Advertisement
- Corrigendum (August 2006)
- Erratum (August 2006)
Review Series Free access | 10.1172/JCI29069
Inflammation and insulin resistance
Steven E. Shoelson, Jongsoon Lee, and Allison B. Goldfine
Joslin Diabetes Center and Department of Medicine, Harvard Medical School, Boston, Massachusetts, USA.
Address correspondence to: Steven E. Shoelson, Joslin Diabetes Center, One Joslin Place, Boston, Massachusetts 02215, USA. E-mail: steven.shoelson@joslin.harvard.edu .
Find articles by Shoelson, S. in: PubMed | Google Scholar
Joslin Diabetes Center and Department of Medicine, Harvard Medical School, Boston, Massachusetts, USA.
Address correspondence to: Steven E. Shoelson, Joslin Diabetes Center, One Joslin Place, Boston, Massachusetts 02215, USA. E-mail: steven.shoelson@joslin.harvard.edu .
Find articles by Lee, J. in: PubMed | Google Scholar
Joslin Diabetes Center and Department of Medicine, Harvard Medical School, Boston, Massachusetts, USA.
Address correspondence to: Steven E. Shoelson, Joslin Diabetes Center, One Joslin Place, Boston, Massachusetts 02215, USA. E-mail: steven.shoelson@joslin.harvard.edu .
Find articles by Goldfine, A. in: PubMed | Google Scholar
Published July 3, 2006 - More info
J Clin Invest. 2006;116(7):1793–1801. https://doi.org/10.1172/JCI29069.
© 2006 The American Society for Clinical Investigation
-
Abstract
Over a hundred years ago, high doses of salicylates were shown to lower glucose levels in diabetic patients. This should have been an important clue to link inflammation to the pathogenesis of type 2 diabetes (T2D), but the antihyperglycemic and antiinflammatory effects of salicylates were not connected to the pathogenesis of insulin resistance until recently. Together with the discovery of an important role for tissue macrophages, these new findings are helping to reshape thinking about how obesity increases the risk for developing T2D and the metabolic syndrome. The evolving concept of insulin resistance and T2D as having immunological components and an improving picture of how inflammation modulates metabolism provide new opportunities for using antiinflammatory strategies to correct the metabolic consequences of excess adiposity.
-
Historical perspectives on the link between inflammation and insulin resistance
Clues to the involvement of inflammation in diabetes date back to more than a century ago, when high doses of sodium salicylate (5.0–7.5 g/d) were first demonstrated to diminish glycosuria in diabetic patients having “the milder form of the disease,” presumably type 2 diabetes (T2D) (1–3). In 1876 Ebstein concluded that sodium salicylate could make the symptoms of diabetes mellitus totally disappear (1, 3). Similarly, in 1901 Williamson found that “sodium salicylate had a definite influence in greatly diminishing the sugar excretion” (2). The effect was rediscovered in 1957 when an insulin-treated diabetic, given high-dose aspirin to treat the arthritis associated with rheumatic fever, no longer required daily insulin injections (4). Fasting and postchallenge glucose concentrations were nearly normal, despite the discontinuation of insulin and treatment with aspirin alone. Upon resolution of the joint symptoms, the aspirin was discontinued, and a repeat glucose tolerance test was grossly abnormal. Intrigued by these findings, Reid and colleagues prospectively studied 7 additional patients, 4 the “overweight mild type” and three “lean more severe diabetics” (4). Over a 2-week course of high-dose aspirin (5.0–8.0 g/d), fasting blood glucose levels fell from an average of more than 190 mg/dl before treatment to 92 mg/dl; every patient responded. Additional trials showed equivalent efficacy (5, 6). Mechanistic studies focused on insulin secretion, undoubtedly because of the established importance of insulin secretion in the pathogenesis of diabetes, but the findings were inconclusive (7). Insulin resistance and its role in the pathogenesis of T2D were less well appreciated, and, as a result, insulin sensitization was not considered as a potential mechanism for glucose lowering at the time. It wasn’t until much later that studies looking at a role for inflammation in the pathogenesis of insulin resistance reinvestigated the hypoglycemic actions of salicylates and identified the molecular target to be the IκB kinase-β (IKKβ)/NF-κB axis (8–10).
Although epidemiological associations relating inflammation to T2D or obesity can be traced to the late 1950s and 1960s, when increases were found in circulating concentrations of fibrinogen and other acute-phase reactants (11–13), the findings similarly failed to influence thoughts about pathogenesis. More recently, additional epidemiological studies confirmed and extended these early findings (14). Increased levels of markers and mediators of inflammation and acute-phase reactants such as fibrinogen, C-reactive protein (CRP), IL-6, plasminogen activator inhibitor-1 (PAI-1), sialic acid, and white cell count correlate with incident T2D (15–25). Markers of inflammation and coagulation are reduced with intensive lifestyle intervention, as was performed in the diabetes prevention program (26), but experiments showing that adipose tissue–derived proinflammatory cytokines such as TNF-α could actually cause insulin resistance in experimental models provided the necessary impetus to begin thinking in terms of pathogenesis (27–29). This discovery gave the field a critical boost, because epidemiological studies, while highly informative, are correlative by nature and, alone, are unable to determine causality. These different areas of research have coalesced sufficiently that credible hypotheses can now link inflammation to the development of insulin resistance and pathogenesis of T2D (30, 31).
-
Molecular pathways that link inflammation and insulin resistance
Hotamisligil and colleagues (27) and Karasik and colleagues (28) first showed that the proinflammatory cytokine TNF-α was able to induce insulin resistance. This was a revolutionary idea, that a substance produced by fat — and overproduced by expanded fat — had local and potentially systemic effects on metabolism. The concept of fat as a site for the production of cytokines and other bioactive substances quickly extended beyond TNF-α to include leptin, IL-6, resistin, monocyte chemoattractant protein-1 (MCP-1), PAI-1, angiotensinogen, visfatin, retinol-binding protein-4, serum amyloid A (SAA), and others (32–36). Adiponectin is similarly produced by fat, but expression decreases with increased adiposity (37). While leptin and adiponectin are true adipokines that appear to be produced exclusively by adipocytes, TNF-α, IL-6, MCP-1, visfatin, and PAI-1 are expressed as well at high levels in activated macrophages and/or other cells. The relative amount of each produced by the adipocyte versus associated adipose tissue macrophages remains unknown. Sites of resistin production are more complex; they include macrophages in humans but both adipocytes and macrophages in rodents (34). TNF-α, IL-6, resistin, and undoubtedly other pro- or antiinflammatory cytokines appear to participate in the induction and maintenance of the subacute inflammatory state associated with obesity. MCP-1 and other chemokines have essential roles in the recruitment of macrophages to adipose tissue. These cytokines and chemokines activate intracellular pathways that promote the development of insulin resistance and T2D.
