Issue published April 1, 2003 Previous issue | Next issue

- Volume 111, Issue 7
Go to section:
-
Science in Medicine
×
Abstract
Authors
Michael Field
-
Research Articles
Taichi Sakaguchi, Shi Fang Yan, Shi Du Yan, Dmitri Belov, Ling Ling Rong, Monica Sousa, Martin Andrassy, Steven P. Marso, Stephan Duda, Bernd Arnold, Birgit Liliensiek, Peter P. Nawroth, David M. Stern, Ann Marie Schmidt, Yoshifumi NakaTaichi Sakaguchi, Shi Fang Yan, Shi Du Yan, Dmitri Belov, Ling Ling Rong, Monica Sousa, Martin Andrassy, Steven P. Marso, Stephan Duda, Bernd Arnold, Birgit Liliensiek, Peter P. Nawroth, David M. Stern, Ann Marie Schmidt, Yoshifumi Naka×
Abstract
Cellular proliferation, migration, and expression of extracellular matrix proteins and MMPs contribute to neointimal formation upon vascular injury. Wild-type mice undergoing arterial endothelial denudation displayed striking upregulation of receptor for advanced glycation end products (RAGE) in the injured vessel, particularly in activated smooth muscle cells of the expanding neointima. In parallel, two of RAGE’s signal transducing ligands, advanced glycation end products (AGEs) and S100/calgranulins, demonstrated increased deposition/expression in the injured vessel wall. Blockade of RAGE, employing soluble truncated receptor or antibodies, or in homozygous RAGE null mice, resulted in significantly decreased neointimal expansion after arterial injury and decreased smooth muscle cell proliferation, migration, and expression of extracellular matrix proteins. A critical role for smooth muscle cell RAGE signaling was demonstrated in mice bearing a transgene encoding a RAGE cytosolic tail-deletion mutant, specifically in smooth muscle cells, driven by the SM22α promoter. Upon arterial injury, neointimal expansion was strikingly suppressed compared with that observed in wild-type littermates. Taken together, these data highlight key roles for RAGE in modulating smooth muscle cell properties after injury and suggest that RAGE is a logical target for suppression of untoward neointimal expansion consequent to arterial injury.
Authors
Taichi Sakaguchi, Shi Fang Yan, Shi Du Yan, Dmitri Belov, Ling Ling Rong, Monica Sousa, Martin Andrassy, Steven P. Marso, Stephan Duda, Bernd Arnold, Birgit Liliensiek, Peter P. Nawroth, David M. Stern, Ann Marie Schmidt, Yoshifumi Naka
×Abstract
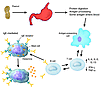
Neurogenic inflammation is believed to originate with the antidromic release of substance P, and of other neurokinins encoded by the preprotachykinin A (PPT-A) gene, from unmyelinated nerve fibers (C-fibers) following noxious stimuli. Consistent with this concept, we show here that selective sensory-fiber denervation with capsaicin and targeted deletion of the PPT-A gene protect murine lungs against both immune complex–mediated and stretch-mediated injuries. Reconstitution of PPT-A gene–deleted mice with WT bone marrow does not abrogate this protection, demonstrating a critical role for PPT-A gene expression by sensory neurons in pulmonary inflammation. Surprisingly, reconstitution of WT mice with PPT-A gene–deficient bone marrow also confers protection against pulmonary injury, revealing that PPT-A gene expression in hemopoietic cells has a previously unanticipated essential role in tissue injury. Taken together, these findings demonstrate a critical synergy between capsaicin-sensitive sensory fibers and hemopoietic cells in neurokinin-mediated inflammation and suggest that such synergy may be the basis for a stereotypical mechanism of response to injury in the respiratory tract.
