilitated their differentiation trajectory. We revealed an age-dependent gradient in CD38 levels on naïve CD4+ T cells and showed that high CD38 expression contributes to both the glycolytic state and tolerogenic potential of neonatal CD4+ T cells, effects that were mediated at least in part via the NAD-dependent deacetylase SIRT1. Thus, the early-life window for peripheral tolerance in humans is critically enabled by the immunometabolic state of the naïve CD4+ compartment.
Authors
Laura R. Dwyer, Andrea M. DeRogatis, Sean Clancy, Victoire Gouirand, Charles Chien, Elizabeth E. Rogers, Scott P. Oltman, Laura L. Jelliffe-Pawlowski, Theo van den Broek, Femke van Wijk, Susan V. Lynch, Rachel L. Rutishauser, Allon Wagner, Alexis J. Combes, Tiffany C. Scharschmidt
Abstract
Skeletal muscle frequently experiences oxygen depletion, especially during exercise, and the alpha subunit of the hypoxia-inducible factors (HIF1α and HIF2α) plays a crucial role in mediating cellular adaptation to low oxygen levels. However, although significant, the absence of an appropriate experimental mouse model leaves the precise roles of HIFα in myofibers unclear. Therefore, this study developed mice with myofiber-specific knockouts of prolyl hydroxylase proteins (PHDs), in which HIFα is stabilized, and inducible myofiber-specific overexpression of stable HIF1α or HIF2α to explore the role of HIFα in myofibers. Using three distinct mouse models, we found that HIF1α increased the number of oxidative fibers but paradoxically impaired exercise performance and mitochondrial function. Comparatively, HIF2α exerted protection mechanisms against glucose intolerance and diet-induced obesity. Notably, HIF2α stabilization in skeletal muscle markedly elevated erythropoietin (EPO) levels in muscle and serum but not in the kidney and liver, suggesting skeletal muscle is a previously unrecognized site of EPO production in the body. Thus, this study demonstrates the distinct roles of HIF1α and HIF2α in skeletal muscle, newly uncovering that the PHD-HIF2α axis produces EPO from myofibers.
Authors
Junhyeong Lee, Merc Emil Matienzo, Sangyi Lim, Edzel Evallo, Yeongsin Kim, Sujin Jang, Keon Kim, Chang Hyeon Choi, Youn Ho Han, Chang-Min Lee, Tae-Il Jeon, Sang-Ik Park, Jun Wu, Dong-il Kim, Min-Jung Park
Abstract
Metabolic-inflammatory crosstalk orchestrates muscle repair. Although pyroptosis typically aggravates sterile injury, we demonstrated that GSDME-dependent pyroptotic signaling associated with recruited myeloid cells paradoxically supported regeneration. GSDME expression was induced in post-surgical human muscle injury and murine damage models. Gsdme deficiency delayed functional recovery and exacerbated injury-induced myosteatosis, a pathological form of intramuscular ectopic fat deposition. Time-series and single-cell RNA-sequencing analyses revealed that GSDME loss shifted the transcriptional program from oxidative metabolism toward lipid storage and adipogenesis. Lipidomics confirmed aberrant accumulation of triacylglycerols and sphingolipids in Gsdme-deficient muscle. Single-cell profiling further identified divergent fibro-adipogenic progenitors (FAPs) states skewed toward adipogenesis, accompanied by impaired expansion of restorative Lyve1⁺Cd163⁺Txnip⁺ tissue-resident macrophages (TRMs)—validated by multiplex flow cytometry. Blocking CCR2-dependent monocyte recruitment produced regenerative defects comparable to those caused by Gsdme deficiency. Myeloid-specific Gsdme reintroduction rescued TRM expansion and function, curbed FAP adipogenic reprogramming, whereas FAP-specific expression proved ineffective. Mechanistically, IL-18 downstream of GSDME-dependent signaling engaged KLF4/JUN signaling in TRMs, sustaining their reparative and lipid-clearing capacity. This GSDME–IL-18–TRMs axis was compromised in aged muscle, yet exogenous IL-18 reversed myosteatosis and accelerated regeneration. Together, these findings suggest that GSDME-dependent pyroptotic signaling can act as a metabolic checkpoint that sustains TRM-driven lipid homeostasis to support muscle regeneration.
Authors
Qi Cao, Jian Liu, Gang Huang, Su-Yuan Wang, Guo-Dong Lu, Yong Huang, Yi-Ting Chen, Zhen Zhang, Jiang-Tao Fu, Si-Jia Sun, Xiaofei Chen, Chunlin Zhuang, Chunquan Sheng, Fu-Ming Shen, Dong-Jie Li, Pei Wang
Abstract
Obesity is accompanied by increases in free fatty acids (FFAs) in the systemic circulation, and obese patients often develop cardiac hypertrophy and diastolic dysfunction, termed obesity cardiomyopathy. Proinflammatory cytokines, including IL-6, have been implicated in the pathogenesis of the cardiac dysfunction associated with obesity cardiomyopathy. Elevation of FFAs induced by high fat diet (HFD) consumption induced diastolic dysfunction in the heart as early as after one month. HFD consumption directly stimulated IL-6 production in cardiomyocytes before local inflammation developed and induced diastolic dysfunction even in the presence of macrophage depletion with clodronate in the heart. PPARα played an essential role in mediating Il6 transcription in response to HFD consumption by forming a heterodimer with p50/RelA and binding to the NFκB element in cardiomyocytes. Local production of IL-6 in cardiomyocytes, in turn, mediated the development of diastolic cardiac dysfunction. HFD-induced diastolic dysfunction was attenuated by cardiac-specific deletion of either Ppara or Il6, as well as by interference with the PPARα-NFκB heterodimer formation by a molecular decoy. These results suggest that elevated FFAs directly upregulate Il6 through the PPARα-NFκB heterodimer in cardiomyocytes and highlight autocrine production of IL-6 as a key downstream mechanism in the initial development of diastolic dysfunction.