The investigations that focused on intracellular pathways activated by inflammation, instead of individual cytokines, have helped to restructure the framework for thinking about insulin resistance. As mentioned above, the antihyperglycemic effects of salicylates focused attention on IKKβ and NF-κB (38–40). However, increasing adiposity activates both JNK and IKKβ (8, 41–43). Many of the more typical proinflammatory stimuli simultaneously activate JNK and IKKβ pathways, including cytokines and TLRs (Figure 1). Concordantly, genetic or chemical inhibition of either JNK or IKKβ/NF-κB can improve insulin resistance. The several hypothesized mechanisms that might explain how obesity activates JNK and NF-κB can be separated into receptor and nonreceptor pathways (Figure 1). Proinflammatory cytokines such as TNF-α and IL-1β activate JNK and IKKβ/NF-κB through classical receptor-mediated mechanisms that have been well characterized (Figure 1). JNK and IKKβ/NF-κB are also activated by pattern recognition receptors, defined as surface proteins that recognize foreign substances. These include the TLRs and the receptor for advanced glycation end products (RAGE) (44). Many TLR ligands are microbial products, including LPS and lipopeptides derived from bacteria (44). The fact that TLRs recognize microbial lipid conjugates has led to speculation that endogenous lipids or lipid conjugates might also activate 1 or more of the TLRs in obesity, a possibility supported by experiments showing that saturated fatty acids bind and activate TLR4 (45). Likewise, RAGE binds a variety of ligands, including endogenous advanced glycation end products (AGEs) and a distinct set of microbial products (46, 47). AGEs are nonenzymatic adducts formed between glucose and targeted proteins, particularly those with slow rates of turnover. Prolonged hyperglycemia and the accompanying production of excess quantities of AGEs can activate NF-κB.
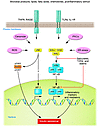 Figure 1
Figure 1Potential cellular mechanisms for activating inflammatory signaling. Obesity and high-fat diet activate IKKβ/NF-κB and JNK pathways in adipocytes, hepatocytes, and associated macrophages. Stimuli that have been shown to activate these pathways during metabolic dysregulation include ligands for TNF-α, IL-1, Toll, or AGE receptors (TNFR, IL-1R, TLR, or RAGE, respectively), intracellular stresses including ROS and ER stress, ceramide, and various PKC isoforms. Obesity-induced IKKβ activation leads to NF-κB translocation and the increased expression of numerous markers and potential mediators of inflammation that can cause insulin resistance. Obesity-induced JNK activation promotes the phosphorylation of IRS-1 at serine sites that negatively regulate normal signaling through the insulin receptor/IRS-1 axis. Examples include serine-302 (pS302) and serine-307 (pS307). By contrast, evidence has not been reported for obesity-induced effects on transcription factors such as AP-1 that are regulated by JNK. IKKβ and/or NF-κB are inhibited or repressed by the actions of salicylates, TZDs, and statins.
In addition to proinflammatory cytokine and pattern recognition receptors, cellular stresses activate JNK and NF-κB, including ROS and ER stress. Systemic markers of oxidative stress increase with adiposity, consistent with a role for ROS in the development of obesity-induced insulin resistance (48). One potential mechanism is through the activation of NADPH oxidase by lipid accumulation in the adipocyte, which increases ROS production (49). This mechanism was shown to increase the production of TNF-α, IL-6, and MCP-1, and decrease the production of adiponectin. Consistent with this, the antioxidant N-acetyl cysteine can reduce ROS and improve insulin resistance in a hyperglycemia-induced model (50). Lipid accumulation also activates the unfolded protein response to increase ER stress in fat and liver (51). ER stress was shown to activate JNK to lead to serine phosphorylation of insulin receptor substrate-1 (IRS-1), but as with all of the stimuli described in Figure 1, ER stress similarly activates NF-κB.
Ceramides may form under conditions of cell stress and promote cellular signaling, including the regulation of apoptosis. Saturated fats may also promote the synthesis of ceramides, which accumulate in tissues such as muscle and may correlate with the degree of insulin resistance (52). Ceramides can also activate inflammatory pathways including JNK and NF-κB (53). Lipid excess increases the activities of various PKC isoforms. Acute lipid infusion activates PKC-θ in rodent muscle and PKC-βII and PKC-δ in human muscle, which may also activate IKKβ and NF-κB (54, 55). Consistent with these findings, salicylates improve muscle insulin resistance after lipid infusion (56), although the relevance of the acute lipid infusion model to the pathology of obesity-induced insulin resistance is questionable. One or more of the upstream activators of inflammation listed in Figure 1 may be relevant to the in vivo pathogenesis of insulin resistance, but more information is needed to determine which of these or others predominate. Once activated, however, the processes can be self-perpetuating through a positive-feedback loop created by the produced proinflammatory cytokines.
-
Transcription versus phosphorylation in the pathogenesis of insulin resistance
While both JNK and IKKβ/NF-κB play important roles in inflammation-induced insulin resistance, accumulated evidence suggests that they do so through dissimilar mechanisms. JNK is a stress kinase that normally phosphorylates the c-Jun component of the AP-1 transcription factor, but to date there are no known links between this well-established transcriptional pathway and JNK-induced insulin resistance. Instead, JNK has been shown to promote insulin resistance through the phosphorylation of serine residues in IRS-1 (41, 42, 51, 57, 58) (Figure 1). Insulin receptor signaling that normally occurs through a tyrosine kinase cascade is inhibited by counterregulatory serine/threonine phosphorylations (59).
In contrast, IKKβ is highly selective toward its physiological substrates, the IκB protein inhibitors of NF-κB. Phosphorylation by IKKβ targets IκBα for proteasomal degradation, which liberates NF-κB for translocation into the nucleus, where it promotes the expression of numerous target genes whose products induce insulin resistance (see Box 1). Unlike JNK, IKKβ does not phosphorylate IRS-1 to cause insulin resistance but causes insulin resistance through transcriptional activation of NF-κB. Increased lipid deposition in adipocytes leads to the production of proinflammatory cytokines, including TNF-α, IL-6, IL-1β, and resistin, which further activate JNK and NF-κB pathways through a feed-forward mechanism. In addition to the cytokines, there is upregulated expression of transcriptions factors, receptors, and other relevant proteins including chemokines that recruit monocytes and stimulate their differentiation into macrophages (Box 1).