Authors
Mara Chavolla-Calderón, Meggan K. Bayer, J. Julio Pérez Fontán
×Abstract
Adipose tissue lipolysis supplies circulating FFAs, which largely meet lipid fuel needs; however, excess FFAs, can contribute to the adverse health consequences of obesity. Because “normal” FFA release has not been well defined, average (mean of 4 days) basal FFA release and its potential regulation factors were measured in 50 lean and obese adults (25 women). Resting energy expenditure (REE), but not body composition, predicted most of the interindividual variation in FFA release. There was a significant, positive linear relationship between palmitate release and REE; however, women released approximately 40% more FFA than men relative to REE. Neither plasma palmitate concentrations nor respiratory quotient by indirect calorimetry differed between men and women. Glucose release rates were not different in men and women whether related to REE or fat free mass. These findings indicate that nonoxidative FFA clearance is greater in women than in men. This could be an advantage at times of increased fuel needs. We conclude that “normal” adipose tissue lipolysis is different in men and women and that the fuel export role of adipose tissue in obesity will need to be reassessed.
Authors
Søren Nielsen, ZengKui Guo, Jeanine B. Albu, Samuel Klein, Peter C. O’Brien, Michael D. Jensen
Sassan HajMohammadi, Keiichi Enjyoji, Marc Princivalle, Patricia Christi, Miroslav Lech, David Beeler, Helen Rayburn, John J. Schwartz, Samad Barzegar, Ariane I. de Agostini, Mark J. Post, Robert D. Rosenberg, Nicholas W. ShworakSassan HajMohammadi, Keiichi Enjyoji, Marc Princivalle, Patricia Christi, Miroslav Lech, David Beeler, Helen Rayburn, John J. Schwartz, Samad Barzegar, Ariane I. de Agostini, Mark J. Post, Robert D. Rosenberg, Nicholas W. Shworak×Abstract
Endothelial cell production of anticoagulant heparan sulfate (HSact) is controlled by the Hs3st1 gene, which encodes the rate-limiting enzyme heparan sulfate 3-O-sulfotransferase-1 (3-OST-1). In vitro, HSact dramatically enhances the neutralization of coagulation proteases by antithrombin. The in vivo role of HSact was evaluated by generating Hs3st1–/– knockout mice. Hs3st1–/– animals were devoid of 3-OST-1 enzyme activity in plasma and tissue extracts. Nulls showed dramatic reductions in tissue levels of HSact but maintained wild-type levels of tissue fibrin accumulation under both normoxic and hypoxic conditions. Given that vascular HSact predominantly occurs in the subendothelial matrix, mice were subjected to a carotid artery injury assay in which ferric chloride administration induces de-endothelialization and occlusive thrombosis. Hs3st1–/– and Hs3st1+/+ mice yielded indistinguishable occlusion times and comparable levels of thrombin•antithrombin complexes. Thus, Hs3st1–/– mice did not show an obvious procoagulant phenotype. Instead, Hs3st1–/– mice exhibited genetic background–specific lethality and intrauterine growth retardation, without evidence of a gross coagulopathy. Our results demonstrate that the 3-OST-1 enzyme produces the majority of tissue HSact. Surprisingly, this bulk of HSact is not essential for normal hemostasis in mice. Instead, 3-OST-1–deficient mice exhibited unanticipated phenotypes suggesting that HSact or additional 3-OST-1–derived structures may serve alternate biologic roles.