Authors
Shin-ichi Oka, Eun-Ah Sung, Peiyong Zhai, Kevin B. Schesing, Santosh Bhat, Adave Chin, Jiyeon Park, Yeun-Jun Chung, Akihiro Shirakabe, Takanobu Yamamoto, Yoshiyuki Ikeda, Wataru Mizushima, Shohei Ikeda, Mingming Tong, Jaemin Byun, Michinari Nakamura, Samuel I. Kim, Jamie Francisco, Dominic P. Del Re, Junichi Sadoshima
Abstract
Background Youth with type 2 diabetes (T2D) and severe obesity face high risk of diabetic kidney disease, which metabolic bariatric surgery (MBS) can mitigate. This study explores structural and molecular changes in kidneys after vertical sleeve gastrectomy (VSG), a form of MBS. Methods Paired analyses, including metabolic profiling, kidney volume assessment, histological evaluation, and single-cell RNA sequencing (scRNAseq) on kidney biopsies from five youth with T2D and obesity pre- and 12 months post-VSG in the IMPROVE-T2D (Impact of Metabolic surgery on Pancreatic, Renal and cardiOVascular hEalth in youth with T2D) cohort. Circulating proteomics with kidney transcriptomics, were linked using data from an independent cohort of youth with obesity, with or without T2D, undergoing MBS in Teen-Longitudinal Assessment of Bariatric Surgery (Teen-LABS, n=64). Results Post-VSG, participants lost weight and had improvements in insulin sensitivity and metabolic parameters. Kidney changes included reduced renal hyperfiltration, total kidney volume, mesangial matrix area, and microalbuminuria. scRNAseq in proximal tubule (PT) and thick ascending limb cells indicated repression of glycolysis, gluconeogenesis, and tricarboxylic acid cycle genes, with upregulation of AMP-activated protein kinase (AMPK) and Forkhead box O3 (FOXO3). Decreased metabolic signaling aligned with reduced ribosomal phosphorylated S6K (pS6K), suggesting attenuated mTORC1 activity. JAK-STAT pathway activation in PT was diminished, correlating with lower circulating ligands from Teen-LABS proteomic data. Conclusion MBS/VSG prompts kidney molecular adaptations, providing potential targets for non-surgical interventions against obesity- and diabetes-associated kidney disease.
Authors
Abhijit S. Naik, Fadhl M. Alakwaa, Viji Nair, Phillip J. McCown, Jennifer A. Schaub, Edgar A. Otto, Rajasree Menon, Francesca Annese, Ye Ji Choi, Hailey E. Hampson, Thomas H. Inge, John Hartman, Sean Eddy, Cathy Smith, Jeffrey B. Hodgin, Ken Inoki, Swayam Prakash Srivastava, Kareem Al-Fagih, Shota Yoshida, Jesse A. Goodrich, Melanie G. Cree, Phoom Narongkiatikhun, Long Yuan, Kalie L. Tommerdahl, Pottumarthi Prasad, Daniël H. van Raalte, Megan M. Kelsey, Justin R. Ryder, Tyler J. Dobbs, Patricia Ladd, Subramaniam Pennathur, Robert G. Nelson, Yusuke Okabayashi, Victor G. Puelles, Jenna Ferrence-Salo, Jeffrey A. Beamish, Frank C. Brosius, Kristen J. Nadeau, Laura Pyle, Matthias Kretzler, Petter Bjornstad
Abstract
Ceramides are essential skin lipids for maintaining the mammalian skin permeability barrier, which protects against external stimuli. The precursor of epidermal ceramides, glucosylceramides (GlcCer), is synthesized within granular keratinocytes while its precise cellular transport mechanisms remain poorly characterized. Here, we identified three pathogenic variants in the GLTP gene, which encodes glycolipid transfer protein, in five unrelated families with nonsyndromic epidermal differentiation disorder presenting with generalized skin scaling. The biallelic GLTP variants resulted in loss of competent GLTP expression. CRISPR/Cas9-generated Gltp knockout mice exhibited lethal barrier defects, partially recapitulating the clinical features of our patients. We demonstrated that GLTP facilitated GlcCer transport in differentiated keratinocytes, with its deficiency causing impaired GlcCer trafficking and consequent aberrant retention in lysosomes, thereby disrupted lysosome function. The lysosomal dysfunction impaired autophagy flux, resulting in delayed keratinocyte terminal differentiation, which is expected to compromise the skin barrier integrity and ultimate abnormal scaling. Pharmaceutical inhibition of GlcCer synthesis effectively rescued both autophagy and keratinocyte differentiation defects. Our findings establish GLTP as a novel underlying gene for nonsyndromic epidermal differentiation disorders and unravel its essential role in maintaining skin homeostasis during terminal differentiation by mediating epidermal GlcCer transport.
Authors
Zeqiao Zhang, Shimiao Huang, Adam Jackson, Elizabeth A. Jones, Siddharth Banka, Chao Yang, Sisi Zhao, Kunlun Lv, Sha Peng, Zhimiao Lin, Huijun Wang



Copyright © 2026 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)