Inflammation is also closely linked to the pathogenesis of atherosclerosis, suggesting that inflammation might be a common denominator that links obesity to many of its pathological sequelae. Overlapping collections of transcriptionally regulated inflammatory proteins participate in the pathogenesis of these disorders (Box 1). Signs of inflammation accompany even the earliest accumulation of lipid within the arterial wall, including the upregulation of the cell adhesion molecules P- and E-selectin, ICAM-1, and VCAM-1, which localizes circulating immune cells (60, 61). The adherent cells can migrate into the subendothelial space, where they contribute to the local inflammatory response. Cytokines and chemokines produced locally include MCP-1 and macrophage inflammatory protein-1α (MIP-1α), MIP-1β, MIP-2, and MIP-3α. T cell activation leads to expression of IFN-γ and lymphotoxin; macrophages, endothelial cells, and SMCs produce TNF-α (62, 63); and together these stimulate the local production of IL-6 in the atheroma (64, 65). The additional engagement of CD40 and CD40 ligand promotes these processes as well as increasing MMP expression (66). The latter can break down collagen and tissue factor, an important mediator of thrombosis (67).
As vascular remodeling progresses, the accumulation of foam cells leads to the formation of a lipid pool, rich in prothrombotic tissue factor. PDGF and TGF-β increase the rate of collagen production, which contributes to the formation of a fibrous cap. Conversely, IFN-γ halts collagen synthesis by SMCs. Activated macrophages secrete MMPs, which degrade collagen and render the fibrous cap weak and prone to rupture (68). Thus a dynamic balance is maintained between collagen synthesis and breakdown. If proinflammatory forces predominate, the fibrous cap may thin and eventually rupture, with release of prothrombotic lipids into the lumen. This may herald the onset of an acute ischemic event. NF-κB regulates many of the proteins that mediate the atherogenic process, in common with the pathogenesis of insulin resistance, suggesting that small increases in obesity-induced inflammation might promote both processes via common mechanisms. This also suggests the corollary that pharmacological decreases in inflammatory activity might coordinately downregulate the production of a number of proteins involved in the pathogenesis of insulin resistance, T2D, and cardiovascular disease (CVD).
-
Where is inflammation-induced insulin resistance initiated?
Adipose tissue has attracted a great deal of attention as a pathogenic site of obesity-induced insulin resistance, partly because changes in adiposity are easy to see but also because fat produces bioactive proteins that are readily detected and reflect the inflammatory state of the organ. However, it has also been firmly established that all fat is not equal; adipose tissue in the subcutaneous versus abdominal or visceral depots differs by cell size (69, 70), metabolic activity, and potential role in insulin resistance (71, 72). Visceral fat is more pathogenic. The adipocyte itself is integral to the development of obesity-induced inflammation. As discussed above, proteins produced by adipocytes that might collaboratively initiate the process include TNF-α, IL-6, resistin, leptin, adiponectin, MCP-1, PAI-1, and angiotensinogen, but since the recruited immune cells produce many of the same substances, with the exception of leptin and adiponectin, it is difficult to pinpoint precise sites of production. Myeloid-selective deletion of IKKβ improves obesity-induced insulin resistance, underscoring potential roles for both NF-κB and inflammatory cells including macrophages (73), but this has not helped to distinguish where the process is initiated. Both cell types, lipid-laden adipocytes and recruited macrophages, seem to participate in the pathogenesis of inflammation-induced insulin resistance (Figure 2). Since the bulk of accumulated lipid is stored in adipocytes, it is generally assumed that the adipocyte initiates the process and the macrophage serves to amplify the signal. Since many of the bioactive proteins involved are NF-κB targets, and NF-κB activation can be self-sustaining, antiinflammatory therapies including salicylates may coordinately decrease their expression and improve insulin resistance.
 Figure 2
Figure 2Potential mechanisms for activation of inflammation in adipose tissue. Dietary excess and obesity cause lipid accumulation in adipocytes, initiating a state of cellular stress and activation of JNK and NF-κB. These inflammatory signaling pathways regulate protein phosphorylation and cellular transcriptional events, thereby leading to increased adipocyte production of proinflammatory cytokines, including TNF-α, IL-6, leptin, and resistin, chemokines such as MCP-1, and other proatherogenic mediators, for example PAI-1. Endothelial adhesion molecules (e.g., ICAM-1 and VCAM-1) and chemoattractant molecules (designated CCX) bind integrins and chemokine receptors (CCR), respectively, on the monocyte surface to recruit them to the adipose tissues. The monocytes that differentiate into macrophages produce many of the same inflammatory cytokines and chemokines as those listed above, and additional ones, to further promote local inflammation and propagate the inflammatory diathesis systemically. pS, phosphoserine.
It is important to understand how increasing adiposity leads to the recruitment of immune cells to adipose tissue. MCP-1 (CCL2), a chemoattractant for monocytes, DCs, and memory T cells, is produced by adipocytes in parallel with increasing adiposity (74, 75), suggesting that MCP-1 might play a role in recruitment of monocytes. Consistent with this, mice lacking CCR2, an important receptor for MCP-1, are partly protected from developing high-fat diet–induced insulin resistance and exhibit reductions in adipose tissue macrophage recruitment and inflammatory gene expression (76). The fact that protection is incomplete implies that additional chemoattractant ligand-receptor pairs might be involved. It is also interesting that some macrophages found in the adipose tissue of obese rodents are large and multinucleated (74, 75, 77). Such multinucleate giant cells are often found at sites of chronic inflammation and result from the fusion or engulfment of macrophages by each other. Macrophages including multinucleate giant cells may aggregate at sites of adipocyte necrosis (77).
Other cell types in adipose tissue may also participate in the inflammatory process. Vascular cells are an obvious place to look. Adipose tissue is highly vascularized, with multiple capillaries in contact with each adipocyte (78). Moreover, adipose tissue rapidly proliferates and expands as nutrient stores increase, possibly using processes similar to the angiogenesis that supports tumor growth (77). In addition to being important for fat expansion, the microvasculature undoubtedly plays important roles in adipose tissue inflammation. For example, circulating leukocytes do not adhere to normal endothelium, but after initiation of a high-fat Western diet the endothelium expresses cell adhesion molecules that bind leukocytes (79). Adipose tissue endothelial cells may increase the expression of one or more of the adhesion proteins ICAM-1, VCAM-1, E-selectin, or P-selectin in response to increased adiposity. As mentioned earlier, MCP-1 induces the migration of blood monocytes into the subendothelial space and augments differentiation into macrophages. Thus changes are predicted in adipose tissue endothelial cells in response to altered adiposity. As macrophages rarely function alone, other types of immune cells are likely to participate in adipose tissue inflammation, although this has not yet been reported. In addition to cytokine and protease release, the actions of macrophages in inflammation include antigen presentation and T cell activation. Classical inflammation involves the added presence of neutrophils, DCs, NK cells, mast cells, and various subtypes of T lymphocytes. Potential roles for these other immune cells in adipose tissue inflammation will doubtless be topics for future investigation.