Authors
Sassan HajMohammadi, Keiichi Enjyoji, Marc Princivalle, Patricia Christi, Miroslav Lech, David Beeler, Helen Rayburn, John J. Schwartz, Samad Barzegar, Ariane I. de Agostini, Mark J. Post, Robert D. Rosenberg, Nicholas W. Shworak
×Abstract
The dissemination of IgA-dependent immunity between mucosal sites has important implications for mucosal immunoprotection and vaccine development. Epithelial cells in diverse gastrointestinal and nonintestinal mucosal tissues express the chemokine MEC/CCL28. Here we demonstrate that CCR10, a receptor for MEC, is selectively expressed by IgA Ab-secreting cells (large s/cIgA+CD38hiCD19int/–CD20–), including circulating IgA+ plasmablasts and almost all IgA+ plasma cells in the salivary gland, small intestine, large intestine, appendix, and tonsils. Few T cells in any mucosal tissue examined express CCR10. Moreover, tonsil IgA plasmablasts migrate to MEC, consistent with the selectivity of CCR10 expression. In contrast, CCR9, whose ligand TECK/CCL25 is predominantly restricted to the small intestine and thymus, is expressed by a fraction of IgA Ab-secreting cells and almost all T cells in the small intestine, but by only a small percentage of plasma cells and plasmablasts in other sites. These results point to a unifying role for CCR10 and its mucosal epithelial ligand MEC in the migration of circulating IgA plasmablasts and, together with other tissue-specific homing mechanisms, provides a mechanistic basis for the specific dissemination of IgA Ab-secreting cells after local immunization.
Authors
Eric J. Kunkel, Chang H. Kim, Nicole H. Lazarus, Mark A. Vierra, Dulce Soler, Edward P. Bowman, Eugene C. Butcher
×Abstract
The rapid and selective accumulation of neutrophils into the lungs is thought to underlie the pulmonary failure that leads to sepsis-related death. In this study we investigated whether neutrophil TLR4 is important in LPS-induced pulmonary neutrophil recruitment by creating chimeric mice (transferring bone marrow between TLR4+/+ and TLR4–/– mice). In TLR4+/+ mice receiving TLR4–/– bone marrow, 6 weeks after transplant TLR4 was absent in all circulating leukocytes as well as in resident macrophages (these mice were termed LeukocyteTLR4–/–), and these cells were completely nonresponsive to LPS. In TLR4–/– mice receiving TLR4+/+ bone marrow, endothelial cells but not leukocytes were deficient in TLR4 (EndotheliumTLR4–/–). Surprisingly, systemic LPS (0.5 mg/kg) induced a dramatic increase in neutrophil sequestration into the lungs of LeukocyteTLR4–/– mice over the first 4 hours. Concomitantly, numbers of circulating leukocytes decreased by 90%. By contrast, EndotheliumTLR4–/– mice showed very little increase in neutrophil sequestration in the lungs, suggesting that endothelium rather than leukocyte TLR4 was important. Intravital microscopy of peripheral microcirculation in the cremaster muscle revealed about 30-fold more leukocyte–endothelial cell interactions in LPS-treated EndotheliumTLR4–/– mice than in LPS-treated LeukocyteTLR4–/– mice. This is consistent with less sequestration of leukocytes into the lungs of EndotheliumTLR4–/– mice. In conclusion, our data challenge the view that LPS directly activates neutrophils to trap in lungs and suggest a far more important role than previously appreciated for the endothelial cells.
Authors
Graciela Andonegui, Claudine S. Bonder, Francis Green, Sarah C. Mullaly, Lori Zbytnuik, Eko Raharjo, Paul Kubes
×Abstract
The extracellular calcium-sensing receptor (CaR; alternate gene names, CaR or Casr) is a membrane-spanning G protein–coupled receptor. CaR is highly expressed in the parathyroid gland, and is activated by extracellular calcium (Ca2+o). Mice homozygous for null mutations in the CaR gene (CaR–/–) die shortly after birth because of the effects of severe hyperparathyroidism and hypercalcemia. A wide variety of functions have been attributed to CaR. However, the lethal CaR-deficient phenotype has made it difficult to dissect the direct effect of CaR deficiency from the secondary effects of hyperparathyroidism and hypercalcemia. We therefore generated parathyroid hormone–deficient (PTH-deficient) CaR–/– mice (Pth–/–CaR–/–) by intercrossing mice heterozygous for the null CaR allele with mice heterozygous for a null Pth allele. We show that genetic ablation of PTH is sufficient to rescue the lethal CaR–/– phenotype. Pth–/–CaR–/– mice survive to adulthood with no obvious difference in size or appearance relative to control Pth–/– littermates. Histologic examination of most organs did not reveal abnormalities. These Pth–/–CaR–/– mice exhibit a much wider range of values for serum calcium and renal excretion of calcium than we observe in control littermates, despite the absence of any circulating PTH. Thus, CaR is necessary for the fine regulation of serum calcium levels and renal calcium excretion independent of its effect on PTH secretion.