In addition to adipose tissue, the liver is affected by obesity (Figure 3). Nonalcoholic fatty liver disease (NAFLD) often accompanies abdominal adiposity, and its prevalence is increasing and closely parallels the prevalence of the comorbid conditions T2D and hyperlipidemia. The pathological spectrum of NAFLD ranges from simple steatosis to steatohepatitis, advanced fibrosis, and cirrhosis. Inflammation clearly plays a pivotal role in the progression of this disease process. While inadequate suppression of hepatic glucose production, due at least in part to hepatic insulin resistance, is an established contributor to hyperglycemia in T2D, the role of inflammation in the pathogenesis of these processes has only recently been explored. Inflammatory gene expression increases in liver with increasing adiposity (43). This suggests that hepatocyte lipid accumulation (steatosis) might induce a subacute inflammatory response in liver that is similar to the adipose tissue inflammation that follows adipocyte lipid accumulation. Alternatively, proinflammatory substances in the portal circulation, potentially produced in abdominal fat, might initiate hepatic inflammation. Regardless, NF-κB is activated in the hepatocyte, and cytokines including IL-6, TNF-α, and IL-1β are overproduced in fatty liver. The proinflammatory cytokines participate in the development of insulin resistance and activate Kupffer cells, the resident hepatic macrophages. Unlike adipose tissue, where macrophages are relatively sparse basally but increase numerically with adiposity, the liver is densely populated with Kupffer cells, which account for over 5% of total cells. The number of Kupffer cells does not increase with adiposity, but their activation state does (43). A wide variety of other immune cells are present in normal liver and may also play roles in inflammation-induced insulin resistance, including T and B lymphocytes, NK cells, and DCs as well as hepatic stellate cells and liver sinusoidal endothelial cells (80). NKT cells are enriched in normal mouse liver, and their numbers decrease in ob/ob or high-fat diet models of obesity (81, 82). NKT cells are regulatory lymphocytes, with features of both classical T (CD3+) and NK (NK1.1+) cells and characteristic expression of CD1d, an MHC class I homologue that presents glycolipid antigens to TCRs. Adoptive transfer of NKT cells reportedly improves nonalcoholic steatohepatitis and glucose intolerance in ob/ob mice (83), consistent with a role for decreased NKT numbers in the pathogenesis of these disorders.
 Figure 3
Figure 3Potential mechanisms for adiposity-induced inflammation in the liver. Healthy liver contains a broad repertoire of cells that participate in inflammatory and immune responses, including resident hepatic macrophages (Kupffer cells), B and T cells, NK and NKT cells, DCs, liver sinusoidal endothelial cells, hepatic stellate cells, and hepatocytes. Hepatic steatosis and obesity are accompanied by the activation of inflammatory signaling pathways in liver. Proinflammatory cytokines and FFAs, produced either by hepatocytes in response to steatosis or by abdominal fat tissue, may activate Kupffer cells. Numbers of regulatory NKT cells decrease in parallel with the Kupffer cell activation.
Skeletal muscle is another major site of insulin resistance in obesity and T2D. However, increasing adiposity does not appear to activate inflammatory cascades in skeletal muscle, as it does in fat and liver. Inflammation is activated in muscle by intralipid infusion, but this is distinct from the effects of increasing adiposity. The lipid infusion model is a research tool used to acutely raise circulating and intratissue fatty acid levels and induce insulin resistance. Intralipid infusion activates PKC-θ and IKKβ in mouse muscle, and the associated insulin resistance is inhibited by salicylate or IKKβ depletion (54, 56). This is in contrast with high-fat diet–induced and obesity-induced insulin resistance, neither of which activates IKKβ/NF-κB in skeletal muscle (84, 85) or leads to an increase in skeletal muscle macrophages (75). Concordantly, neither muscle-specific ablation of IKKβ nor muscle-specific inhibition of NF-κB improves insulin resistance in obese mice (84, 85). It is perhaps more appropriate to think of skeletal muscle as a target of inflammation-induced insulin resistance as opposed to a site of initiation (Figure 4).
 Figure 4
Figure 4Local, portal, and systemic effects of inflammation in insulin resistance and atherogenesis. Increasing adiposity activates inflammatory responses in fat and liver, with associated increases in the production of cytokines and chemokines. Immune cells including monocytes and macrophages are recruited and/or activated, and together these cause local insulin resistance. Portal delivery of abdominal fat–derived cytokines and lipids contributes to hepatic inflammation and insulin resistance. Proinflammatory and proatherogenic mediators are produced in the adipose tissue and liver and associated immune cells. This creates a systemic inflammatory diathesis that promotes insulin resistance in skeletal muscle and other tissues and atherogenesis in the vasculature.
-
Future trials to target inflammation
While demonstrating that TNF-α could induce insulin resistance (27, 28) was paramount in linking inflammation to the pathogenesis of insulin resistance, studies to evaluate whether blocking TNF-α with mAbs improves insulin sensitivity have so far been inconclusive (86, 87). This may be due in part to small trial sizes and inadequate statistical power but might also be related to mechanisms of pathogenesis. TNF-α by itself may just not be that important. With multiple cytokines and chemokines involved, it is also possible that different combinations of cytokines and chemokines might be more or less important in different patients. If this were true, then neutralization strategies might need to be individually tailored. It may be more prudent to modulate signaling at convergent sites of integration, such as JNK or IKKβ/NF-κB, since this would provide a more general strategy for treatment. Several drugs in current clinical practice have been shown to have antiinflammatory properties or side effects distinct from their major mechanisms of action, including members of the thiazolidinedione (TZD) class of PPARγ agonists and members of the statin class of HMG CoA reductase inhibitors. Both appear to have important antiinflammatory properties and potential benefits beyond their primary actions on glucose homeostasis and cholesterol lowering, respectively.
TZDs, which include pioglitazone, rosiglitazone, and troglitazone (the latter is no longer in clinical use), are used to improve insulin sensitivity and reduce hyperglycemia in patients with T2D. The TZDs’ primary mode of action is through binding and activating PPARγ to induce the expression of a number of gene products with roles in adipocyte differentiation, lipid and glucose uptake, and fatty acid storage (88). TZDs’ beneficial actions in insulin sensitivity are often attributed to fatty acid sequestration in the adipose tissue. This reduces circulation levels of FFAs and keeps the fatty acids out of other tissues, including muscle and liver, where they can cause insulin resistance. But in addition to adipocytes, PPARγ is also expressed in macrophages and other immune cells, hepatocytes, endothelial cells, and VSMCs. The antiinflammatory actions of the TZDs appear to be mediated through the transrepression of NF-κB and consequent decreases in the expression of target genes for cytokine and growth factors, cell proliferation and migration, ECM remodeling, and cell cycle progression and differentiation. One proposed mechanism involves the TZD-dependent SUMOylation of PPARγ, which targets it to nuclear receptor corepressor–histone deacetylase-3 (NCoR-HDAC3) complexes on inflammatory gene promoters (such as NF-κB and AP-1). The binding of SUMOylated PPARγ stabilizes the corepressor complexes and prevents their clearance, thus maintaining the transcription factor complexes in a repressed state (89). It has even been suggested that TZDs exert antiinflammatory effects through PPARγ-independent activation of the glucocorticoid receptor (90). The clinical benefits of TZDs may in part depend upon antiinflammatory effects that work together with classical mechanisms of glucose and lipid regulation (91) to improve insulin sensitivity, promote plaque remodeling, and potentially reduce cardiovascular events (92, 93). Several other nuclear receptors, including PPARα, PPARδ, and liver X receptor (LXR), have also been shown to have antiinflammatory properties that may be beneficial for the treatment of metabolic or cardiovascular conditions (94, 95), although significant glucose-lowering effects have not been associated with agonists to these transcription factors.
Several of the clinically available statins have been shown to downregulate transcriptional activities of NF-κB, AP-1, and HIF-1α, with coordinate reductions in the expression of prothrombotic and inflammatory cytokines (95). Randomized clinical trials evaluating statins have also demonstrated reductions in CRP, multiple cytokines, and inflammatory markers. Despite these modest antiinflammatory properties, the statins do not appear to significantly influence either insulin resistance or glycemia.
The antiinflammatory properties of TZDs and statins are side effects distinct from their primary modes of action. By contrast, high-dose salicylates directly target inflammation by inhibiting NF-κB (38–40). The glucose-lowering effects of salicylates, seen decades ago in patients with diabetes (1–7), are now recognized as well to be due at least in part to NF-κB inhibition (8–10, 43, 73). More recent studies demonstrated that high-dose aspirin (~7.0 g/d) improved multiple metabolic measures in patients with T2D, including substantial reductions in fasting and postprandial glucose, triglycerides, and FFAs (9). These changes were associated with reduced hepatic glucose production and improvements in insulin-stimulated glucose disposal, assessed during euglycemic-hyperinsulinemic clamping. However, the therapeutic usefulness of high-dose aspirin is limited by the antithrombotic and anti–platelet aggregation effects, which, coupled with gastrointestinal irritation, are associated with unacceptably high risks of bleeding.
Aspirin is a prototypical NSAID that effectively inhibits the COX enzymes COX1 and COX2 through the irreversible modification of the enzymes’ active sites. This occurs through a transacetylation reaction; the acetyl group of aspirin migrates to and covalently modifies the enzymes to block their catalytic activities. In platelets this occurs even at low doses (80–100 mg/d), because they lack nuclei and cannot resynthesize COX1, and platelets are thus inactivated for their lifetimes. Aspirin at a typical dose of 650 mg covalently modifies COX1 and COX2 in all tissues, which similarly inhibits prostaglandin synthesis. NSAIDs other than aspirin do not transacetylate the COX enzymes but bind with sufficiently high affinity that the enzymes are competitively inhibited. The mechanism of action of high-dose salicylate is distinct, as it lacks an acetyl group and neither covalently modifies COX1 or COX2 nor binds with sufficient affinity to effectively inhibit the enzymes.
The nonacetylated salicylates, delivered as sodium salicylate, salsalate, and Trilisate, inhibit NF-κB (38–40). This is presumed to be through direct inhibition of IKKβ (40). The nonacetylated salicylates do not prolong bleeding times and may thus provide a relatively safe and effective means of targeting the subacute inflammation that underlies the obesity-related syndromes. In fact, clinical trials to test efficacy, tolerability, and durability of salsalate (Disalcid) are currently being undertaken in the NIH-funded TINSAL-T2D and -CVD trials (Targeting Inflammation with Salsalate in T2D or CVD, respectively). Other antiinflammatory strategies are also being considered, including the potential use of specific JNK or IKKβ inhibitors and compounds that block TNF-α, IL-6, TLR, or chemokine signaling or reduce oxidative or ER stress, but these studies are at much earlier stages.
-
Concluding remarks
While the importance of inflammation-induced insulin resistance is doubtless increasing in parallel with the epidemic of obesity, there are additional unrelated mechanisms associated with insulin resistance. For example, polymorphisms in genes encoding components of the insulin signaling pathway and the insulin-resistant syndromes in patients with lipodystrophy who lack adipose tissue are different from the insulin resistance in typical overweight patients with T2D. Whether antiinflammatory strategies are beneficial in these cases has not been investigated. Similarly unknown are the distinctions between populations, such as those of Asian descent who may exhibit the characteristics of adiposity-induced inflammation while relatively lean.
In summary, obesity, T2D, and CVD share a metabolic milieu characterized by insulin resistance and chronic subacute inflammation. While drugs that secondarily alter the inflammatory process are undoubtedly of great clinical importance, several lines of evidence suggest it might also be possible to directly target inflammation with pharmacological interventions to treat and/or prevent insulin resistance and T2D and modulate risk for CVD and other metabolic conditions. These approaches may provide clinical benefits to a large number of persons affected by the obesity epidemic and the related cluster of metabolic disorders.
-
Footnotes
Nonstandard abbreviations used: AGE, advanced glycation end product; CRP, C-reactive protein; CVD, cardiovascular disease; IKKβ, IκB kinase-β; IRS-1, insulin receptor substrate-1; MCP-1, monocyte chemoattractant protein-1; MIP, macrophage inflammatory protein; PAI-1, plasminogen activator inhibitor-1; RAGE, receptor for advanced glycation end products; T2D, type 2 diabetes; TZD, thiazolidinedione.
Conflict of interest: The authors have declared that no conflict of interest exists.
Reference information: J. Clin. Invest.116:1793–1801 (2006). doi:10.1172/JCI29069.
-
References
- Ebstein, W. 1876. Zur therapie des Diabetes mellitus, insbesondere über die Anwendung des salicylsauren Natron bei demselben. Berliner Klinische Wochenschrift. 13:337-340.