Authors
Claudine H. Kos, Andrew C. Karaplis, Ji-Bin Peng, Matthias A. Hediger, David Goltzman, Khalid S. Mohammad, Theresa A. Guise, Martin R. Pollak
×Abstract
To understand the role of the calcium-sensing receptor (CasR) in the skeleton, we used a genetic approach to ablate parathyroid glands and remove the confounding effects of elevated parathyroid hormone (PTH) in CasR-deficient mice. CasR deficiency was transferred onto the glial cells missing 2–deficient (Gcm2-deficient) background by intercrossing CasR- and Gcm2-deficient mice. Superimposed Gcm2 deficiency rescued the perinatal lethality in CasR-deficient mice in association with ablation of the parathyroid glands and correction of the severe hyperparathyroidism. In addition, the double homozygous CasR- and Gcm2-deficient mice demonstrated healing of the abnormal mineralization of cartilage and bone associated with CasR deficiency, indicating that rickets and osteomalacia in CasR-deficient mice are not due to an independent function of CasR in bone and cartilage but to the effect of severe hyperparathyroidism in the neonate. Analysis of the skeleton of 6-week-old homozygous CasR- and Gcm2-deficient mice also failed to identify any essential, nonredundant role for CasR in regulating chondrogenesis or osteogenesis, but further studies are needed to establish the function of CasR in the skeleton. In contrast, concomitant Gcm2 and CasR deficiency failed to rescue the hypocalciuria in CasR-deficient mice, consistent with direct regulation of urinary calcium excretion by CasR in the kidney. Double Gcm2- and CasR-deficient mice provide an important model for evaluating the extraparathyroid functions of CasR.
Authors
Qisheng Tu, Min Pi, Gerard Karsenty, Leigh Simpson, Shiguang Liu, L. Darryl Quarles
×Abstract
Pseudohypoaldosteronism type II (PHAII) is an autosomal dominant disorder of hyperkalemia and hypertension. Mutations in two members of the WNK kinase family, WNK1 and WNK4, cause the disease. WNK1 mutations are believed to increase WNK1 expression; the effect of WNK4 mutations remains unknown. The clinical phenotype of PHAII is opposite to Gitelman syndrome, a disease caused by dysfunction of the thiazide-sensitive Na-Cl cotransporter. We tested the hypothesis that WNK kinases regulate the mammalian thiazide-sensitive Na-Cl cotransporter (NCC). Mouse WNK4 was cloned and expressed in Xenopus oocytes with or without NCC. Coexpression with WNK4 suppressed NCC activity by more than 85%. This effect did not result from defects in NCC synthesis or processing, but was associated with an 85% reduction in NCC abundance at the plasma membrane. Unlike WNK4, WNK1 did not affect NCC activity directly. WNK1, however, completely prevented WNK4 inhibition of NCC. Some WNK4 mutations that cause PHAII retained NCC-inhibiting activity, but the Q562E WNK4 demonstrated diminished activity, suggesting that some PHAII mutations lead to loss of NCC inhibition. Gain-of-function WNK1 mutations would be expected to inhibit WNK4 activity, thereby activating NCC, contributing to the PHAII phenotype. Together, these results identify WNK kinases as a previously unrecognized sodium regulatory pathway of the distal nephron. This pathway likely contributes to normal and pathological blood pressure homeostasis.