- Williamson, R.T. 1901. On the treatment of glycosuria and diabetes mellitus with sodium salicylate. Br. Med. J. 1:760-762. View this article via: PubMed Google Scholar
- Shoelson, S. 2002. Invited comment on W. Ebstein: on the therapy of diabetes mellitus, in particular on the application of sodium salicylate. J. Mol. Med. 80:618-619.
- Reid, J., Macdougall, A.I., Andrews, M.M. 1957. On the efficacy of salicylate in treating diabetes mellitus. Br. Med. J. 2:1071-1074. View this article via: PubMed Google Scholar
- Hecht, A., Goldner, M.G. 1959. Reappraisal of the hypoglycemic action of acetylsalicylate. Metabolism. 8:418-428. View this article via: PubMed Google Scholar
- Gilgore, S.G. 1960. The influence of salicylate on hyperglycemia. Diabetes. 9:392-393.
- Baron, S.H. 1982. Salicylates as hypoglycemic agents. Diabetes Care. 5:64-71.
- Yuan, M., et al. 2001. Reversal of obesity- and diet-induced insulin resistance with salicylates or targeted disruption ofIkk β. Science. 293:1673-1677.
- Hundal, R.S., et al. 2002. Mechanism by which high-dose aspirin improves glucose metabolism in type 2 diabetes. J. Clin. Invest. 109:1321-1326.
- Shoelson, S.E., Lee, J., Yuan, M. 2003. Inflammation and the IKKβ/IκB/NF-κB axis in obesity- and diet-induced insulin resistance. Int. J. Obes. Relat. Metab. Disord. 27(Suppl. 3):S49-S52.
- Fearnley, G.R., Vincent, C.T., Chakrabarti, R. 1959. Reduction of blood fibrinolytic activity in diabetes mellitus by insulin. Lancet. 2:1067. View this article via: PubMed Google Scholar
- Ogston, D., McAndrew, G.M. 1964. Fibrinolysis in obesity. Lancet. 14:1205-1207.
- Grace, C.S., Goldrick, R.B. 1968. Fibrinolysis and body build. Interrelationships between blood fibrinolysis, body composition and parameters of lipid and carbohydrate metabolism. J. Atheroscler. Res. 8:705-719. View this article via: PubMed Google Scholar
- Tataranni, P.A., Ortega, E. 2005. A burning question: does an adipokine-induced activation of the immune system mediate the effect of overnutrition on type 2 diabetes? Diabetes. 54:917-927.
- Schmidt, M.I., et al. 1999. Markers of inflammation and prediction of diabetes mellitus in adults (Atherosclerosis Risk in Communities study): a cohort study. Lancet. 353:1649-1652.
- Duncan, B.B., et al. 2003. Low-grade systemic inflammation and the development of type 2 diabetes: the Atherosclerosis Risk in Communities study. Diabetes. 52:1799-1805.
- Pradhan, A.D., Manson, J.E., Rifai, N., Buring, J.E., Ridker, P.M. 2001. C-reactive protein, interleukin 6, and risk of developing type 2 diabetes mellitus. JAMA. 286:327-334.
- Barzilay, J.I., et al. 2001. The relation of markers of inflammation to the development of glucose disorders in the elderly: the Cardiovascular Health Study. Diabetes. 50:2384-2389.
- Vozarova, B., et al. 2002. High white blood cell count is associated with a worsening of insulin sensitivity and predicts the development of type 2 diabetes. Diabetes. 51:455-461.
- Festa, A., D’Agostino, R., Tracy, R.P., Haffner, S.M. 2002. Elevated levels of acute-phase proteins and plasminogen activator inhibitor-1 predict the development of type 2 diabetes: the insulin resistance atherosclerosis study. Diabetes. 51:1131-1137.
- Freeman, D.J., et al. 2002. C-reactive protein is an independent predictor of risk for the development of diabetes in the West of Scotland Coronary Prevention Study. Diabetes. 51:1596-1600.
- Ford, E.S. 2002. Leukocyte count, erythrocyte sedimentation rate, and diabetes incidence in a national sample of US adults. Am. J. Epidemiol. 155:57-64.
- Prince, R.L., Larkins, R.G., Alford, F.P. 1981. The effect of acetylsalicylic acid on plasma glucose and the response of glucose regulatory hormones to intravenous glucose and arginine in insulin treated diabetics and normal subjects. Metabolism. 30:293-298.
- Nakanishi, N., Yoshida, H., Matsuo, Y., Suzuki, K., Tatara, K. 2002. White blood-cell count and the risk of impaired fasting glucose or type II diabetes in middle-aged Japanese men. Diabetologia. 45:42-48.
- Spranger, J., et al. 2003. Inflammatory cytokines and the risk to develop type 2 diabetes: results of the prospective population-based European Prospective Investigation into Cancer and Nutrition (EPIC)-Potsdam Study. Diabetes. 52:812-817.
- Haffner, S., et al. 2005. Intensive lifestyle intervention or metformin on inflammation and coagulation in participants with impaired glucose tolerance. Diabetes. 54:1566-1572.
- Hotamisligil, G.S., Shargill, N.S., Spiegelman, B.M. 1993. Adipose expression of tumor necrosis factor-α: direct role in obesity-linked insulin resistance. Science. 259:87-91.
- Feinstein, R., Kanety, H., Papa, M.Z., Lunenfeld, B., Karasik, A. 1993. Tumor necrosis factor-α suppresses insulin-induced tyrosine phosphorylation of insulin receptor and its substrates. J. Biol. Chem. 268:26055-26058. View this article via: PubMed Google Scholar
- Hotamisligil, G.S., Spiegelman, B.M. 1994. Tumor necrosis factor alpha: a key component of the obesity-diabetes link. Diabetes. 43:1271-1278.
- Pickup, J.C., Crook, M.A. 1998. Is type II diabetes mellitus a disease of the innate immune system? Diabetologia. 41:1241-1248.
- Kolb, H., Mandrup-Poulsen, T. 2005. An immune origin of type 2 diabetes? Diabetologia. 48:1038-1050.
- Zhang, Y., Proenca, R., Maffei, M., Barone, M., Leopold, L., Friedman, J.M. 1994. Positional cloning of the mouse obese gene and its human homologue. Nature. 372:425-432.
- Fried, S.K., Bunkin, D.A., Greenberg, A.S. 1998. Omental and subcutaneous adipose tissues of obese subjects release interleukin-6: depot difference and regulation by glucocorticoid. J. Clin. Endocrinol. Metab. 83:847-850.