Authors
Chao-Ling Yang, Jordan Angell, Rose Mitchell, David H. Ellison
×Abstract
While mast cells and basophils constitutively express the high-affinity IgE receptor (FcεRI), it is absent or weakly expressed on APCs from normal donors. FcεRI is strongly upregulated on APCs from atopic donors and involved in the pathophysiology of atopic diseases. Despite its clinical relevance, data about FcεRI regulation on APCs are scarce. We show that in all donors intracellular α chain of the FcεRI (FcεRIα) accumulates during DC differentiation from monocytes. However, expression of γ chains of the FcεRI (FcεRIγ), mandatory for surface expression, is downregulated. It is low or negative in DCs from normal donors lacking surface FcεRI (FcεRIneg DCs). In contrast, DCs from atopics express surface FcεRI (FcεRIpos DCs) and show significant FcεRIγ expression, which can be coprecipitated with FcεRIα. In FcεRIneg DCs lacking FcεRIγ, immature and core glycosylated FcεRIα accumulates in the endoplasmic reticulum. In FcεRIpos DCs expressing FcεRIγ, an additional mature form of FcεRIα exhibiting complex glycosylation colocalizes with FcεRIγ in the Golgi compartment. IgE binding sustains surface-expressed FcεRI on DCs from atopic donors dependent on baseline protein synthesis and transport and enhances their IgE-dependent APC function. We propose that enhanced FcεRI on DCs from atopic donors is driven by enhanced expression of otherwise limiting amounts of FcεRIγ and is preserved by increased IgE levels.
Authors
Natalija Novak, Carmen Tepel, Susanne Koch, Klaudia Brix, Thomas Bieber, Stefan Kraft
×Abstract
During ascent to high altitude and pulmonary edema, the alveolar epithelial cells (AEC) are exposed to hypoxic conditions. Hypoxia inhibits alveolar fluid reabsorption and decreases Na,K-ATPase activity in AEC. We report here that exposure of AEC to hypoxia induced a time-dependent decrease of Na,K-ATPase activity and a parallel decrease in the number of Na,K-ATPase α1 subunits at the basolateral membrane (BLM), without changing its total cell protein abundance. These effects were reversible upon reoxygenation and specific, because the plasma membrane protein GLUT1 did not decrease in response to hypoxia. Hypoxia caused an increase in mitochondrial reactive oxygen species (ROS) levels that was inhibited by antioxidants. Antioxidants prevented the hypoxia-mediated decrease in Na,K-ATPase activity and protein abundance at the BLM. Hypoxia-treated AEC deficient in mitochondrial DNA (ρ0 cells) did not have increased levels of ROS, nor was the Na,K-ATPase activity inhibited. Na,K-ATPase α1 subunit was phosphorylated by PKC in hypoxia-treated AEC. In AEC treated with a PKC-ζ antagonist peptide or with the Na,K-ATPase α1 subunit lacking the PKC phosphorylation site (Ser-18), hypoxia failed to decrease Na,K-ATPase abundance and function. Accordingly, we provide evidence that hypoxia decreases Na,K-ATPase activity in AEC by triggering its endocytosis through mitochondrial ROS and PKC-ζ–mediated phosphorylation of the Na,K-ATPase α1 subunit.
Authors
Laura A. Dada, Navdeep S. Chandel, Karen M. Ridge, Carlos Pedemonte, Alejandro M. Bertorello, Jacob I. Sznajder
×Abstract
Comparing lymphocyte responses to allergenic and nonallergenic foods could reveal the differences between pathogenic and normal immune responses to foods. Defining the cytokine-producing phenotypes of peanut-specific lymphocytes from peanut-allergic children, children who outgrew peanut allergy, and children who have always tolerated peanuts may be useful for understanding the mechanisms of food tolerance. Investigating immune responses against foods is hindered, however, by the fact that circulating food antigen–specific lymphocytes are very rare. In a novel approach we used carboxyfluorescein succinimidyl ester to detect peanut-specific lymphocytes by flow cytometry. We confirmed that these cells are indeed peanut specific by cloning. Peanut-allergic donors show Th2 polarization of cytokine production by peanut-specific cells (IFN-γ low, TNF-α low, IL-4 high, IL-5 high, IL-13 high). Conversely, nonallergic children and children who have outgrown their allergy show Th1 skewing to peanut antigens (IFN-γhigh, TNF-α high, IL-4 low, IL-5 low, IL-13low), similarly to nonallergenic food antigens (β-lactoglobulin, OVA). This finding suggests that peanut antigens do not intrinsically induce Th2 skewing, but that the type of response depends upon the donor’s allergic status. In conclusion, food allergic status is characterized by a Th2 response whereas Th1-skewed responses underlie oral tolerance.