- Steppan, C.M., et al. 2001. The hormone resistin links obesity to diabetes. Nature. 409:307-312.
- Shimomura, I., et al. 1996. Enhanced expression of PAI-1 in visceral fat: possible contributor to vascular disease in obesity. Nat. Med. 2:800-803.
- Fukuhara, A., et al. 2005. Visfatin: a protein secreted by visceral fat that mimics the effects of insulin. Science. 307:426-430.
- Scherer, P.E., Williams, S., Fogliano, M., Baldini, G., Lodish, H.F. 1995. A novel serum protein similar to C1q, produced exclusively in adipocytes. J. Biol. Chem. 270:26746-26749.
- Kopp, E., Ghosh, S. 1994. Inhibition of NF-kappa B by sodium salicylate and aspirin. Science. 265:956-959.
- Pierce, J.W., Read, M.A., Ding, H., Luscinskas, F.W., Collins, T. 1996. Salicylates inhibit I kappa B-alpha phosphorylation, endothelial-leukocyte adhesion molecule expression, and neutrophil transmigration. J. Immunol. 156:3961-3969. View this article via: PubMed Google Scholar
- Yin, M.J., Yamamoto, Y., Gaynor, R.B. 1998. The anti-inflammatory agents aspirin and salicylate inhibit the activity of IκB kinase-β. Nature. 396:77-80.
- Aguirre, V., Uchida, T., Yenush, L., Davis, R., White, M.F. 2000. The c-Jun N-terminal kinase promotes insulin resistance during association with insulin receptor substrate-1 and phosphorylation of Ser(307). J. Biol. Chem. 275:9047-9054.
- Hirosumi, J., et al. 2002. A central role for JNK in obesity and insulin resistance. Nature. 420:333-336.
- Cai, D., et al. 2005. Local and systemic insulin resistance resulting from hepatic activation of IKKβ and NF-κB. Nat. Med. 11:183-190.
- Akira, S., Uematsu, S., Takeuchi, O. 2006. Pathogen recognition and innate immunity. Cell. 124:783-801.
- Lee, J.Y., Sohn, K.H., Rhee, S.H., Hwang, D. 2001. Saturated fatty acids, but not unsaturated fatty acids, induce the expression of cyclooxygenase-2 mediated through Toll-like receptor 4. J. Biol. Chem. 276:16683-16689.
- Ramasamy, R., Yan, S.F., Schmidt, A.M. 2005. The RAGE axis and endothelial dysfunction: maladaptive roles in the diabetic vasculature and beyond. Trends Cardiovasc. Med. 15:237-243.
- Bierhaus, A., et al. 2005. Understanding RAGE, the receptor for advanced glycation end products. J. Mol. Med. 83:876-886.
- Keaney, J.F., et al. 2003. Obesity and systemic oxidative stress: clinical correlates of oxidative stress in the Framingham Study. Arterioscler. Thromb. Vasc. Biol. 23:434-439.
- Furukawa, S., et al. 2004. Increased oxidative stress in obesity and its impact on metabolic syndrome. J. Clin. Invest. 114:1752-1761.
- Lin, Y., et al. 2005. The hyperglycemia-induced inflammatory response in adipocytes: the role of reactive oxygen species. J. Biol. Chem. 280:4617-4626.
- Ozcan, U., et al. 2004. Endoplasmic reticulum stress links obesity, insulin action, and type 2 diabetes. Science. 306:457-461.
- Straczkowski, M., et al. 2004. Relationship between insulin sensitivity and sphingomyelin signaling pathway in human skeletal muscle. Diabetes. 53:1215-1221.
- Summers, S.A. 2006. Ceramides in insulin resistance and lipotoxicity. Prog. Lipid Res. 45:42-72.
- Griffin, M.E., et al. 1999. Free fatty acid-induced insulin resistance is associated with activation of protein kinase C theta and alterations in the insulin signaling cascade. Diabetes. 48:1270-1274.
- Itani, S.I., Ruderman, N.B., Schmieder, F., Boden, G. 2002. Lipid-induced insulin resistance in human muscle is associated with changes in diacylglycerol, protein kinase C, and IkappaB-alpha. Diabetes. 51:2005-2011.
- Kim, J.K., et al. 2001. Prevention of fat-induced insulin resistance by salicylate. J. Clin. Invest. 108:437-446.
- Aguirre, V., et al. 2002. Phosphorylation of Ser307 in insulin receptor substrate-1 blocks interactions with the insulin receptor and inhibits insulin action. J. Biol. Chem. 277:1531-1537.
- Werner, E.D., Lee, J., Hansen, L., Yuan, M., Shoelson, S.E. 2004. Insulin resistance due to phosphorylation of insulin receptor substrate-1 at serine 302. J. Biol. Chem. 279:35298-35305.
- Zick, Y. 2005. Ser/Thr phosphorylation of IRS proteins: a molecular basis for insulin resistance. Sci. STKE. 268:e4.
- Tedder, T.F., Steeber, D.A., Chen, A., Engel, P. 1995. The selectins: vascular adhesion molecules. FASEB J. 9:866-873. View this article via: PubMed Google Scholar
- Adams, D.H., Shaw, S. 1994. Leucocyte-endothelial interactions and regulation of leucocyte migration. Lancet. 343:831-836.
- Warner, S.J., Libby, P. 1989. Human vascular smooth muscle cells. Target for and source of tumor necrosis factor. J. Immunol. 142:100-109. View this article via: PubMed Google Scholar
- Barath, P., et al. 1990. Detection and localization of tumor necrosis factor in human atheroma. Am. J. Cardiol. 65:297-302.
- Seino, Y., et al. 1994. Interleukin 6 gene transcripts are expressed in human atherosclerotic lesions. Cytokine. 6:87-91.
- Rus, H.G., Vlaicu, R., Niculescu, F. 1996. Interleukin-6 and interleukin-8 protein and gene expression in human arterial atherosclerotic wall. Atherosclerosis. 127:263-271.
- Schonbeck, U., Libby, P. 2001. CD40 signaling and plaque instability. Circ. Res. 89:1092-1103.
- Mach, F., Schonbeck, U., Bonnefoy, J.Y., Pober, J.S., Libby, P. 1997. Activation of monocyte/macrophage functions related to acute atheroma complication by ligation of CD40: induction of collagenase, stromelysin, and tissue factor. Circulation. 96:396-399. View this article via: PubMed Google Scholar
- Libby, P. 2001. Current concepts of the pathogenesis of the acute coronary syndromes. Circulation. 104:365-372. View this article via: PubMed Google Scholar
- Johnson, P.R., Hirsch, J. 1972. Cellularity of adipose depots in six strains of genetically obese mice. J. Lipid Res. 13:2-11. View this article via: PubMed Google Scholar
- Krotkiewski, M., Bjorntorp, P., Sjostrom, L., Smith, U. 1983. Impact of obesity on metabolism in men and women. Importance of regional adipose tissue distribution. J. Clin. Invest. 72:1150-1162.