Authors
Victor Turcanu, Soheila J. Maleki, Gideon Lack
Rosalía Lavado-Autric, Eva Ausó, José Victor García-Velasco, María del Carmen Arufe, Francisco Escobar del Rey, Pere Berbel, Gabriella Morreale de EscobarRosalía Lavado-Autric, Eva Ausó, José Victor García-Velasco, María del Carmen Arufe, Francisco Escobar del Rey, Pere Berbel, Gabriella Morreale de Escobar×Abstract
Epidemiological studies from both iodine-sufficient and -deficient human populations strongly suggest that early maternal hypothyroxinemia (i.e., low circulating free thyroxine before onset of fetal thyroid function at midgestation) increases the risk of neurodevelopmental deficits of the fetus, whether or not the mother is clinically hypothyroid. Rat dams on a low iodine intake are hypothyroxinemic without being clinically hypothyroid because, as occurs in pregnant women, their circulating 3,5,3′-triiodothyronine level is usually normal. We studied cell migration and cytoarchitecture in the somatosensory cortex and hippocampus of the 40-day-old progeny of the iodine-deficient dams and found a significant proportion of cells at locations that were aberrant or inappropriate with respect to their birth date. Most of these cells were neurons, as assessed by single- and double-label immunostaining. The cytoarchitecture of the somatosensory cortex and hippocampus was also affected, layering was blurred, and, in the cortex, normal barrels were not formed. We believe that this is the first direct evidence of an alteration in fetal brain histogenesis and cytoarchitecture that could only be related to early maternal hypothyroxinemia. This condition may be 150–200 times more common than congenital hypothyroidism and ought to be prevented both by mass screening of free thyroxine in early pregnancy and by early iodine supplementation to avoid iodine deficiency, however mild.
Authors
Rosalía Lavado-Autric, Eva Ausó, José Victor García-Velasco, María del Carmen Arufe, Francisco Escobar del Rey, Pere Berbel, Gabriella Morreale de Escobar
×Abstract
Phosphatase and tensin homologue deleted on chromosome ten (PTEN) is part of a complex signaling system that affects a variety of important cell functions. PTEN blocks the action of PI3K by dephosphorylating the signaling lipid phosphatidylinositol 3,4,5-triphosphate. We have used a mouse model for asthma to determine the effect of PI3K inhibitors and PTEN on allergen-induced bronchial inflammation and airway hyperresponsiveness. PI3K activity increased significantly after allergen challenge. PTEN protein expression and PTEN activity were decreased in OVA-induced asthma. Immunoreactive PTEN localized in epithelial layers around the bronchioles in control mice. However, this immunoreactive PTEN dramatically disappeared in allergen-induced asthmatic lungs. The increased IL-4, IL-5, and eosinophil cationic protein levels in bronchoalveolar lavage fluids after OVA inhalation were significantly reduced by the intratracheal administration of PI3K inhibitors or adenoviruses carrying PTEN cDNA (AdPTEN). Intratracheal administration of PI3K inhibitors or AdPTEN remarkably reduced bronchial inflammation and airway hyperresponsiveness. These findings indicate that PTEN may play a pivotal role in the pathogenesis of the asthma phenotype.
Authors
Yong-Geun Kwak, Chang H. Song, Ho K. Yi, Pyoung H. Hwang, Jong-Suk Kim, Kyung S. Lee, Yong C. Lee



Copyright © 2025 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)