- Coon, P.J., Rogus, E.M., Drinkwater, D., Muller, D.C., Goldberg, A.P. 1992. Role of body fat distribution in the decline in insulin sensitivity and glucose tolerance with age. J. Clin. Endocrinol. Metab. 75:1125-1132.
- Gastaldelli, A., et al. 2002. Metabolic effects of visceral fat accumulation in type 2 diabetes. J. Clin. Endocrinol. Metab. 87:5098-5103.
- Arkan, M.C., et al. 2005. IKK-beta links inflammation to obesity-induced insulin resistance. Nat. Med. 11:191-198.
- Sartipy, P., Loskutoff, D.J. 2003. Monocyte chemoattractant protein 1 in obesity and insulin resistance. Proc. Natl. Acad. Sci. U. S. A. 100:7265-7270.
- Weisberg, S.P., et al. 2003. Obesity is associated with macrophage accumulation in adipose tissue. J. Clin. Invest. 112:1796-1808.
- Weisberg, S.P., et al. 2006. CCR2 modulates inflammatory and metabolic effects of high-fat feeding. J. Clin. Invest. 116:115-124.
- Kolonin, M.G., Saha, P.K., Chan, L., Pasqualini, R., Arap, W. 2004. Reversal of obesity by targeted ablation of adipose tissue. Nat. Med. 10:625-632.
- Crandall, D.L., Hausman, G.J., Kral, J.G. 1997. A review of the microcirculation of adipose tissue: anatomic, metabolic, and angiogenic perspectives. Microcirculation. 4:211-232.
- Blake, G.J., Ridker, P.M. 2002. Inflammatory bio-markers and cardiovascular risk prediction. J. Intern. Med. 252:283-294.
- Racanelli, V., Rehermann, B. 2006. The liver as an immunological organ. Hepatology. 43(Suppl. 1):S54-S62.
- Guebre-Xabier, M., et al. 2000. Altered hepatic lymphocyte subpopulations in obesity-related murine fatty livers: potential mechanism for sensitization to liver damage. Hepatology. 31:633-640.
- Li, Z., Soloski, M.J., Diehl, A.M. 2005. Dietary factors alter hepatic innate immune system in mice with nonalcoholic fatty liver disease. Hepatology. 42:880-885.
- Elinav, E., et al. 2006. Adoptive transfer of regulatory NKT lymphocytes ameliorates non-alcoholic steatohepatitis and glucose intolerance in ob/ob mice and is associated with intrahepatic CD8 trapping. J. Pathol. 209:121-128.
- Rohl, M., et al. 2004. Conditional disruption of IκB kinase 2 fails to prevent obesity-induced insulin resistance. J. Clin. Invest. 113:474-481.
- Cai, D., et al. 2004. IKKβ/NF-κB activation causes severe muscle wasting in mice. Cell. 119:285-298.
- Dominguez, H., et al. 2005. Metabolic and vascular effects of tumor necrosis factor-alpha blockade with etanercept in obese patients with type 2 diabetes. J. Vasc. Res. 42:517-525.
- Gonzalez-Gay, M.A., et al. 2006. Anti-tumor necrosis factor-alpha blockade improves insulin resistance in patients with rheumatoid arthritis. Clin. Exp. Rheumatol. 24:83-86. View this article via: PubMed Google Scholar
- Yki-Jarvinen, H. 2004. Thiazolidinediones. N. Engl. J. Med. 351:1106-1118.
- Pascual, G., et al. 2005. A SUMOylation-dependent pathway mediates transrepression of inflammatory response genes by PPAR-gamma. Nature. 437:759-763.
- Ialenti, A., et al. 2005. Mechanism of the anti-inflammatory effect of thiazolidinediones: relationship with the glucocorticoid pathway. Mol. Pharmacol. 67:1620-1628.
- Xiang, A.H., et al. 2006. Effect of pioglitazone on pancreatic beta-cell function and diabetes risk in Hispanic women with prior gestational diabetes. Diabetes. 55:517-522.
- Meisner, F., et al. 2006. Effect of rosiglitazone treatment on plaque inflammation and collagen content in nondiabetic patients: data from a randomized placebo-controlled trial. Arterioscler. Thromb. Vasc. Biol. 26:845-850.
- Dormandy, J.A., et al. 2005. Secondary prevention of macrovascular events in patients with type 2 diabetes in the PROactive Study (PROspective pioglitAzone Clinical Trial In macroVascular Events): a randomised controlled trial. Lancet. 366:1279-1289.
- Glass, C.K., Ogawa, S. 2006. Combinatorial roles of nuclear receptors in inflammation and immunity. Nat. Rev. Immunol. 6:44-55.
- Castrillo, A., Tontonoz, P. 2004. Nuclear receptors in macrophage biology: at the crossroads of lipid metabolism and inflammation. Annu. Rev. Cell Dev. Biol. 20:455-480.
-
Version history
- Version 1 (July 3, 2006): No description
Article tools
-
View PDF

- Download citation information
- Send a comment
- Terms of use
- Standard abbreviations
- Need help? Email the journal
Review Series
Diabetes
-
Insulin resistance and atherosclerosis
Clay F. Semenkovich -
Glucose transport and sensing in the maintenance of glucose homeostasis and metabolic harmony
Mark A. Herman et al. -
AMP-activated protein kinase signaling in metabolic regulation
Yun Chau Long et al. -
Central insulin action in energy and glucose homeostasis
Leona Plum et al. -
Inflammation and insulin resistance
Steven E. Shoelson et al. -
Inflammation and insulin resistance
Steven E. Shoelson et al. -
Islet β cell failure in type 2 diabetes
Marc Prentki et al. -
Adiponectin and adiponectin receptors in insulin resistance, diabetes, and the metabolic syndrome
Takashi Kadowaki et al. -
Insulin resistance and pancreatic β cell failure
Masato Kasuga
Metrics
Go to
- Top
- Abstract
- Historical perspectives on the link between inflammation and insulin resistance
- Molecular pathways that link inflammation and insulin resistance
- Transcription versus phosphorylation in the pathogenesis of insulin resistance
- Where is inflammation-induced insulin resistance initiated?
- Future trials to target inflammation
- Concluding remarks
- Footnotes
- References
- Version history



Copyright © 2026 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)




